INTRODUCTION
The appendiceal mucocele (AM) is an uncommon disorder,
which is found in 0.2-0.3% of all appendectomies and represents 8%-10% of all appendiceal tumors.
Usually it occurs in patients of middle age (> 50 years) and according to some studies the incidence is similar between men and women,
while for other authors there is a higher incidence in females (4: 1).
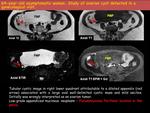
We present our series of appendiceal mucocele that consists of a total of 8 cases (5 women,
3 men),
aged between 30 and 87 years (mean 64.8 years),
diagnosed between January 2012 and March 2017.
Except for one case in which the patient was not a tributary of surgical treatment,
the rest have histological verification (table 1):
-
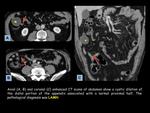
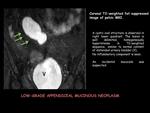
5 Mucoceles: 4 low-grade appendiceal mucinous neoplasms (LAMNs) and 1 mucosal hyperplasia.
-
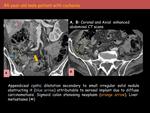
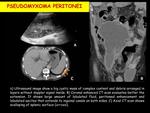
2 Pseudomyxoma Peritonei: 1 located in the right lower abdomen and the other diffuse.
-
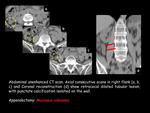
1 appendiceal obstruction due to implantation secondary to carcinomatosis due to synchronous sigmoid colon neoplasia (fig.2).
We review the current histological classification,
the clinical manifestations and the imaging features giving particular attention to the findings that may contribute to an accurate diagnosis.
ETIOLOGY AND HISTOLOGICAL CLASSIFICATION
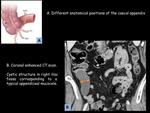
The appendiceal mucocele is not a pathological entity in itself,
but is a morphological term to describe macroscopically a cecal appendix with a very distended lumen due to an anomalous accumulation of mucus inside,
associated or not with obstruction,
affecting partially or completely the organ (fig.3).
This process is due to various pathological disorders,
both neoplastic and non-neoplastic.
Although the most frequent etiology is the Appendiceal Mucinous Neoplasm the terms mucocele and mucinous neoplasm are not interchangeable.
Histologically we can divide the appendiceal mucoceles into 4 subtypes:
-
Simple mucocele
-
Mucosal hyperplasia
-
Mucinous adenoma
-
Mucinous adenocarcinoma
The simple mucocele or appendiceal retention cyst is caused by an obstruction of the appendix base that can be caused by many etiologies: fecaliths,
scars due to chronic inflammation,
parasites,
polyps,
etc.
It has also been described in cases of endometriotic implants and melanoma metastasis.
Benign appendiceal mucoceles are much more frequent than the malignant ones,
accounting for 63% to 84% of cases.
The classification and nomenclature of appendiceal mucinous tumors is controversial and,
sometimes,
still unclear.
The 2010 WHO classification is the currently most accepted classification and recognizes 3 main categories of mucinous neoplasms (table 2):
Adenomas are confined to the mucosa of the appendix with no invasion beyond the muscularis mucosa.
Adenomas of appendix follow an adenoma-carcinoma sequence and require excision as premalignant lesions.
LAMNs are low-grade tumors that are morphologically well-differentiated adenomas that can proliferate outside de the appendix.
Mucinous adenocarcinoma presents invasive glands with high-grade of cytological atypia,
destruction of the appendiceal wall,
extracellular mucin in more than 50% of the lesion and risk of metastasis.
The Pseudomyxoma Peritonei (PMP) represents the presence of generalized implants of mucin in the abdominal cavity,
secondary to the extension of a mucinous neoplasm,
frequently by spontaneous or intraoperative rupture of a LAMN.
The PMP is also classified into three categories: low-grade,
high-grade and PMP with seal ring cells.
The terms of low-grade and high-grade PMPs are synonyms of the previous diffuse peritoneal adenomucinosis (DPAM) and peritoneal mucinous carcinomatosis (PMC),
respectively.
Traditionally,
PMPs were considered to originate from primary ovarian tumors,
but immunohistochemistry has shown that they originate from gastrointestinal mucinous neoplasms,
basically of appendiceal origin.
The most important factors that must be taken into account for any appendiceal mucinous lesion and that may influence the prognosis of the disease are the presence of extra-appendiceal mucin and the degree of cytological atypia.
The current trend is to avoid the terms "cystadenoma",
“mucinous cystadenocarcinomas”,
“DPAM” and “PMP”.
CLINICAL MANIFESTATIONS
The clinical manifestation is rather unspecific.
Most of these AM are asymptomatic and are detected incidentally in surgery or when performing an imaging test for another unrelated reason (50%).
When they are symptomatic,
the most frequent clinical presentation simulates an acute appendicitis.
Few times the patient comes with a palpable painless abdominal mass or with intestinal obstruction due to torsion or invagination of the mucocele,
anemia due to intestinal bleeding,
weight loss or vomiting.
PMP can present with increased abdominal girth or abdominal hernias.
DIAGNOSTIC IMAGING
The preoperative diagnosis is advisable in order to properly plan the surgical procedure and avoid the most feared complication,
which is the accidental rupture of the mucocele and the subsequent development of a PMP.
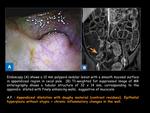
In both the endoscopy and the barium enema,
the appendiceal mucocele can be detected as an elevation or a soft print located on the medial side of the cecal pole that suggests the presence of an extra-mucosal or extrinsic process (fig.4),
and given the typical topography,
the appendiceal origin is the first suspicion.
Endoscopy can be diagnostic if it shows the discharge of mucin in the appendiceal orifice.
However,
neither the endoscopy nor the enema allow to adequately evaluate the size or relationships of the lesion.
This requires sectional imaging such as ultrasound (US),
Computed Tomography (CT) or Magnetic Resonance (MRI).
Given that these patients are usually presenting with acute pain in right lower abdominal quadrant,
US and CT are the techniques usually used in the diagnosis of emergencies.
Patients with mucinous neoplasms may have increased carcinoembryonic antigen levels.
Fine-needle biopsy should be avoided as it can cause peritoneal spread and the cytological diagnosis is usually difficult.
Conventional radiology
Plain radiographs of the abdomen help a little for the diagnosis of AM,
although sometimes it is possible to see curvilinear calcifications in the right iliac fossa.
The barium enema or double contrast enema are increasingly disused techniques.
Classic signs include appendix fill defect,
well-circumscribed submucosal lesion in the cecal pole and extraluminal compression.
Ultrasound Findings:
Mucocele usually presents on US as a cystic lesion of ovoid,
tubular or pear-shaped morphology,
with content of diverse echostructure,
usually with low level internal echoes,
sometimes with fine echogenic septa organized in concentric layers which represents mucin laminated (fig.5).
This "onion-skin” appearance is considered a pathognomonic sign of AM.
Parietal hyperechoic foci with posterior shadow can be observed,
which translates the presence of mural calcifications.
In case of female patients it’s very important to try to locate the right ovary and avoid confusing the appendiceal mucocele with ovarian cystic disorders.
If the appendix shows a transverse diameter greater than 15 mm,
an AM will be suspected with a sensitivity of 83% and a specificity of 92%.
Although the size of the lesion is not necessarily associated with malignancy,
AMs smaller than 2 cm are rarely malignant.
CT Findings
The current technology with multidetector CT scan offers the possibility to study the anatomy of the appendiceal region with multiplanar high-definition images,
facilitating the assessment of the pathology and its spread.
For these reasons CT is the technique of choice that allows to visualize in greater detail the anatomical relationships of the cecal region and its parietal calcifications.
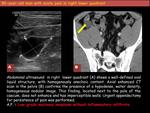
Simple mucocele is seen as a tubular or rounded cystic structure in the expected position of the appendix,
with well-defined contours and enhancing walls of variable thickness.
In 50% of cases there are curvilinear or punctate mural calcifications (fig.6,
fig.7).
Fat stranding in pericecal area may be secondary to inflammatory changes of a concomitant appendicitis.
The presence of gas bubbles or hydro-aerial levels inside the lumen usually indicate infection and can complicate both benign and malignant forms (fig.
8).
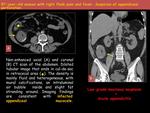
A mural thickening of soft tissue density,
a wall irregularity or a nodular uptake may suggest malignancy.
The presence of mucin outside the appendix excludes the diagnosis of simple mucocele or adenoma and according to the current WHO classification,
it must be considered a feature of LAMN and mucinous adenocarcinoma.
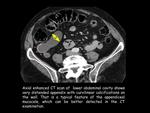
MDCT is especially useful for detecting extra-appendiceal mucin in the right lower quadrant which is also referred to as a localized PMP (fig.9).
Nonetheless,
it is difficult to use CT findings to differentiate benign from malignant mucoceles.
It seems that the wall irregularity and mural soft-tissue thickening can be useful in preoperative diagnosis of malignant AM.
MRI Findings
MRI is helpful to detected incidental AM,
extra-appendiceal mucin and to differentiate large mucinous neoplasms from other intraperitoneal and retroperitoneal disorders.
AM presents as a hyperintense cystic dilatation of the appendix on T2-weighted images (fig.10),
with low or intermediate signal intensity in T1-weighted-images depending on the mucin concentration.
If intravenous contrast is administered,
wall enhancement will be observed also in the case of a simple mucocele.
Pseudomyxoma Peritonei (PMP)
The PMP presents as lobulated ascites serosal implants,
with irregular peritoneal and omental thickening.
The CT allows an appropriate study,
observing a low attenuation ascitic fluid that causes scalloping of liver and splenic margins (fig.11) and fixed bowel loops.
It’s also possible to observe nodules with rim-like calcifications.
DIFFERENTIAL DIAGNOSIS AND COMPLICATIONS
When a cystic well-encapsulated mass is detected in the lower right quadrant of the abdomen,
the differential diagnosis should include: loops of the small bowel distended with fluid content,
cystic lymphangioma,
abscesses,
mesenteric cyst,
enteric duplication cyst and Meckel's diverticulum.
In females,
cystic disorders of adnexal origin must also be ruled out,
such as a cystic ovarian neoplasm,
a tubo-ovarian abscess or a hydrosalpinx.
Inflamed or perforated mucoceles may be indistinguishable from acute appendicitis.
An appendiceal diameter of more than 15 cm is a useful sign of chronic obstruction of the appendix that suggests underlying mucinous neoplasm.
Complications of the AM may include a secondary ileocolic intussusception,
a ureteral obstruction for compression or a torsion with necrosis and hemorrhage.
However,
the main complication and the most feared is the spontaneous or iatrogenic rupture of the AM,
with spread to the peritoneal cavity and development of a PMP.
THERAPEUTIC MANAGEMENT
The treatment is controversial.
It is considered that the regulated appendectomy is sufficient for simple retention cyst and small mucinous adenomas,
whereas bulky adenomas with large base may need cecal resection and always all the implanted mucoid material must be removed.
All appendectomies should include a wide mesoappendix resection to assess for lymph node involvement.
When a mucinous adenocarcinoma is suspected,
treatment should be more aggressive with right hemicolectomy and lymphadenectomy.
It is important to note that all AM over 2cm in diameter should be surgically treated because of the risk of mucinous neoplasm.
The laparoscopic approach is usually not recommended.
If an AM is detected incidentally during a laparoscopy,
it is best to convert it to open laparotomy.
Nevertheless there are more and more case reports and case series describing the use of standard laparoscopy for AM.
The association of AM with other synchronous or metachronous colorectal tumors is well documented.
For this reason,
when the final pathological diagnosis is appendiceal mucinous neoplasm,
an exhaustive review of the rest of the colon before or during surgery is recommended,
and subsequently,
a proper post-surgical follow-up with colonoscopies and / or CT follow-up.