Introduction
- Pelvic floor disorders represents a common health problem
- Women are more affected
- Advanced age,
multiparty,
obesity,
smoke,
previous pelvic surgery,
constipation,
genetic factors,
heavy physical exertion contributes to this problem
- Symptoms are variable and nonspecific
- Clinical evaluation of these disorders is insufficient
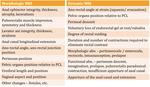
Radiologic evaluation should be preceded by:
- Clinical history – symptom duration,
severity
- Physical examination
- Clinical background - obstetric trauma,
surgeries,
inflammation,
infections,
Inflamatory Bowel Disease,
fistulas,
others
- Colonoscopy/rectosygmoidoscopy
- Functional tests
- Others
It is always imperative to exclude an organic cause,
especially involving the colon and ano-rectal compartment
MRI - advantages
- Doesn’t use ionizing radiation – no known adverse biologic effects
- High contrast resolution (High spatial and temporal resolution)
- Multiplanar imaging
- Not limited by structure interposal
- Doesn’t require retrograde opacification of the bladder
- Doesn’t require fasting and intestinal preparation
- Less operator dependent
- Higher patient acceptance
- Allows for direct and integrated study of the pelvic compartments
- Allows for a broader morphologic and dynamic study of the pelvic floor and the respective support system
MRI - limitations
- Less accessibility
- Slower examination method
- Claustrophobia
- Pacemaker
- Paramagnetic device interference
- Steep Learning curve
When to perform MRI defecography?
MRI defecography should be indicated in cases where the patient complaints or another exam provides suggestion of:
- Constipation
- Incontinence
- Defecatory dysfunction
- Rectal or anal pain
- Digitation
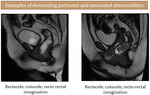
- Rectocele,
enterocele,
cistocele
- Invagination,
prolapse
In summary,
MRI defecography allows for pelvic floor anatomy and functional evaluation,
as well as their respective abnormalities,
making a precise diagnosis and provides valuable information on treatment planning.
How to perform MRI defecography?
The examination requires the use of a body phased array coil and it is performed at our institution in a 1,5 Tesla equipment,
in a closed MRI system.
There is no need for previous preparation (enema,
IV contrast,
fasting).
It is necessary to explain the process and have the patient sign an informed consent prior to examination.
It is essential to explain the procedure to the patient,
and to have access to clinical information
The following procedures are employed:
- Opacification of vagina and rectum with ultrasound Gel
- Contrast introduction is made with a 50cc syringe and a rectal catheter
- The amount of contrast introduced in the rectum varies between 150 and 250cc (depends on the patient tolerance)
- Moderately filled bladder
- Patient stays in supine position
- Use of a disposable diaper is recommended
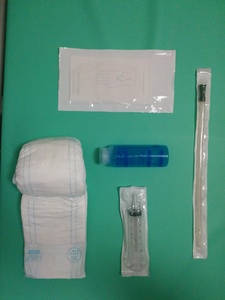
Fig. 45: MRI defecography material - gloves, diaper, ultrasound gel, syringe, probe.
Summary of the sequences performed according to our most recent protocol may be separate into anatomical and functional evaluation,
and are as follows:
- Anatomical evaluation - axial,
coronal and sagittal T2WI high-resolution images at rest for:
- pelvic support elements (muscles,
ligaments,
fascias,
bones)
- Sphincteric components
- organs (uretra,
uterus,
cervix,
vagina,
bladder,
anal canal and rectum,
in women)
- Functional evaluation - conventional sagital plans T2 Fast spin echo and sagital T2 Cine RM aquisitions:
-
Resting
-
Voluntary contraction of the perineum - valsalva and squeezing maneuvers
-
Defecation (and maximum defecatory effort)
- Post defecation resting
Every study is made in the presence of the radiologist,
who directs the exam and evaluates the images
| Sequence |
Slice orientation |
Matrix |
Slice thickness |
| T1 TSE HR |
Transversal |
320 |
3 mm |
| T2 TSE HR |
Coronal |
384 |
3 mm |
| T2 TSE HR |
Transversal |
384 |
3 mm |
| T2 TSE HR |
Sagital |
384 |
2,8 mm |
| T2 TRUFI - resting |
Sagital |
320 |
4,5 mm |
| T2 TRUFI - squeezing |
Sagital |
320 |
4,5 mm |
| T2 TRUFI Cine - defecation |
Sagital |
256 |
10 mm |
| T2 TRUFI defecation |
Sagital |
320 |
4,5 mm |
| T2 TRUFI post-def.
resting |
Sagital |
320 |
4,5 mm |
Pelvic floor unit
Retention and evacuation of the pelvic organs requires structural and functional integrity of the pelvic floor elements,
which include:
- Ano-rectal neuromuscular system
- Pelvic organs (bladder,
uterus (F) and rectum)
- Suspensory ligaments (ancorage points for muscles and viscera)
- Muscles (support,
contraction against ligaments; aperture/restraint)
- Osseous structures
- Nerves
The pelvic floor unit is a multilayer system that provides active and passive support to the pelvic structures.
A complex coordination and interaction is fundamental for pelvic floor function.
The fascia are ancoraged to the pelvic bones.
The ligaments are formed from fascia thickenings and both fascia and ligaments contribute for passive support of pelvic structures.
The active support of pelvic floor depends of pelvic muscular system. Undameged structures are necessary for maintening pelvic floor functional activity
Every pelvic compartment and structure is interdependent,
interacting and compensating each other.
MRI anatomy - Pelvic Compartments
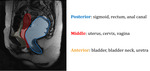
The pelvic compartments can be separated in three segments - anterior,
middle and posterior.
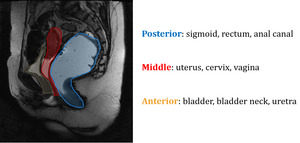
Fig. 1: Sagital slice showing the pelvic compartments
MRI anatomy - Pelvic Floor Layers
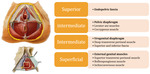
The pelvic floor support structures can be divided in four layers,
namely:
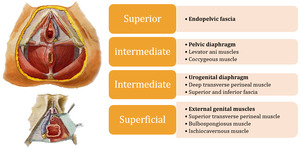
Fig. 2: Left images are adapted from - Netter FH. (2014) Atlas of human anatomy. Saunders, 6th edition.
References: Netter FH. (2014) Atlas of human anatomy. Saunders, 6th edition
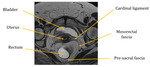
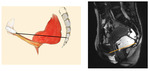
Superior (1st) Layer - endopelvic fascia:
- Adventitial layer that covers the pelvic diaphragm and envelops the pelvic organs
- It is covered by the peritoneum
- Gives support to the uterus and upper third of the vagina
- It is difficult to se on MRI - however,
there are focal areas of thickening,
named fascias,
that can be discerned
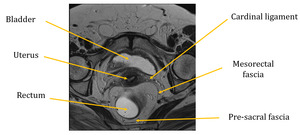
Fig. 3
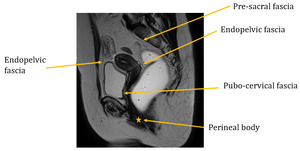
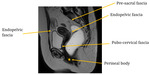
Fig. 4
Intermediate (2nd) layer - Pelvic Diaphragm
The pelvic diaphragm is composed of the ischio-coccygeous muscle and the levator ani muscles (puborectalis,
pubococcygeous and iliococcygeous).
They represent one of the main pelvic floor support layers.
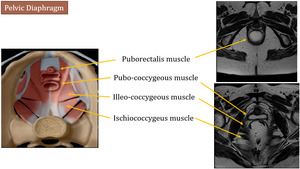
Fig. 5: Left image is adapted from Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
References: Shaaban AM, et al. (2015) Diagnostic Imaging gynecology. Elsevier
- Ischio-coccygeous muscle - forms the posterior part of the pelvic diaphragm,
attaches to the ischion and the coccyx
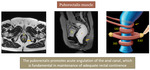
- Puborectalis muscle - arises from the pubi rami,
joins the pubococcygeous muscle and forms a sling posteriorly around the rectum
- Pubococcygeous muscle - arises from the pubic bone and attaches to the coccyx
- Iliococcygeous muscle - arises from the obturator internus fascia and inserts in the lateral aspect of the coccyx
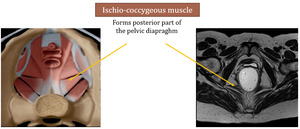
Fig. 6: Left image is adapted from Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
References: Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
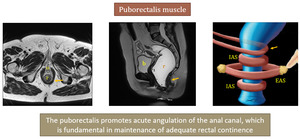
Fig. 7: b - bladder, r - rectum, u - urethra, IAS - internal anal sphincter, EAS - external anal sphincter.
Right image is adapted from Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
References: Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
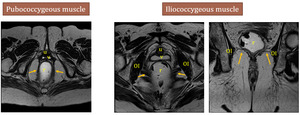
Fig. 8: OI - obturator internus, u - urethra, v - vagina, r - rectum
Intermediate (3rd) layer - Urogenital diaphragm
The 3rd layer corresponds to a fibromuscular layer that lies directly below the pelvic diaphragm,
which is triangular in shape.
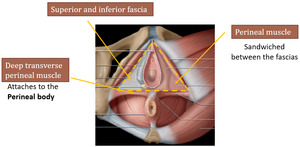
Fig. 9: Adapted from Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
References: Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
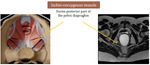
A very important element to take notice in the MRI examination is the perineal body - a fascial condensation posterior to the vagina,
attachment site of perineal muscle and external anal sphincter.
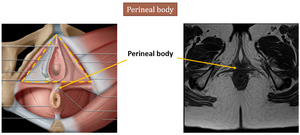
Fig. 10: left image is adapted from Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
References: Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
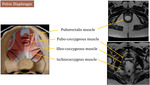
Superficial (4th) layer - External genital muscles
Most superficial of the four layers,
the extragenital muscles provide support to the inferior pelvic wall and exerts a role in sexual function.
Posterior compartment – anal sphincters
Envelops the anal canal and is composed of:
- Internal sphincter - layer of smooth muscle,
continuation of rectal muscularis propria
- Inter-sphincteric space with longitudinal smooth muscle layer
- External sphincter - with striated muscle
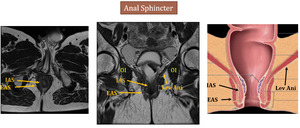
Fig. 11: Lev Ani - levator ani muscle, OI - obturator internus, IAS - internal anal sphincter, EAS - external anal sphincter
Right image is adapted from Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
References: Shaaban AM, et al. Diagnostic Imaging gynecology. Elsevier (2015)
MRI anatomy - Measurements
There are several points and lines of reference to evaluate the pelvic floor and different structures positions in the pelvis
The most used lines are the pubococcygeal (PCL) and midpubic line (MPL)
We used also the Anorectal Junction (AJR),
Anorectal angle (ARA),
H-Line and M-line.
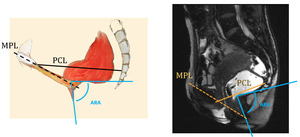
Fig. 12: Measurement lines - summary
References: Jonas
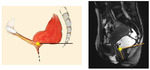
- Pubo-coccygeal line (PCL) – drawn between the inferior-posterior margin of the pubic symphysis to the anterior margin of the junction between first and second coccygeal segments; corresponds to levator plate; good correlation between PCL and classification of prolapse for anterior and middle compartments
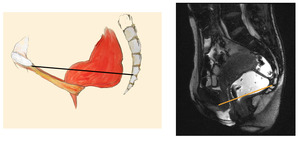
Fig. 13: Pubo-coccygeal line
References: Jonas
The PCL represents the levator plate.
Organ prolapse is measured drawing a perpendicular line below and relative to the PCL for each compartment and respective organ (bladder – anterior,
vagina – middle,
ano-rectal junction – posterior)
Perineal descent is present when it extends 3 cm below the PCL during evacuation
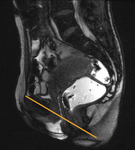
- Mid-pubic /Hymeneal line (MPL) – drawn through the longitudinal axis of the pubic bone and passing through its midequatorial point; it crosses the hymen level; moderate correlation with prolapse grading;
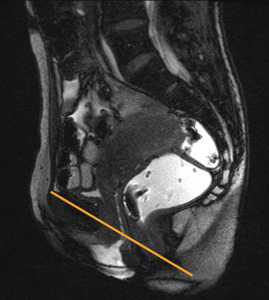
Fig. 14: Mid-pubic line
This line represents an alternative measurement to the PCL for organ prolapse assessment,
but it is mostly recommended for posterior compartment evaluation.
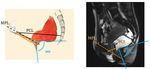
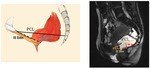
- Hiatus (H) line – drawn from the inferior margin of the symphsis pubis to the posterior margin of the puborectalis muscle sling.
- M line – extends perpendicularly from the PCL to the posterior end of the H line; allows for measurement of pelvic floor descent and subsequent grading
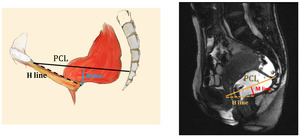
Fig. 15: M-line and H-line, relative to the PCL
References: Jonas
When there is weaking of the pelvic floor support structures,
there is consequent hiatal relaxation and widening.
The H line measures hiatal widening and the M line represents hiatal descent,
in the context of pelvic relaxation.
This measurement system,
called HMO system,
can also be used to measure organ prolapse,
which can be defined as any organ that descends below the H line
- Ano-rectal junction – the anal canal typically measures between 2,5 – 4 cm; conventional measurement of the ano-rectal junction is 4 cm from the anus or at the point of intersection of anal canal with the lower third of the rectum,
which form the ano-rectal angle
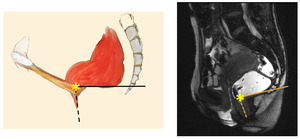
Fig. 16: Ano-rectal junction
References: Jonas
The ARJ represents the point at which posterior compartment descent and posterior organ prolapse are calculated,
whichever grading technique previously described is chosen
- Ano-rectal angle – measured from the midline of the anal canal to a tangent to the posterior rectal wall; changes in the ano-rectal angle during squeezing and defecation allow estimation of the puborectalis muscle function
Although there are established values for the ARA amplitude,
the most important factor is the variation during functional assessment,
where an ARA reduction during contraction and an increased ARA during defecation are expected,
relative to the resting study (70-134°)
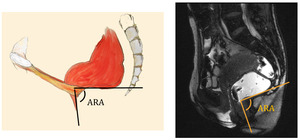
Fig. 18: Ano-rectal angle
References: Jonas
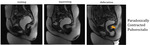
- Pubo-rectalis impression – concavity formed by the distal posterior rectal wall due to normal contraction of the pubo-rectalis muscle
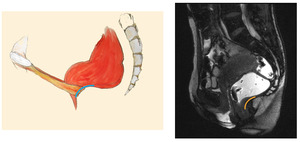
Fig. 19
References: jonas
Pubo-rectalis impression should increase during voluntary contraction and relaxes during defecation (to allow for content evacuation).
Paradoxal contraction of the puborectalis muscle during defecation is associated with ano-rectal dysfunction
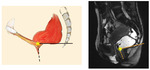
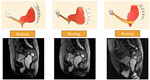
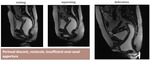
MRI dynamic evaluation - normal findings
MRI dynamic evaluation is performed in three different stages: resting,
squeezing (valsalva maneuver),
defecation.
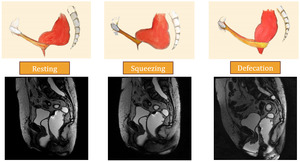
Fig. 46
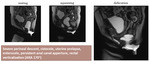
Resting
- Base of the bladder and cervix lie above the PCL
- ARJ lies 5 mm above PCL
- ARA - between 70-134°
- Anal canal is closed
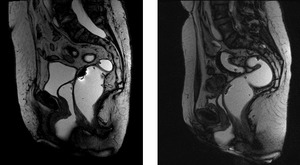
Fig. 44: Resting.
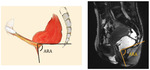
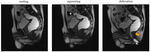
Squeezing
- Rectum horizontalization
- ARJ moves superiorly and anteriorly 10-15 mm
- ARA decreases 15-20º,
reflecting normal puborectalis contraction
- Pubo-rectalis impression increases posterior concavity of the distal rectum
- Anal canal remains closed
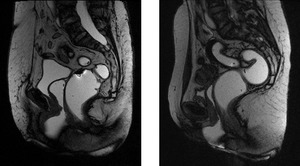
Fig. 22: Squeezing - normal MRI sagital images
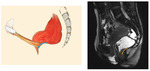
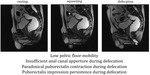
Defecation
- ARJ moves downwards (less than 3 cm) below PCL
- ARA increases,
reflecting puborectalis relaxation
- Pelvic floor descent should be less than 3,5 cm
- Anterior rectal wall becomes concave; puborectalis muscle impression is diminished
- Anal canal opens
- Rectal emptying should take less than 30 sec.
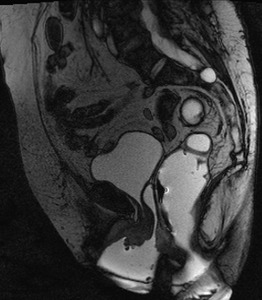
Fig. 23: Defecation - normal MRI sagital image
Anal canal apperture - measured as an anterior-posterior diameter,
during maximal defecation exertion; must be above 5 mm
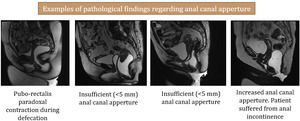
Fig. 32