Caroli disease is a rare congenital disorder with autosomal recessive inheritance pattern [1,2].
The disease belongs to a spectrum of fibropolycystic liver disease which result from in utero ductal plate malformation [3].
Caroli disease versus caroli syndrome:
Two form of Caroli disease have been described [4],
[5-8]:
- Simple/Isolated type: Large bile ducts are affected and it is characterized by cystic dilatation of intrahepatic bile ducts that is often limited to one lobe (usually left lobe).
However extra hepatic bile ducts involvement may exist.
- Complex type (also known as caroli syndrome): Both central intrahepatic bile ducts and the ductal plates of the smaller peripheral bile ducts are affected,
with the latter leading to the development of hepatic fibrosis.
Caroli syndrome is associated with congenital hepatic fibrosis,
portal hypertension and polycystic kidney disease.
Pathogenesis:
Several pathological hypotheses have been proposed and these include: neonatal occlusion of the hepatic artery,
leading to bile duct ischemia and cystic dilatation; abnormal growth rate of the developing biliary epithelium; and the lack of normal involution of ductal plates resulting in epithelium-lined cyst surrounding the portal triads [9,
10].
Clinical Presentation:
The manifestation of the disease depends on the level of the biliary tree which is affected.
The clinical onset usually occur in childhood or young adulthood.
Calroli disease manifests as recurrent attacks of cholangitis while patient with caroli syndrome presents with sign of portal hypertension including splenomegaly and hematemesis from esophageal varies.
Association:
Caroli's disease is a member of the family of fibrocystic ductal plate diseases to which the following diseases are usually belong:
- Congenital hepatic fibrosis (CHF): An autosomal recessive inherited disease with 56% being sporadic [11].
It is usually associated with renal tubular ectasia found in autosomal recessive polycystic kidney disease (ARPKD) and may also be accompanied by biliary malformation such as caroli’s disease and choledochal cyst [12].
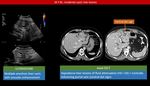
Ultrasonography is preferred imaging modality which demonstrates: Increase parenchymal echogenicity of the liver,
hypertrophy of the left lateral segment and caudate lobe,
hypertrophic left medial segment (contrary to cirrhosis) ,
hepatosplenomegaly,
intrahepatic bile duct dilatation +/- stone (caroli’s disease),
portal hypertension and cavernous transformation of portal vein.
- Renal disease: Caroli's syndrome may have the same renal malformations that are associated with isolated autosomal recessive congenital hepatic fibrosis (CHF).
They range from medullary collecting ducts ectasia resembling medullary sponge kidney [13] to dilatation of both the medullary and cortical collecting tubules [14] and autosomal recessive polycystic kidney disease ARPKD.
» Medullary sponge kidney: Usually bilateral.
CT urography nicely demonstrates the characteristic imaging findings including: striated nephrogram,
cystic dilatation of the renal tubules,
medullary nephrocalcinosis and medullary cysts.
» Autosomal Recessive Polycystic Kidney Disease (ARPKD) & rarely Autosomal Dominant Polycystic Kidney Disease (ADPKD): ARPKD is marked by smooth enlargement and increase echogenicity of both kidneys and multiple small renal cysts which usually form in utero. As mentioned earlier there is an association between ARPKD and CHF,
with the latter being progressive and inversely proportional to the age of presentation.
Imaging findings:
- Ultrasound: Sonographic findings are usually non-specific and include presence of multiple intrahepatic anechoic cystic areas in which fibrovascular bundles,
stones or septum may be present.
The fibrovascular bundles represent the portal veins and hepatic arteries which are demonstrated on Doppler scan [15].
The liver parenchyma may shows coarse echotexture if hepatic fibrosis established along with features of portal hypertension.
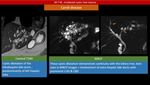
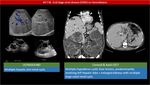
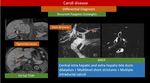
- CT scan: Multiple cystic lesion of fluid attenuation.
Central dot sign: a pathognomic findings characterized by enhancing fibrovascular bundle within the dilated intrahepatic bile duct [16].
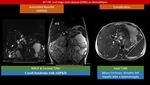
- Magnetic Resonance Imaging and Magnetic Resonance Cholangiopancreatography ( MRI/MRCP): Communication of the intrahepatic cysts with the biliary tree is the key feature of the diagnosis and ability to demonstrate the intrahepatic ductal anatomy makes MRCP a reliable diagnostic tool in Caroli’s disease,
providing that acceptable image quality can be maintained [17].
The disease manifestoes as diffuse,
lobar or segmental saccular dilatation of the intrahepatic bile ducts that communicate with the biliary tree [2,
9].
- The diagnosis is more difficult to establish in case of fusiform dilatations of the biliary tracts and Endoscopic retrograde cholangiopancreatography (ERCP) is the gold standard in this situation [15].
Complication:
- Intraductal sludge and calculus.
- Recurrent cholangitis is a common complication leading to segmental luminal narrowing and strictures.
- Liver abscess.
- Biliary cirrhosis and portal hypertension.
- Liver failure.
- Risk of malignancy: Cholangiocarcinoma may be present as a late complication in 7% of patients [15,18].
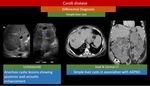
Differential Consideration:
1. Simple hepatic cysts,
(Figure 7) : benign liver lesions which are usually discovered incidentally and almost always asymptomatic.
Certain diseases such as polycystic liver disease and polycystic kidney disease are associated with multiple hepatic cysts.
They are usually multiple in numbers,
vary in size and can occur anywhere in the liver with right hepatic lobe predication. Common features include: round or oval shaped cystic lesions,
anechoic and posterior wall enhancement in U/S,
fluid attenuation (HU 0-15) on CT scan and show no enhancement after administration of I.V contrast.
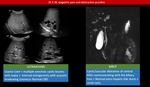
2. Biliary hamartoma (von Meyenburg Complex),
(Figure 8) : benign congenital hepatic lesions comprising of dilated small bile ducts surrounded by fibrous stroma [19].
On imaging,
biliary hamartomas present as multiple,
small (< 15 mm),
round or irregular scattered cysts with a predilection for the subcapsular region.
Being less than 15 mm is the differentiating features from the simple hepatic cyst that tend to be larger.
The ultrasound findings are variable because of the small size and variable histological components of these lesions.
Cysts might appear anechoic,
hypoechoic,
or hyperechoic in ultrasound and show features of simple cyst in CT and MRI.
In most cases,
biliary hamartoma dose not enhance after I.V contrast administration and thin rim enhancement has been described likely due to compressed adjacent liver parenchyma [20].
The lack of communication with the biliary system helps to differentiate biliary hamartomas from Caroli disease.
3.
Polycystic liver disease (PCLD): a hereditary condition that may arise either in patients with ADPKD or in patients with a different genetic mutation that results solely in autosomal dominant polycystic liver disease.
Histologically there are two types of cyst [21]: intrahepatic cyst and peribiliary cyst.
The intrahepatic cysts are more common,
arise from von Meyenburg Complex and mostly peripherally located ranging from a few millimeters into 80 mm.
4.
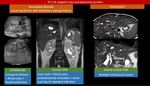
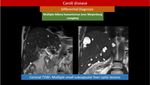
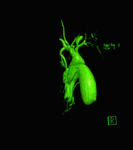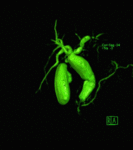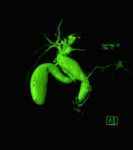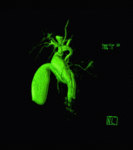
Recurrent pyogenic cholangitis (also known oriental cholangitis),
(Figure 9) : complex disease that is characterized by intrahepatic pigmented stones and recurrent attacks of cholangitis.
MRI is the ideal tool of imaging modality demonstrating: central intrahepatic and extrahepatic biliary dilatation,
multilevel short strictures,
reduced arborization and abrupt tapering of peripheral ducts [22] and intraductal pigmented calculi.
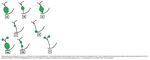
5. Choledochal cyst,
(Figure 10& 11): Is a rare congenital anomaly of the bile duct resulting in cystic or fusiform dilatation of the intrahepatic bile ducts,
extra hepatic bile ducts or both.
Choledochal cysts are classified into five basic types according to the Todanisystem.