Results
Among the prostheses studied,
22% were diagnosed as broken by MRI(n=71),
in 59 patients.
52% of broken implants were sub-pectoral,
45% sub-glandular and 4% dual-plane. The majority of implants were set 10 years before the MRI images (70%),
with a median of 14 years.
This value was 20 years for patients with bilateral rupture.
We followed 30 patients with 24 breast implants surgically replaced.
In the broken implants diagnosed group we have found 92,6% true positives.
Traumatic events,
especially car accidents,
are decisive factor in 6% of rupture.
Discussion
MRI is the gold standard for the evaluation of breast implants rupture.1 It has a high spatial and soft tissue resolution and lack of ionizing radiation.
In particular,
thanks to the ability of MRI to suppress or emphasize the signal from water,
fat,
or silicone,
it can show the smallest signal changes that could be referred to an implant rupture.4 MRI is particularly useful in case of intracapsular rupture.3
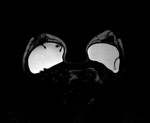
The most reliable sign on MRI for intracapsular rupture is the presence of multiple curvilinear low signal intensity lines within the T2 bright silicone,
called the “linguine sign” [Figure 1].
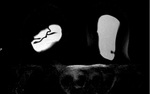
The curvilinear lines represent collapsed implant membrane floating within the silicone gel.4 Signs of minimally collapsed intracapsular rupture include the “tear drop sign” and the “key hole sign” [Figure 2].
The tear drop sign represents focal silicone invagination between the inner shell and the fibrous capsule,
with the margins of the collapsing shell in contact with one another.
The key hole represents focal invagination of silicone,
with the margins of the collapsing shell not in contact with one another. 3,
4
The “salad oil sign” or “droplet sign” refers to one or multiple focal hypointensities in T2 bright silicone. It is important to note that this finding can be “normal” post implant placement without apparent rupture as occasional small droplets of water or small amounts of air can be identified within the silicone implant [Figure 3].
3
Radial folds are uninterrupted hypointense lines characterized by a double layer,
which extend almost perpendicularly inwards from the implant surface and end blindly inside the lumen [Figure 2].
These folds are a common finding in intact implants.
Complex radial folds differ from the above in that they are longer and often have a multidirectional course.
They represent a normal finding,
although the possibility of early implant rupture cannot be excluded,
especially when associated with other signs [Figure 4].
5
In the literature,
we found variable prevalence of intracapsular signs of rupture,
(77-89%).
We had a similar percentage in our study: 76%.
However we had just a 22% MRI diagnosis of rupture,
both intracapsular and extracapsular,
versus a 55% in the most recent study.
6 This difference can be explained by a less accurate patients selection in our study,
with the use of MRI not fully justified by the clinical examination.
About the time of implants,
we found that an older prosthesis is related to a greater probability of bilateral rupture,
but we didn't find similar study in literature. 7
In our study the percentage of true positive was 92,6%,
that is a better results than most similar papers.
5
The main limitation of our study was the difficulty to find information about the follow-up; another limitation was the retrospective analysis,
that doesn’t allow to know elements of the medical history in the first place.