Imaging techniques for the evaluation of MM can be divided in three grioups:
Morphological,
which detect bone involvement,
functional that detect tumor activity; and a mixed group of the former mentioned techniques (morpho-functional techniques)
MORPHOLOGICAL TECHNIQUES
CONVENTIONAL RADIOLOGY
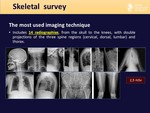
Skeletal survey is the most used imaging technique..
It includes 14 radiographies,
from the skull to the knees,
with double projections of the tree spine regions and thorax.
The total estimated radiation dose is about 2.5mSv.
Fig. 3

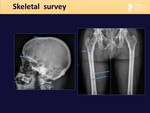
Fig. 3: Skeletal survey: display of the 14 plain radiographs of which it's composed.
This technique offers some advantages:
- Widely available
- Low cost
- Detects 50-70% of the bone lesions,
especially those with cortical and trabecular localizations Fig. 4
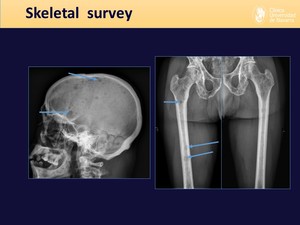
Fig. 4: Skeletal survey findings. Example of a patient with multiple lytic bone lesions (blue arrows), easily detected by skeletal survey.
But it also has many disadvantages:
Low sensitivity:
- Does not detect diffuse involvement
- High false negative rates Fig. 5
- Delayed detection of lesions
Low specificity:
- As they are 2D images there is a problem of superimposed structures
- Difficult differentiation in patients with osteoporosis
Despite all these problems,
skeletal survey is still used, if there is no other technique available,
because of its wide availability,
and prognosis impact: the presence of lytic lesions on RX is a diagnostic criteria of MM that requires immediate treatment.
CT
On the other hand,
whole body multidetector CT (TCMD) is superior to conventional radiographs at defining cortical bone lesions.
It has many advantages:
- High spatial resolution,
with good quality 3D reconstructions
- Low exploration time (64 slices in 1,5 sec.)
- It helps to guide biopsies
However it also has some disadvantages:
- Low contrast resolution,
that makes it difficult to distinguish lesions in patients with osteopenia
- High false negative rates
- High Radiation dose (up to 35 mSv)
Low dose CT is a CT performed with special parameters in order to reduce radiation exposure,
being able to reduce the radiation dose from 35 to 4 mSv Fig. 7

Fig. 7: Low-dose CT allows for a precise evaluation of patients with reduced radiation exposure.
The advantages:
• Only 4 - 5 mSv of radiation dose
• Higher sensitivity than skeletal survey (90% vs 50-70%)
• Good option for diagnosis and follow-up
The disadvantages:
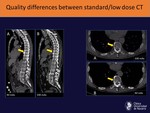
• Worse imaging quality than normal dose CT Fig. 8
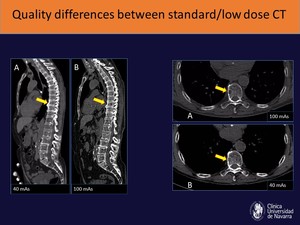
Fig. 8: In low dose studies, however, there is a reduced image quality that in most cases does not hinder our ability to detect lesions, although it makes it more challenging. In this patient, a lytic lesion in T9 is barely visible in the low dose CT (40 mAS), but clearly identifiable in the standard dose CT (100 mAs)
• Low contrast resolution
• Difficult to differentiate tumor infiltration from osteoporosis
A whole body low dose CT study has up to 1800 images to be analyzed,
representing a very time-consuming study for the radiologist.
Fig. 9
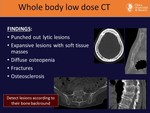
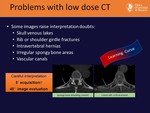
Thanks to WB CT we can identify: Fig. 10
• Punched-out lytic lesions (frequent in the skull)
• Expansive lesions with soft tissue masses
• Diffuse osteopenia
• Fractures
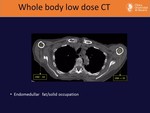
• Osteosclerosis
It is also useful at differentiating intramedullary fat from solid occupation.
Fig. 11
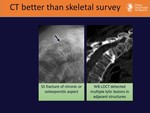
CT is globally a better technique than skeletal survey,
Fig. 12 Fig. 13,
but it has some drawbacks to take into account:
It relies on bone destruction to identify lesions,
and can't accurately depict bone marrow infiltration. Fig. 14

Fig. 14: Since CT relies on bone destruction to visualize lesions, it can't detect non-destructive bone marrow disease.
Even though the acquisition time is 5 minutes,
the analysis and image interpretation may take up to 45 min,
and the radiologist needs a learning curve to achieve good diagnostic accuracy.
Fig. 15
MRI
MRI is the last of the morphological techniques.
This technique offers many advantages:
- No radiation
- High contrast resolution
- Detects bone marrow infiltration associated or not to trabecular destruction
- Detects extra-osseous lesions
- Helps to select higher activity areas for biopsy
Disadvantages:
- Long acquisition time
- High cost
- Limiting patient factors: claustrophobia,
motion artifacts,
pacemakers etc.
- Does NOT detect bone destruction (but it detects infiltration)
- Artifacts due to ferromagnetic devices
To perform an optimal MRI studie,
some requierements must be met

Fig. 16: Whole body MRI standard sequences, and technical requierements for an optimal study.
Despite not being able to detect bone destruction,
MRI can detect five different patterns of marrow involvement: normal,
typical of monoclonal gammopathy of undetermined significance (MGUS) and detectable at diagnosis in 50–75% of patients with smoldering/Durie-Salmon stage I MM; diffuse,
seen in nearly 80% of patients with advanced disease or high tumor burden; focal or multifocal (30% of the patients); and variegated or ‘salt and pepper’,
which reflects non-homogeneous composition of bone marrow,
with fatty islands and low-grade interstitial infiltration by plasma cells.
Lesions are usually seen as hipointense on T1 sequences and hyperintense on T2 and STIR.
Pathological enhancement may also be seen after contrast administration.

Fig. 17: Diverse affectation patterns of Multiple Myeloma in MRI images.
According to the Latest recommendations of 2015,
Whole body MRI is reccomended in the following settings: Fig. 18
• For the evaluation of axial skeleton
• To assess painful lesions
• To distinguish between benign or malign fractures
• For the detection of spinal cord compression Fig. 19
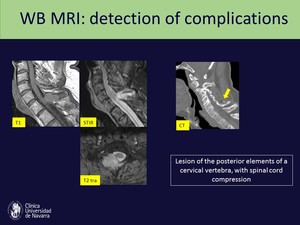
Fig. 19: MRI ability to detect medullary complications, such as in this case, in which we can observe a spinal cord compression caused by a tumoral lesion.
• To assess soft tissue involvement
• To study of MGUS and Smoldering Myeloma.
Whole body MRI is an expensive,
not widely available and time-consuming technique,
but some of these difficulties can be overcome by performing a more limited study (axial skeleton and pelvis only),
while being able to detect up to 90% of the lesions.
Fig. 20
This approach can be especially useful as a follow up study,
or to assess treatment response in known lesions.
FUNCIONTAL AND MORPHO-FUNCTIONAL TECHNIQUES
DIFFUSION WEIGHTED MRI (DWI)
DWI relies on the restricted movement of water molecules caused by the hypercellularity of MM lesions to detect them,
being able to quantify the ADC (Apparent Diffusion Coefficient),
which is an indirect measure of tumoral cellularity.
DWI sequences,
added to a conventional MRI study,
allow for a precise morpho-functional evaluation of MM patients,
with the added cost of increased study time. Fig. 21
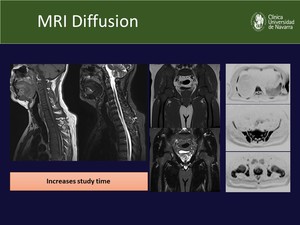
Fig. 21: MRI conventional and diffusion-weighted sequences, with the inverted diffusion images on the right column.
The diffusion images show hypercellular lesions as black areas over a white background, hard to identify on conventional images, increasing the sensitivity of the study.
PET and PET/CT
Possitron emmision tomography (PET) is a functional technique able to detect metabolic activity measuring the uptake of radiopharmaceutical agents.
At our institution,
all PET studies are merged with a CT scan performed at the same time,
since PET/CT offers several advantages compared to dedicated PET: Fig. 22
- Sequential acquisition of morpho-funtional images
- Reduced scan times compared to dedicated PET
- Attenuation correction and quantification (SUV)
- Improved lesion localization
- Higher accuracy and therapy planning
PET/CT is an invaluable tool in the evaluation of patienes with known or suspected MM with many unique features:
- Imaging of the whole body in a reasonable time frame and single procedure.
- Ability to detect both medullary and extra-medullary lesions.
- Capability to identify small osteolytic lesions with the CT despite really small tumour cell deposits (subject to partial volume effect and resolution limit of 5mm).
- Ability to assess the disease burden and distinguish between active or inactive disease and/or necrotic-fibrotic tissue,
as well as infection,
inflammation or other tumors.
- Lack of restrictions in case of renal failure or metallic devices.
Free position under the scanner (patients with bone pain)
For PET studies in MM patients, 18F-FDG is the radiopharmaceutical agent of choice.
18F-FDG is a glucose analog and it is the most widely used radiopharmaceutical agent in the diagnosis,
prognosis and treatment response assessment in different tumors.
Fig.
24
However ,
PET/CT studies have diagnostic difficulties that must be taken into account:
Potential false positive findings (PITFALLS)
- Osteoporotic fracture (vertebral body,
ribs,
sacrum)
- Stress fracture,
bone infarct (femoral head)
- Jaw osteonecrosis (biphosphonates)
- Kyphoplasty,
orthopedic devices
- Degenerative Joint Disease and arthritis process
- Bone marrow biopsy/aspiration
False-negative readings
- Diffuse bone marrow involvement
- < 5 mm lesions
- Skull lesions
- Administration of high-dose steroids (within 10 days)
18F-FDG PET/CT has diagnostic and prognostic value at all stages of the disease:
IN MM
At diagnosis
- High sensitivity and specificity in the assessment of bone damage and soft tissue masses.
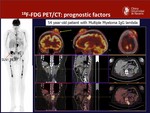
- Prognostic value: Positive findings of PET/CT at diagnosis,
(the number of focal (FL) lesions,
the intensity of tumor metabolism (SUV) and the presence of extramedullary disease (EMD)) are strong predictors of Progression-Free survival (PSF) and Overall Survival (OS).
Fig. 23

Fig. 23: Patient that shows all the prognostic factors associated with lower PFS and OS: Presence of extramedullary disease (yellow arrow), more than 3 focal lesions and SUVmax value above 4.2 (39.8)
EMD Incidence ranges from 7% to 18%,
and it is more frequent in later phases of the disease up to 60% in autopsies.
Its detection has incerased inthe last years due to the availability of more sensitive imaging techniques and the prolongation of survival.
PET/CT is able identify EMD from para-medullary/breakout lesions with high sensitivity (96%) and diagnostic accuracy.
Patientes with EMD have an extremely poor prognosis even in the novel agents era.
EMD is associated with unfavorable cytogenetic abnormalities and Gene Expression Profiling (GEP) defined high-risk MM
At relapse or progression
Negative PET/CT at diagnosis is predictive of favorable outcomes.
The number of focal lesions,
high SUVmax values and the presence of EMD Affects Time To Progression (TTP) and OS.
PET/CT influences treatment strategies in 30% of patients:
• Revealing occult sites of EMD
• Detecting sites of active disease (sensitivity of 80%)
The combination of PET/CT + laboratory data results in a 100% of specificity in predicting relapse or progression.
The evaluation of metabolic activity allows the detection of earlier relapse,
the discrimination of progressive disease from stable or non-viable disease,
serving as confirmatory imaging test in equivocal cases of progression,
thus contributing to define the prognosis of MM patients.
To evaluate response to therapy
PET/CT can evalulate the increase or decrease in metabolic activity after treatement in known lesions,
being able to determine the pressnece of progression,
partial response or complete response with higher sensitivity and specificity than CT alone. Fig. 24,
Fig. 25

Fig. 24: Complete response assessed by PET. Despite the presence of a lytic lesion in the skull detected by CT in this treated patient, PET showed no metabolic activity within the lesion, confirmed months later as complete response.
To assess minimal residual disease (MRD)
Minimal Residual Disease (MRD) is the presence of minimal uptake in lesions after treatment.
and it is categorised by the International Myeloma Working Group (IMWG) criteria. Fig. 26
Fig. 27 Fig. 28

Fig. 27: Example of a patient with MM, that after treatment still presents a lesion in the right arm, with a low metabolic activity (SUVmax: 2,2), that represents MRD.
IN SMM
- Patients who meet the criteria for SMM but have >1 lytic lesions on CT/PET are defined as having MM.
- Early data suggest that focal lesions without underlying bone changes on CT/PET are related to a higher risk of early progression from SMM to MM.
IN SOLYTARY PLASMACYTOMA
- PET/CT performance in patients with suspected SP is important to assess the extent of the tumor and confirm the diagnosis by ruling out the presence of additional occult sites of proliferating clonal plasma cells.
- PET/CT is recommended as part of the workup in patients with either EMD or SBP.
18F-FDG PET/CT vs 11C-MET PET/CT
11C-Methionine PET/CT is able to detect equal or greater number of lesions than 18F-FDG PET/CT Fig. 29,
Fig. 30

Fig. 30: Another example of the superiority of 11C-MET over 18F-FDG PET /CT in a patient with relapsed MM, in which 18F-FDG PET fails to detect most of the lesions, clearly visible with 11C-MET.