CT EXAMS: RECOMENDATION
Type of CT: Although any CT equip can be used,
a CT scanner with bigger number of detectors is expected to produce scans on which subtle details are enhanced and more easily identified.
64-detector CT offers important advantages,
such as shorter scanning times (useful in emergency) and ease of concurrent performance of CT angiography.
Isotropic data sets are produced that can be manipulated to create multiple reformatted (MPR) and three-dimensional (3D) volume-rendered (VR) CT images with great spatial resolution.
Acquisition: Slice collimation recommended is from 2.5 mm (4 slice CT) to 0.6 mm (64-detector CT).
In case of limb,
trunk or pelvis infection,
we should always make a bilateral acquisition,
in order to detect subtle changes,
specially the overall size and muscles density.
Reconstruction: 3D soft tissue rendered reconstructions (3 to 5 mm thick) should be done in the three spatial planes,
focusing on the presence of enhancement or collections.
Also,
a thin reconstruction with 1 mm collimation can be helpful if we are looking for gas bubbles.
Bone filter can be substantial to assess primary or secondary osseous pathology.
Contrast: If soft tissue infection is suspected,
the scans should be preferably done before and after the administration of intravenous iodinated contrast in portal phase.
We recommend the administration of 120 ml of contrast with an injection speed between 3 and 5 ml/s.
CLINICAL SITUATIONS: WHAT DO WE HAVE TO DO?
Patients may present with pain,
swelling,
erythema and warmth in the area of concern and other systemic symptoms like fever,
malaise or,
in extreme cases,
sepsis.
Laboratory studies such as C-reactive protein,
erythrocyte sedimentation rate and white blood cell count are often nonspecific.
Imaging evaluation is an essential part of assessment and diagnosis of musculoskeletal soft tissue infections,
even when clinically apparent,
as it provides valuable information regarding extent of involvement of deeper tissues,
anatomic structures and compartments,
and can guide intervention when needed.
We propose a schematic review of the most common clinical situations,
in a question and answer format that will help us to give an accurate diagnosis.
- WHEN do we have to obtain our CT exams?
- HOW do we have to acquire our CT exams?
- WHAT do we have to look for?
- Are we seeing any PITFALL?
- WHAT is the indicated treatment / follow-up?
CLINICAL SITUATION 1: Cutaneous swelling and erythema
- WHEN do we have to obtain our CT exams?
o When there’s a major limb size increase in a short time.
o When laboratory studies such as C-reactive protein,
erythrocyte sedimentation rate and white blood cell count show an important alteration.
o When there’s crepitation.
o When there’s suspicion of deep layers affectation (severe pain,
non-response to treatment,
quick clinical worsening...).
o When we need to demonstrate the presence of foreign bodies.
- HOW do we have to acquire our CT exams?
o First basal study,
and if we find more than only trabeculation of the subcutaneous fat we should acquire a CT in portal phase after the administration of intravenous iodinate contrast.
o We have to make an evaluation from superficial to deep.
o Basal CT
- Cutaneous thickening.
- Subcutaneous thickening and fat trabeculation.
· Without superficial fascia thickening: Cellulitis.
· With superficial fascia thickening: Cellulitis with superficial fasciitis.
Fig. 4 Fig. 5
- Thickening and/or collections in the deep fascias or fat trabeculation in the intermuscular and intramuscular septae: Deep fasciitis --> Contrast enhanced CT.
- The presence of gas along the fascial planes: Necrotizing fasciitis.
(although absence of gas does not exclude the disease).
Fig. 6
o Contrast enhanced CT
- Non-enhanced thickened fascia: Necrotizing fasciitis.
- Enlargement and decreased attenuation of the muscle: myositis.
- Intramuscular collections (myonecrosis) or abscesses if they have peripheral enhancement (pyomyositis).
Fig. 7
- Assess the permeability of the vessels to detect a potential compartmental syndrome.
- Are we seeing any PITFALL?
o Cellulitis / superficial fasciitis:
- Cardiogenic edema.
- Lymphedema.
Fig. 8
- Deep venous thrombosis.
Fig. 9
o Necrotizing fasciitis:
- Air bubbles:
· Subcutaneous injection.
· Air migration from arthroscopy.
Fig. 10
· Recent surgery.
- Absence of enhancement:
· Loss of arterial supply (thrombosis,
arterial embolism,
arteriosclerosis obliterans).
· Too early enhancement phase or technical mistakes in contrast administration.
- WHAT is the indicated treatment?
o Cellulitis / superficial fasciitis: antibiotics and close follow-up.
- If clinical worsening: repeat CT and look for necrotizing fasciitis / myositis / abscesses.
- Non-necrotizing deep fasciitis: intense follow-up (potential necrotizing fasciitis).
- Necrotizing fasciitis: RUN: immediate surgical intervention (debridement and decompression).
o Collections / abscesses: drainage if necessary.
CLINICAL SITUATION 2: Pain in an area of normal skin,
with soft tissue swelling and alteration of laboratory studies (C-reactive protein,
erythrocyte sedimentation rate and white blood cell count).
These infections have a hematogenous or iatrogenic origin (mostly implants).
- WHEN do we have to obtain our CT exams?
o When we need to differentiate a pyomyositis from a deep fasciitis (severe pain and clinical worsening).
o When we suspect the presence of collections/abscesses (where CT can also be used to guide punction-drainage).
o When we suspect bone affectation.
o When we suspect the presence of a muscular hematoma.
- HOW do we have to do acquire CT exams?
o Before and after the administration of intravenous iodinated contrast in portal phase.
- First a basal CT to better differentiate an abscess from a hematoma.
- Contrast enhanced CT in portal phase to delimitate collections / myositis,
and differentiate necrotic from viable musculature.
- WHAT do we have to look for?
o We have to make an evaluation from deep to superficial.
o Enlargement and decreased attenuation of the affected muscles with effacement of surrounding fat planes: pyomyositis.
Fig. 11
- Look for intramuscular collections (necrosis) or abscesses if they have peripheral enhancement.
- Inflammatory changes in the subcutaneous tissue and deep fascias can be present,
but the predominance of muscular involvement should help us differentiate it from an initial deep fasciitis.
- Assess vascular enhancement if there is a severe clinical alteration and increased limb size with intramuscular hypoattenuation that could reflect compartmental syndrome.
- If there is collection / enhancement adjacent to the bone: look for osteomyelitis signs.
o Periosteal reaction,
osteopenia,
medullary low/intermediate attenuation areas,
bone lysis,
endostal scalloping or focal cortical erosions: acute osteomyelitis.
Fig. 12
- Look for extramedullary fat-liquid level (rare but specific sign of osteomyelitis reflecting the presence of cortical breach),
and fistula to skin and joints.
o Central intramedullary hypodense cystic lesion with thick rim ossification,
extensive thick well-circumscribed periosteal reaction and one sclerosis around the lesion: Brodie’s abscess (subacute osteomyelitis).
o New bone growing from the periosteum (involucrum),
osseous fragments in lytic areas (sequestrum) Fig. 13 ,
and/or perforation of bone cortex through involucrum where pus escapes by (cloaca): reactivated chronic osteomyelitis.
- Look for fistulas to skin or joints and the presence of gas.
- CT is better than MR to demonstrate the presence of osseous fragments in the sequestrum sinus,
the cortical destruction and the presence of gas.
- Are we seeing any PITFALL?
o Myositis:
-Muscular hypodensity: necrotic tumor,
radionecrosis,
myonecrosis (in diabetics),
rhabdomyolisis,
rupture of Baker cyst.
- Muscular hypodensity and trabeculation of fat: other causes of generalized edema (lymphedema,
cardiogenic edema…).
- Other collections: hematoma (+/- infected).
Fig. 14
- Bursitis (+/- infected).
o Osteomyelitis:
- Other causes of endomedular occupation,
lytic lesions or periosteal reaction: tumors and pseudotumors.
Look for collections!
- WHAT is the indicated treatment?
o Antibiotics and drainage in case of muscular abscess.
o Osteomyelitis: early iv.
antibiotic therapy and surgical curettage if necessary (chronic osteomyelitis).
o Control CT after drainage only if clinical worsening.
CLINICAL SITUATION 3: Articular pain with fever and/or laboratory studies alteration.
- WHEN do we have to obtain our CT exams?
o Severe joint warmth,
swelling and stiffness with low range of motion and there is no fluid seen by ultrasound or after puncture,
to exclude other causes (fracture,
tumor).
o To evaluate soft tissue extension and bone affectation after arthritis diagnosis.
- HOW do we have to acquire our CT exams?
o Before and after the administration of intravenous iodinated contrast in portal phase.
- WHAT do we have to look for?
o We have to make an evaluation from the joint to the periphery.
o Joint effusion,
synovial enhancement (low sensitivity for the diagnosis): inflammatory vs.
septic arthritis.
o Fat trabeculation and/or collections with peripheral enhancement (abscesses) around the joint (a crucial point for its diagnosis) Fig. 15 Fig. 16 : septic arthritis and/or septic bursitis.
o Fat-fluid level (specific sign in absence of trauma).
o Osteoporosis,
bone erosions,
poorly defined joint margins and decreased joint space: subacute septic arthritis with adjacent osteomyelitis.
- Are we seeing any PITFALL?
o Joint effusion +/- synovial enhancement: inflammatory arthritis (or other causes of synovitis).
o Fluid collection in a bursal area (with a minimum distance from the joint): bursitis.
- WHAT is the indicated treatment?
o Aspiration and culture of joint fluid,
important for determining the causative organism and its sensitivity to antibiotics.
o Control CT to assess the evolution of the collections and joint destruction.
CLINICAL SITUATION 4: fever and back pain.
- WHEN do we have to obtain our CT exams?
o Although MRI is considered the modality of choice for evaluating the presence and severity of spinal infection,
CT can suggest spinal infection in emergency.
o CT scanning is most useful for characterizing vertebral osteomyelitis in patients with subacute or chronic illness.
CT scanning provides radiologic guidance for interventional procedures (ie,
biopsy,
drainage).
- HOW do we have to acquire our CT exams?
o Before and after the administration of intravenous iodinated contrast in portal phase: to depict collections or even epidural abscesses.
- WHAT do we have to look for?
o We have to make an evaluation from the vertebrae and intervertebral space to the periphery.
o Lytic fragmentations and cortical erosions in vertebral platforms,
discal hypodensity and/or intradiscal gas (although the most common cause is degenerative),
soft tissue infiltration and/or para-vertebral (clue sign): acute to subacute spondylodiscitis.
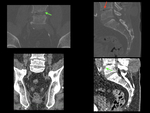
Fig. 17
o Sclerotic reaction in the margin of the bone destruction.
o Blurring of normal trabeculae.
o Loss of cortical endostal margin,
“Ivory vertebra” (diffuse sclerosis of the vertebral body): subacute to chronic spondylodiscitis.
o Collapse and deformity: chronic spondylodiscitis.
- Are we seeing any PITFALL?
o Charcot joint.
o Modic type I degenerative changes.
o Schmörl’s nodes.
o Infiltrative tumors (lymphoma…).
- WHAT is the indicated treatment?
o Treatment consists in antibiotics and,
when indicated,
surgical stabilisation of the infected segments for control of the disease and immediate mobilisation of the patients.
o Close clinical and radiological monitoring is needed.
Control CT if clinical worsening or collections drainage.