ABI involves different stages of severity,
from mucosal to transmural involvement - with different prognosis – and may have different pathogenesis which affects imaging features [1-3]:
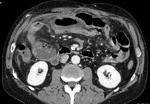
Bowel wall thickening is a typical feature of veno-occlusive disease (due to reduced outflow),
or hypoperfusion states,
and it’s due to mural edema and/or hemorrhage - the presence and degree of bowel wall thickening does not correlate with the severity of ischemic bowel wall damage [1-3].
On the contrary,
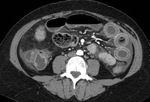
arterial occlusive ischemia presents as “paper thin walled” due vascular volume loss and reduced muscular tone [1-3].
Lumen dilatation and/or air-fluid levels may be present in ABI (and less commonly in reversible bowel ischemia).
They are caused by disruption of the normal peristalsis,
both as a reflex to ischemic injury or by irreversible and transmural ischemic damage to the bowel wall - ischemic injuries in a still viable bowel segment instead usually leads to spastic contractions,
which are most commonly observed in the colon with only mild mucosal ischemia [1].
Abnormal intraluminal pressure from mechanical intestinal obstruction may cause bowel ischemia itself.
ABI may lead to additional fluid exudation into the lumen of ischemic bowel segments - gasless loops.
This feature,
despite being non-specific,
increases the suspicion of ischemic injury [1].
Bowel wall attenuation must be evaluated when dealing with suspected ABI: hypo-density in non-contrast scan due to edema (usually homogeneous attenuation,
which is more commonly detected in veno-occlusive disease),
or hyper-density due to intramural hemorrhage [1].
In ABI conditions,
hyperemia and/or hyperperfusion may be present as well,
that's why it is important to perform a non-contrast examination before contrast media administration,
since differentiation between these findings and acute intramural hemorrhage may be difficult.
Hyperemia of ischemic loops without hyperperfusion is typically encountered in cases of veno-occlusive disease and associated outflow obstruction,
whilsts hyperperfusion of ischemic bowel segments is typically detected during reperfusion following occlusive or non-occlusive ABI or as a result of superinfection and inflammation [1].
Contrast-enhanced CT scan allows to directly detect emboli and thrombi as defects in the mesenteric arteries and their branches (in this case,
the diameter of the superior mesenteric artery is often larger than that of the superior mesenteric vein) [3]
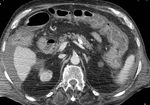
Mesenteric fat stranding and ascites are frequently associated,
but they are not specific for ABI and their presence and degree does not correlate with the severity of ischemic bowel wall damage [1,3].
When watershed areas like ileo-cecal tract,
splenic flexure or rettosigmoid junction are involved,
hypoperfusion states should be suspected,
especially in elderly patients [1-3]
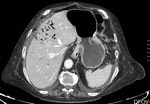
In case of severe ischemia,
pneumatosis and porto-mesenteric gas are reported - caused by the disruption of the normal bowel permeability,
often associated with bacterial overgrowth – and they dramatically change patient’s prognosis.
These findings are less common but more specific of acute bowel ischemia [1].