Keywords:
Musculoskeletal joint, Musculoskeletal system, Musculoskeletal soft tissue, MR, PACS, Contrast agent-intravenous, Diagnostic procedure, Technical aspects, Arthritides, Inflammation
Authors:
J. C. van den Noort, C. den Harder, C. Lavini, J. Huguet, P. F. C. Groot, A. J. Nederveen, M. Maas; Amsterdam/NL
DOI:
10.1594/ecr2018/C-0043
Methods and materials
A framework was developed using a secure,
stand-alone server (HP ProLiant DL380p Gen8,
2x Intel® Xeon® CPU E5-2690,
256GB RAM).
On the server,
the software packages XNAT [8] (www.xnat.org) for dataflow and Matlab (R2012b,
MathWorks,
Natick,
MA,
US) for algorithm coding and execution were installed.
Images were acquired on a 3T MRI scanner (Ingenia,
Philips Healthcare,
Best,
Netherlands),
using a field of view of 256×256mm,
TR 3.7ms,
TE 1.9ms,
flip angle 12°,
and temporal resolution 6.2s.
After acquisition,
image data were automatically exported to a DICOM-node on the server.
In the DICOM-node,
the suited DCE-MRI scans were automatically selected based on the scan protocol name.
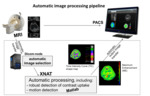
These data were automatically routed to an image processing pipeline framework based on XNAT (Figure 1).
A validated algorithm was used for data analysis [1] with pre-determined settings.
First,
the time-point of contrast agent injection was automatically determined.
Then,
for each pixel,
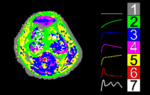
the algorithm assigned one of seven possible TIC-shape categories,
represented by seven colors,
resulting in a 3D TIC-shape map (Figure 2).
Additionally,
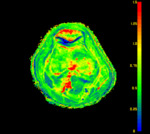
a maximum enhancement (ME) value was calculated for each pixel by dividing the maximum pixel intensity over time by the baseline intensity before start of injection,
resulting in a 3D ME map (Figure 3).
Next to each map,
a legend was included to support interpretation.
All maps were stored in XNAT (for quality inspection) and automatically forwarded to PACS (Agfa) for diagnosis.
In PACS,
the radiologists were able to interact with the 3D maps,
using zoom and scroll functions to go through the different slices.
To assess the satisfaction of the radiologists about the speed of the process,
the presentation of and interaction with the results in PACS,
a questionnaire was developed with seven statements using a Likert scale (i.e.
strongly disagree,
disagree,
neutral,
agree,
and strongly agree).
Five radiologists,
experienced in musculoskeletal imaging,
filled in the questionnaire using the results in PACS from two JIA patients.