We report two cases of Gliosarcoma diagnosed in the department of radiology of the university hospital of Fez during the last four years; the diagnosis was confirmed by a histological study.
Case 1:
43-year-old male patient,
without any pathological history,
admitted for right hemiparesis.
The symtomatology goes back to 4 months by the progressive installation of an intracranial hypertension syndrome made of headaches and vomiting.
This symptomatology was aggravated 02 months later by the installation of a heaviness of the right hemi-body with behavioral disorders,
without notion of seizures or associated visual disturbances.
Clinical examination at admission found a conscious patient,
his Glasgow (GCS) score was 15,
he had a right proportional hemiparesis and dysarthria on neurological examination.
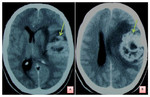
Cerebral CT (Figure 1) revealed the presence of a left temporal process,
measuring 5x4 cm in diameter,
heterogeneously enhanced after injection of the contrast,
with a necrotic central component,
and surrounded by perilesional edema.
Determining a mass effect on medial line structures with falcorial involvement and dilation of the right lateral ventricle.
Cerebral MRI (Figure 2) noted the presence of a left intraparenchymal temporal tumor,
with central necrosis,
heterogeneously enhanced after injection of the contrast and surrounded by perilesional edema.
The patient was operated; he had a total excision of the tumor whose pathological examination was compatible with a gliosarcoma.
Subsequently; the patient received 30 sessions of external radiotherapy,
with a clear clinical improvement.
After a follow-up of four years,
the patient is still autonomous with a discreet right hemiparesis allowing walking,
and does not show any clinical signs that may suggest tumor recurrence.
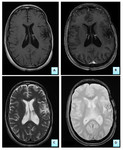
Radiographically,
recently cerebral MRI (Figure 3) and thoraco-abdominopelvic CT showed no evidence of tumor recurrence or visceral secondary localization.
Case 2:
53-year-old male patient with no particular medical history,
admitted to emergency for intracranial hypertension syndrome associated with a right hemibody heavy and seizures.
The clinical examination at admission found a patient obnubile; having a Glasgow score of 12,
with right hemiplegia and facial paralysis.
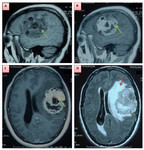
Brain CT revealed an intraaxial lesion on the left frontal lobe,
measuring 35 mm of diameter,
with ring-enhancement after contrast,
surrounded by perilesional edema and a mass effect on the median structures line (Figure 4).
The appearance of the lesion evoked either a glial tumor or an infectious process such as abscess or tuberculoma.
Cerebral MRI complement was performed showing a left frontal intraparenchymal process hypointense on T1-WI,
hyperintense on T2-WI,
heterogeneously enhanced after injection of gadolinium,
surrounded by perilesional edema and determining a mass effect on the midline evoking a high grade glioma (Figure 5).
The diagnosis of a left frontal tumor was then retained and the patient benefited from a complete surgical excision of the tumor.
The postoperative course was favorable with an early recovery of the motor deficit.
The histological study was in favor of gliosarcoma (Figure 6).
The patient was then referred to radiotherapy where he received 30 sessions (60 Gray)
One month after the end of the radiotherapy,
the patient presented multiple scalp swellings next to the irradiation field that ulcerated later (Figure 7).
The cerebral CT scan,
done at the end of radiotherapy,
revealed tumor recurrence (Figure 8).
The patient died 4 months after the end of radiation therapy.