Two series for evaluation of liver,
(arterial and venous) are usually used for the localization / diagnosis of hypo and hyper vascular lesions.
The purpose of this research study will be the observed concordance between the images appeared in both phases with the final objective to assess the need or otherwise of its realization,
to try to achieve this optimization of resources and protocols in the service of our hospital radiology,
as well as a decrease in the dose of radiation received by the patient.
(refer to figure 1 y 2)
Through CT,
detection capability of focal lesions is based on density differences between the focal lesion and the rest of the parenchyma.
In the liver,
the difference of intrinsic density between the hepatic parenchyma and most malignant lesions is very small and is generally necessary to administer intravenous contrast to increase these differences in density.
With conventional TC techniques,
the contrast can only be administered predominantly to parenchyma during the portal phase,
allowing an excellent detection of hypovascular lesions as metastases.
Instead,
hypervascular lesions may be captured in the same way as normal parenchyma and often are isodense during this phase.
Thanks to its high speed,
helical CT allows us to study the liver on arterial phase and portal phase,
successively.
This is what is called biphasic helical CT (1) (2-3).
(refer to figure 3)
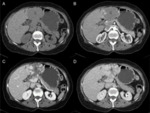
Liver scanning in arterial phase consists in studying the liver during the initial phase of the administration of contrast (from 20 s after the start of injection).
During this phase blood with contrast arrives through the arteries,
but also arrives an amount of blood four times larger via the portal vein without contrast and therefore the liver remains relatively hypodense in the arterial phase.
In the arterial phase hypervascular lesions such as hepatocellular carcinoma,
intensely capture the contrast in the context of a liver that remains relatively hypodense because it has not received yet opacified blood via the portal vein.
Hepatic scanning during the portal phase consists in studying the liver when enough opacified blood reaches the more peripheral sinusoids portals and diffuses into extravascular space.
This phase begins 60-70s after the start of injection.
During this phase the maximum parenchymal enhancement of contrast (4) is obtained.
It is during this phase when the detection of hypovascular lesions such as metastases is maximized (5) (6).
These lesions occur much more frequently than primary hepatic malignancies and have several features in the image.
Hypovascular metastases are best seen during the portal venous phase,
and may show delayed enhancement: colon,
lung,
prostate,
gastric and transitional cell carcinomas are some primary tumors resulting in hypovascular metastases (refer to figure 4).
In comparison,
hypervascular metastases are best seen during the arterial phase and often show wash on delayed images.
These metastases are typically resulting from neuroendocrine tumors (pancreatic islet cells and carcinoid tumor,...) renal cell carcinoma,
melanoma,
sarcoma and thyroid cancer (refer to figure 5-6).
This study aims to demonstrate the existing agreement between the images obtained in the arterial and venous phase of the biphasic helical CT that was performed in patients with metastatic liver disease.
Therefore it would justify the failure to complete both phases of the study and would imply a reduction of the dose received by the patient as well as a reduction in service costs.