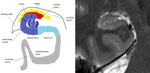
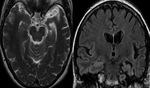
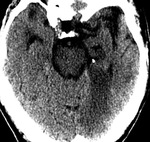
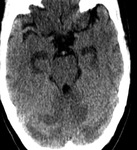
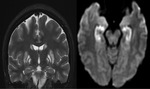
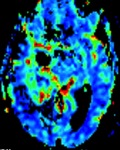
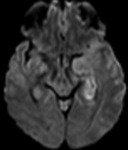
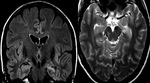
We have reviewed the principal characteristics of the hippocampus anatomy and the most usual diseases affecting it,
which includes: degenerative diseases (Alzheimer disease,
in which the hippocampus is one of the brain regions affected earlier,
and frontotemporal dementia),
vascular pathology (ischemic stroke,
hypoxic-isquemic encephalopathy,
transient global amnesia),
anatomical variants (remnants cysts of hippocampal sulcus),
tumors (glioma,
glioblastoma multiforme),
infectious disease (encephalitis HSV1),
and pathology associated with epilepsy (mesial temporal sclerosis,
status epilepticus).
Fig.
1-3
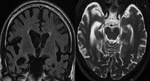
Alzheimer disease (Fig.
4)
We can use the NECT for the screening to exclude potentially reversible or treatable causes of dementia,
evaluate the medial temporal lobe atrophy which is the earliest finding on CT,
and evaluate generalized cortical atrophy which is the latest finding.
The current role of MRI is to exclude other causes of dementia,
identify region-specific patterns of brain volume loss and identify imaging markers of coexistent disease such as amyloid angiopathy.
- T1WI is used to assess the structure and define the atrophy patterns.
We can use the High resolution T1WI for volumetric analysis.
We have to evaluate if there thinned gyri,
widened sulci or enlarged ventricles.
Also probe if there is medial temporal lobe disproportionately affected,
with an average hippocampal volume reduction of 20-25%.
- T2*GRE is used to detect microhemorrhages or amyloid angiopathy.
- Perfusion MR: in which we can see a reduction in the blood volume in the temporal and parietal regions.
Frontotemporal dementia (Fig.
5)
- The role of the NECT is to evaluate the presence of frontal lobe atrophy which often is the most prominent feature,
and consider if there is an increased size of frontal horns (larger than rest of lateral ventricles).
- In MRI we can see on T1WI the atrophy of frontal and temporal lobes,
“Knife-like” gyri with normal signal,
the dilated frontal sulci reflecting atrophy,
and the relative sparing of parietal and occipital lobes.
And on T2WI and FLAIR we can see some hyperintense areas in frontotemporal white-matter.
Acute ischemic stroke (Fig.
6)
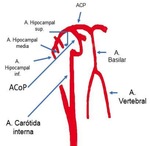
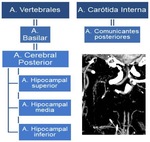
- The acute ischemic strokes that affect the hippocampus are caused by occlusions of the arterial supply from anterior choroidal artery and/or posterior cerebral artery (PCA) hippocampal branches.
The infarcts from arterial supply are usually associated with other infarcts in PCA territories.
- In NECT,
we can see hyperdense vessel which represents acute thrombus in cerebral vessel ("Dot" sign: Occluded MCA branches in sylvian fissure),
the loss of gray-white matter distinction,
the obscuration of deep gray nuclei,
the loss of cortical "ribbon",
and parenchymal hypodense areas.
In 15-45% of cases we can see the hemorrhagic transformation (hyperdense areas).
- With Perfusion-CT,
we assess the ischemic core (high MTT,
low CBF and normal CBV) vs.
penumbra (high MTT,
low CBF and CBV) determining if the patients can benefit from revascularization techniques.
- Finally with Angio-CT,
we have to look for occlusion of the vessel(s) and the presence of slow flow or collateralization.
Hypoxic-ischemic encephalopathy (Fig.
7-8)
- The injury patterns are highly variable depending on brain maturity,
severity and length of insult.
- In mild to moderate stages we can see infarcts in the watershed zones.
- In severe stages we can see the affection of the grey-matter structures such as basal ganglia,
thalami,
cortex,
cerebellum or hippocampi.
- MRI is the best image technique to assess overall extent of injury within hours after Hypoxic ischemic injury event
- The DWI is the first modality to be positive within hours showing restriction in deep nuclei and cortex.
- In T2WI and FLAIR we can see areas of hyperintensity in the cerebellum,
the basal ganglia or in the cortex.
Transient Global Amnesia
- Sudden memory loss without other signs of cognitive or neurologic impairment that recovers completely within 24 hours.
- In NECT and CECT it usually has no pathologic findings.
- In MRI appears as normal in T1WI,
in T2WI and FLAIR it normally appears as normal,
but sometimes we can see as small hyperintense foci but are typically reversible.
In Diffusion-weighted imaging (DWI) we can see tiny "dots" of restricted diffusion in hippocampus in 80% of cases.
- The Perfusion-weighted imaging (PWI) can be negative to visual inspection,
but it can show hypoperfusion,
with low CBF,
CBV in both hippocampus and thalamus compared to normal.
Hippocampal Sulcus Remnant Cysts
- They are a normal anatomic variant and are not associated with atrophy or dementias.
- They are originated because of an incomplete fusion of cornu ammonis and dentate gyrus during embryonic rolling,
leaving sulcal remnant space.
- They are seen as cysts lesions along lateral hippocampus on axial images,
with “string of pearls” appearance.
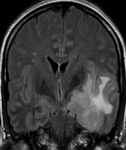
Glioma (Fig.
9-10)
- The glioma sometimes can affect the hippocampus and is seen as an homogeneous mass with hypointense signal in T1WI,
hyperintense in T2WI and FLAIR,
it does not show restriction in DWI,
and the most frequent appearance in T1FatSat sequences after gadolinium administration is the absence of enhancement.
If there is enhancement,
it suggests a higher grade glioma.
- It can have a mass effect,
and it is strange if it has calcification,
cystic or bleeding areas.
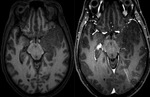
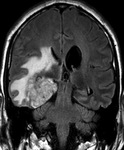
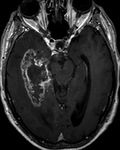
Glioblastoma Multiforme (Fig.
11-13)
In NECT we see an irregular isodense or hypodense mass with central hypodensity representing necrosis,
with marked mass effect and surrounding edema/tumor infiltration,
and hemorrhage is not uncommon.
In CECT we see a strong,
heterogeneous,
irregular rim enhancement.
In MRI this neoplasm can with following findings:
- In T1WI as an irregular isointense/hypointense WM mass in T1WI,
and we also can see necrosis,
cysts or thick irregular margin.
- In T2WI and FLAIR as a heterogeneous,
hyperintense mass with adjacent tumor infiltration/vasogenic edema.
Also can appear with necrosis,
cysts,
hemorrhage,
fluid/debris levels,
flow voids (neovascularity).
It is important to know that the viable tumor extends far beyond signal changes.
- In T2*GRE we can see a susceptibility artifact related to blood products.
- DWI shows lower measures of ADC than low-grade gliomas,
with variable diffusion restriction in solid portions of the tumor.
- PWI shows an elevated maximum relative cerebral blood volume compared to low grade,
with elevated permeability compared to low-grade tumors.
- After gadolinium administration we can see in T1WI a typical thick,
irregular rind of enhancement surrounding central necrosis.
Sometimes this enhancement can show solid,
ring,
nodular,
or patchy appearance.
- And finally,
in MRS we can see a decreased NAA,
with elevated choline,
and a lactate/lipid peak of 1.33 ppm.
Herpes encephalitis
- Brain parenchyma infection caused by herpes simplex virus type 1 (HSV1),
and typically appears as a reactivation in immunocompetent patients.
- The best imaging clue is a cortical-subcortical hyperintensity with relative white matter sparing specially affecting the limbic system (medial temporal and inferior frontal cortex) with DWI restriction.
- Typically shows an asymmetric bilateral disease with deep gray nuclei sparing.
- In T2*GRE we can see hypointensity "blooms" within edematous brain if there is haemorrhage.
- After Gadolinium administration we can see a mild,
patchy enhancement in early phases,
and gyriform enhancement usually one week after the initial symptoms.
Status epilepticus (Fig.
14)
- Transient cerebral edema,
with gray matter involvement and sometimes has also subcortical affection with mild mass effect.
- It can affect the hippocampus,
the splenium of the corpus callosum,
the thalamus and the basal ganglia.
- In MRI we can see restricted diffusion on DWI,
variable enhancement in T1FatSat after gadolinium administration,
with marked hyperemia in the Perfusion sequences.
- MRI findings can be irreversible in prolonged and severe seizures (in cases of atrophy,
laminar cortical necrosis,
or in mesial temporal sclerosis).
Mesial Temporal Sclerosis (Fig.
15)
- Mesial Temporal Sclerosis is the most frequent cause of complex partial epilepsy in adults.
- It has an unknown etiology,
although it is associated with prolonged febrile seizures.
- It has a specific pattern of atrophy of the hippocampus with gliosis,
showing increased T2 signal and loss of internal architecture.
- Approximately the 20% of the patients have bilateral affection from the disease.
- And some associated findings are ipsilateral mammillary body and fornix atrophy,
increased gliosis,
and atrophy of amygdala and parahippocampal gyrus.