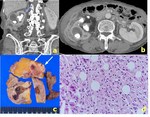
Xanthogranulomatous inflammatory disease is a rare chronic,
aggressive disease pathologically characterized by the formation of soft,
yellow nodules,
which are composed foamy,
lipid-laden macrophages (Fig 1).
Several hypotheses have been proposed including defective lipid transport,
hemorrhage,
immunologic disorders,
reaction to a specific infectious agent of low virulence,
and lymphatic obstruction.
It is commonly seen in the gallbladder and kidney,
where it is referred to as xanthogranulomatous cholecystitis and xanthogranulomatous pyelonephritis.
However,
xanthogranulomatous inflammatory disease also occurs in various organs such as the pancreas,
stomach,
colon,
appendix,
urachus,
urinary bladder,
retroperitoneum and female genital organs.
Xanthogranulomatous cholecystitis
Xanthogranulomatous cholecystitis is a rare chronic inflammatory disease of the gallbladder.
It commonly occurs in the fifth and sixth decades.
Diabetes combined with hypoalbuminemia may be an important factor in xanthogranulomatous cholecystitis.
Patients with xanthogranulomatous cholecystitis present with signs and symptoms of cholecystitis,
including right upper quadrant pain,
vomiting,
jaundice,
and leukocytosis.
On physical examination,
the patient may have a positive Murphy’s sign and palpable right upper quadrant mass.
Sonography shows hypoechoic intramural nodules or a hypoechoic band surrounding the gallbladder.
The hypoechoic nodules represent abscess,
xanthogranulomas,
or a combination of both.
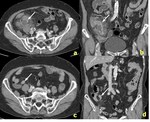
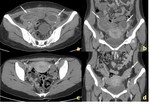
CT and MRI features are similar to the sonography,
showing intramural nodules,
thickened gallbladder wall,
gallstones and ductal dilatation (Figs 2,3).
Histopathologically,
xanthogranulomatous cholecystitis is thought to be initiated after rupture or occlusion of Rokitanski-Aschoff sinuses or small ulceration in the gallbladder mucosa with subsequent intravasation of bile into the gallbladder wall,
causing an inflammatory response where macrophases phagocytose the biliary lipids in the bile with resultant formation of xanthoma cells.
Complications associated with xanthogranulomatous cholecystitis include gallbladder perforation,
abscess formation,
fistulous tract formation to the duodenum or skin,
invasion into the liver or colon and Mirizzi syndrome.
Xanthogranulomatous pancreatitis
Xanthogranulomatous pancreatitis is an extremely rare form of chronic pancreatitis and results from a combination of duct obstruction,
infection,
and repeated hemorrhage as is seen in the kidney and gallbladder.
Xanthogranulomatous pancreatitis presents as either a solid or a cystic lesion and can have variable imaging findings according to the parenchymal changes.
The differential diagnosis includes pseudocysts,
mucinous cystic neoplasm,
cystic neuroendocrine tumor,
intraductal papillary mucinous neoplasm,
oligocystic serous cystadenoma,
and solid pseudopapillary neoplasm.
Xanthogranulomatous appendicitis
Xanthogranulomatous appendicitis is a rare inflammatory disease and is usually seen in patients with interval appendectomy.
Delayed or interval appendectomy specimens often have a characteristic pattern that includes granulomas,
xanthogranulomatous inflammation,
mural fibrosis/thickening,
and transmural chronic inflammation.
Sonography and CT show periappendiceal abscess,
a large soft tissue mass or enlarged appendix without inflammation (Fig 4).
It is not possible to differentiate xanthogranulomatous appendicitis from an infiltrative cancer because xanthogranulomatous appendicitis might present as a mass like lesion with an extension of fibrosis and inflammation to the surrounding tissues,
mimicking an infiltrative cancer.
Xanthogranulomatous inflammation of peritoneum
Xanthogranulomatous inflammation of the peritoneum has not been reported.
In our case,
a 77-year-old man with a history of cholecystectomy for GB cancer was confirmed of xanthogranumatous inflammation of the peritoneum by surgical resection.
On CT,
the mass was seen as a soft tissue mass,
measuring about 1.2cm,
in the peritoneal cavity of epigastric portion (Fig 5).
Xanthogranulomatous pyelonephritis
Xanthogranulomatous pyelonephritis is an unusual form of chronic pyelonephritis in which the renal parenchyma is destroyed and replaced by lipid-laden foamy macrophages.
It usually affects middle-aged women with a history of recurrent urinary tract infection,
diabetes or kidney stones.
The inflammatory process is usually diffuse and can extend beyond the kidney.
The rare focal forms may simulate primary renal tumors.
Sonography shows either diffuse enlargement of the kidney with renal parenchymal thinning or loss of the normal corticomedullary differentiation.
Echogenic material may be seen within the calyces,
corresponding to the fibrinous exudate or hemorrhage seen on gross specimens.
CT shows low attenuation calyces replacing the renal parenchyma and cortical thinning,
representing “bear paw sign” (Figs 6,7) The region of low attenuation represents dilated calyces or inflammatory process.
A large staghorn calculus with contraction of the renal pelvis can be seen.
Complications associated with xanthogranulomatous pyelonephritis include perforation with abscess formation involving the spleen,
paraspinal muscles or psoas muscles,
fistula formation or secondary amyloidosis
Xanthogranulomatous inflammation of urachus
Urachus is an embryological to the allantois.
The urachus narrows to become a fibromuscular strand extending from the apex of the bladder and umbilicus.
Involution of the urachus is usualy complete at birth.
Incomplete involution results in urachal abnormalities: petent urachus,
umbilical-urachal sinus,
vesicourachal diverticulum and urachal cyst.
Infection is the most common complication of urachus.
Xanthogranulomatous lesions are the unusual forms of chronic inflammatory process.
Few cases of urachal xanthogranulomatous inflammation have previously been reported.
Sonography and CT show cystic mass with thick wall extending from umbilicus to the lower pelvis adherent to the dome of the bladder (Fig 8).
In some cases,
preoperative differentiation from urachal carcinoma was impossible.
Xanthogranulomatous prostatitis
Xanthogranulomatous prostatitis is a rare type of granulomatous prostatitis of which very few cases have been reported.
Average age of presentation is the sixties and it may present with lower urinary tract infections.
On rectal examination,
prostate may be hard and nodular mimicking prostate carcinoma.
Rectal sonography usually shows hypoechoic lesions.
On sonography and MRI,
the differentiation between xanthogranulomatous prostatitis and prostate cancer may be difficult (Fig 9).
Xanthogranulomatous inflammation of the female genital tract
Xanthogranulomatous inflammation of the female genital tract is rare and affects endometrium,
fallopian tubes or ovaries focally or entirely,
which clinically forms mass in the pelvic cavity and invades surrounding tissues.
It usually present with history of pelvic inflammatory disease lasting months and years.
It usually occurs between 23 and 72 years (mean; 38.5 years).
The clinical presentations include anemia,
anorexia,
fever,
irregular colporrhagia,
abdominal pain,
and adnexal mass with tenderness.
Sonography and CT show a well-defined solid mass or cystic mass with thick internal septum.
It may be difficult to differentiate to the ovarian malignancy (Fig 10).