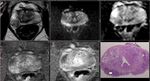
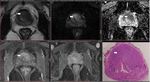
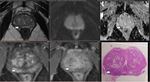
Multiparametric (mp) MRI of the prostate entails functional imaging sequences in addition to the standard anatomical T1WI and T2WI imaging.
The functional sequences of choice are dynamic contrast-enhanced (DCE) MRI and diffusion-weighted imaging (DWI) and calculation of apparent diffusion co-efficient (ADC) maps.
MR spectroscopy is no longer considered essential for multi-parametric MRI and is not recommended in PIRADS v2(5).
Typical imaging consists of T2WI imaging small field of view in three planes,
unenhanced T1-weighted axial imaging,
axial DCE- over ideally 3 - 4 minutes,
and axial DWI (b0,
b500 and b1000) together with ADC maps(6).
Although imaging can be achieved on 1.5 T,
3T is preferred due to higher signal-to-noise ratio.
Good-quality imaging can be achieved with both surface and endorectal coils.
Pooled data showed a specificity of 88% and sensitivity of 74% for prostate cancer detection,
and negative predictive values ranging from 65 to 94%(7).
Multi-parametric MRI is most useful in detection of clinically significant prostate cancer.
Although there is no universally agreed definition of clinically significant prostate cancer,
Gleason 7 or higher,
tumor volume of at least 0.5 mL (1 cm length on imaging),
and/or extraprostatic extension are thought to correspond to clinically significant tumor.
According to the PIRADS lexicon,
clinically significant tumor in the peripheral zone on T2 imaging include circumscribed homogenous hypointense lesions confined to the prostate and measuring less than 1.5 cm in maximal dimensions (PIRADS 4).
PIRADS 5 includes lesions larger than 1.5 cm and evidence of extraprostatic extension(5).
On diffusion-weighted imaging,
markedly hypointense lesions on ADC with corresponding hyperintensity on high b-value imaging represents clinically significant lesions,
with lesions smaller than 1.5 cm being ascribed to PI-RADS 4 and those larger than 1.5 cm being PI-RADS 5 (5).
Dynamic contrast enhanced images should always be interpreted in conjunction with the anatomical T2WI imaging and the diffusion-weighted imaging.
Focal enhancement in clinically significant cancer usually corresponds to focal findings on T2W and/or DWI.
DCE may be helpful when evaluation of DWI is technically compromised and in identifying the index lesions in patient multiple lesions(5).
A 5 point Likert scale has also been proposed in ascribing the degree of suspicion for lesions and has been found to favobably correspond to tumors volume and Gleason score(8)
Multi-parametric MRI is also useful for staging especially for differentiating between organ confined tumors and extraprostatic extension or seminal vesicle invasion.
This distinction is important as separates patient would benefit from radical prostatectomy.
It is also useful from a prognostic point of view. Imaging features of seminal vesicle invasion include focal or diffuse low T2W signalintensity and/or abnormal contrast enhancement within and/or along the seminal vesicle,restricted diffusion,
obliteration of the seminal prostatic angle and evidence of direct tumor extension from the base of the prostate into and around the seminal vesicle(5).
Whole mounts prostate histopathology specimen of patients who underwent radical prostatectomy were obtained and the sites of prostate tumor within the gland marked by the pathologist.
These were directly compared to the preceding multi-parametric MRI (T1WI,
T2WI,
DWI/ADC with or without dynamic postcontrast imaging).
For each patient a compilation of the dominant lesion on the T2WI imaging and ADC DWI sequences were analyzed and compared for concordance with the histological specimen.
MRI staging was also compared to the final histopathology stage.
In a previous study by Vargas et al,
PI-RADS 2 correctly identified 94–95 % of PCa foci ≥0.5 mL,
but was limited for the assessment of GS ≥4+3 tumours ≤0.5 mL.
DCE-MRI offered limited added value to T2WI+DW-MRI(6).