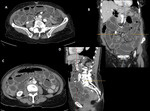
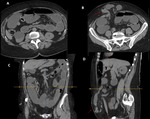
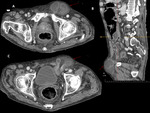
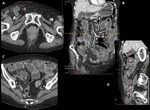
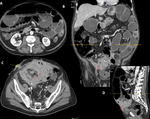
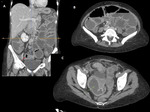
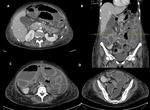
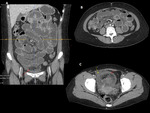
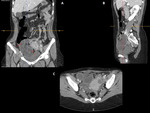
CLINICAL PRESENTATION
The classic clinical features of bowel obstruction are: colicky abdominal pain,
vomiting,
abdominal distension and absolute constipation.
The order and timescale in which these appear vary depending on whether there is large or small bowel obstruction.
Absolute constipation and pain are more prominent early on in large bowel obstruction while vomiting is the predominant early feature of small bowel obstruction.
Additional features depend on the exact underlying pathology.
FIVE QUESTIONS TO ADDRESS IN SUSPECTED OBSTRUCTION
The radiologist must answer five key questions in the evaluation of a patient with suspected obstruction:
1.
Is there obstruction?
2.
Where is the location of the obstruction?
3.
What is the cause of the obstruction?
4.
How severe is the obstruction?
5.
Are there any complications associated?
1.
IS THERE OBSTRUCTION?
The first radiological examination should always be a simple abdominal x-ray. This confirms the diagnosis in 50-80% of the cases.
- Findings of mechanical Small Bowel obstruction (SBO) are:
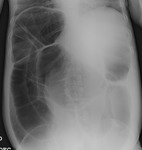
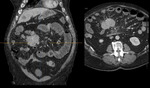
- A dilatation of the proximal small bowel (transverse diameter > 3 cm) with nondilated distal bowel loops. Fig. 3
- Predominantly central dilated loops
- Absence of colonic dilatation (normal caliber or collapsed colon).
- Absence of rectal gas.
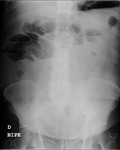
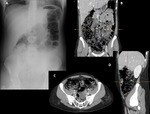
- Multiple gas-fluid levels (>2) on upright or decubitus abdominal radiographs. Fig. 4
- Dilatation of the stomach might be present.
- Findings of mechanical Large Bowel obstruction (LBO) are:
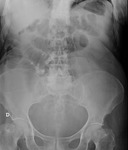
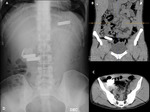
- Colonic distension: gaseous secondary to gas-producing organisms in feces. Fig. 5
- Collapsed distal colon.
- Small bowel dilatation,
depends on the duration of obstruction and the incompetence of the ileocaecal valve.
- In advanced cases,
one may see the stigmata of an ischaemic colon: intramural gas (pneumatosis coli), portal venous gas,
free intra-abdominal gas (pneumoperitoneum).
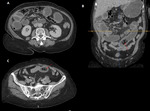
The CT presents itself as the gold-standard examination for the evaluation of obstruction,
it isn’t only able to confirm the diagnosis and localize the location of obstruction but in most instances also is able to identify the cause.
- The radiologic findings suggestive of mechanical SBO in CT are:
- A small-bowel caliber of greater than 2.5 cm,
calculated from outer wall to outer wall,
is considered dilated.
- The transition point often resembles a beak and is described as the beak sign.
- The "small-bowel feces" sign as a result of stasis and mixing of small-bowel contents.
- The radiologic findings suggestive of mechanical LBO in CT are:
- A caliber of greater than 6 cm (9 cm in the cecum) should be considered dilated.
In colonic obstruction,
the cecum is most distensible.
- If the ileocecal valve is incompetent,
dilated small-bowel loops may accompany a large bowel obstruction.
- The large bowel will be distended with a thinned stretched wall but should enhance (unless ischaemic).
The use of positive oral contrast is currently not recommended in guidelines due to its disadvantages: nausea,
vomiting,
risk of aspiration, it demands a minimum delay of 2-3h before the acquisition of CT images and it limits the evaluation of the bowel wall.
2.
WHERE IS THE LOCATION OF THE OBSTRUCTION?
The objective is to identify the transition point.
A systematic approach begins at the rectum and proceeds proximally toward the cecum to determine if the large or small bowel is involved.
The transition point is determined by identifying a caliber change between dilated proximal and collapsed distal small-bowel loops.
Identification of the transition point is generally more difficult in jejunal obstruction.
Multiplanar reformations may aid in determining the site and level of obstruction.
3.
WHAT IS THE CAUSE OF THE OBSTRUCTION?
To determine the cause,
it's important to distinguish whether the obstruction involves the small or large bowel because the causes,
symptoms,
and treatment are often quite different.
- SMALL BOWEL OBSTRUCTION (SBO)
Small bowel obstruction accounts for 80% of all mechanical intestinal obstruction.
Causes can be divided into congenital and acquired.
In the adult,
most of the causes are acquired,
and can be extrinsic causing compression,
intrinsic,
or luminal.
1.
EXTRINSIC CAUSES.
1.1.
FIBROUS ADHESIONS
Adhesions are the main cause of small bowel obstruction,
ranging from 50%–80% of all cases.
Almost all of them are postoperative,
with a minority being secondary to peritonitis.
The diagnosis of SBO due to adhesions is primarily one of exclusion because adhesive bands are not seen at conventional CT; only an abrupt change in the caliber of the bowel is seen with no identifiable cause (no masses,
no inflammation,
no wall thickening).
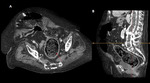
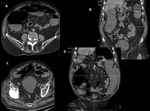
This finding combined with a history of abdominal surgery and associated kinking and tethering of the adjacent nonobstructed bowel usually suggests the diagnosis. Fig. 6, Fig. 7
1.2.
ABDOMINAL HERNIA
Hernias are considered the second most common cause of SBO,
responsible for 10% of cases.
In developing countries,
they are still considered the foremost cause.
Hernias are classified according to the anatomic location of the orifice through which the bowel protrudes.
They are broadly classified as external or internal.
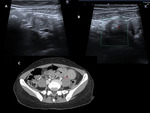
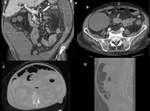
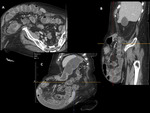
- An external hernia results from a defect in the abdominal and pelvic wall at sites of congenital weakness or previous surgery. Fig. 8, Fig. 9, Fig. 10
- An internal hernia is less common,
it occurs when there is protrusion of the viscera through the peritoneum or mesentery and into a compartment within the abdominal cavity.
1.3. ENDOMETRIOSIS
Endometriosis is the presence of functional endometrial glands and stroma outside the uterine cavity and musculature.
It affects about 5% of women of reproductive age.
Endometrial implants are typically located on the antimesenteric edge of the bowel,
and their appearance is variable,
being the most common like a solid nodule with positive enhancement contiguous with or penetrating the thickened bowel wall.
1.4. MASSES
- Extrinsic neoplasm. Fig. 11
- Intra-abdominal abscess.
- Aneurysm.
- Haematoma.
2.
INTRINSIC BOWEL WALL CAUSES
2.1.
INFLAMATTION,
e.g. Crohn,
tuberculosis, eosinophilic gastroenteritis…
- Crohn Disease:
Small bowel obstruction in Crohn disease can be a manifestation of three clinical situations that can occur in this disease.
1.
The acute presentation is characterized by bowel luminal narrowing secondary to the transmural acute inflammatory process.
The radiologist may see bowel wall thickening with stratification,
mucosal hyperenhancement,
and the comb sign. Fig. 12, Fig. 13
2.
In the chronic phase,
the luminal stenosis is predominantly of a cicatricial/fibrotic etiology and there is fat deposition in the bowel wall.
3.
Finally,
it can be secondary to adhesions,
incisional hernias,
exacerbation of the inflammatory condition,
or postoperative strictures in patients who have undergone previous intestinal surgery.
2.2. TUMOUR
Primary small bowel neoplasms are rare (<2% of gastrointestinal malignancy) and usually advanced at the time of SBO.
The most common include adenocarcinoma,
lymphoma,
gastrointestinal stromal tumors (GIST) and carcinoid tumors.
The findings in the CT depend on the type of tumor.
In the case of adenocarcinoma,
it shows an irregular and asymmetric mural thickening with luminal narrowing at the transition point. Fig. 14, Fig. 15
Metastatic disease is the most frequent neoplastic cause of SBO.
It is more frequent in the form of peritoneal carcinomatosis,
which is suggested when extrinsic serosal disease involving the small bowel wall is seen in association with a transition point. Fig. 16
Tumors with a propensity to cause widespread peritoneal metastases include ovarian,
colonic,
pancreatic,
and gastric neoplasms.
2.3.
RADIATION ENTERITIS
Radiation enteritis causes obstruction in the late phase one year after radiation therapy,
usually to the pelvis by fibrotic changes and mesenteric adhesions.
Therefore,
the ileal loops are the most affected.
CT shows narrowing of the lumen secondary to mural thickening,
an angular bowel wall due to adhesions,
and retraction of the mesentery.
There may also be an abnormal enhancement of the thickened bowel wall caught in the line of the radiation Field.
2.4.
INTESTINAL ISCHAEMIA
Occlusion or stenosis of the mesenteric arterial or venous vascular supply to the bowel usually produces bowel ischemia,
which subsequently causes wall thickening in the affected loops with noncircumferential or asymmetric wall enhancement,
resulting in obstruction.
In advanced cases,
a bowel infarct may be present,
which manifests at CT as pneumatosis and air in the portal venous system. Fig. 17, Fig. 18, Fig. 19
2.5.
INTRAMURAL HAEMATOMA
Intramural small bowel hematoma may occur secondary to anticoagulant therapy,
iatrogenic intervention or trauma.
The development of obstruction is usually due to luminal narrowing.
If this condition is suspected,
nonenhanced CT should be performed,
as it will show a spontaneously hyperattenuating clot.
CT also demonstrates circumferential,
homogeneous,
regular,
and spontaneously hyperattenuating wall thickening with moderate mesenteric infiltration.
2.6.
INTUSSUSCEPTION
Intussusception is a relatively rare condition in adults,
accounting for less than 5% of SBOs.
Only lead-point intussusceptions secondary to neoplasms,
adhesions,
or foreign bodies are associated with SBO.
Transient intussusceptions are not associated with this condition.
At CT,
the presence of a bowel-within-bowel configuration with or without mesenteric fat and mesenteric vessels is pathognomonic for intussusception.
We can find three patterns depending on the severity and duration of the disease: the target sign,
a sausage-shaped mass with alternating layers of low and high attenuation,
and a reniform mass. Fig. 20
3.
INTRALUMINAL CAUSES
3.1.
FOREIGN BODY,
BEZOAR
Bezoars:
Obstruction secondary to a bezoar is rare,
but the number of cases has increased owing to the high frequency of gastric outlet surgery.
Such surgery prevents adequate digestion of vegetable fibers,
which become impacted,
causing obstruction.
At CT,
a bezoar appears as an intraluminal mass with an ovoid shape and a mottled gas pattern.
Foreign body:
It usually occurs in children or in emotionally disturbed or mentally disabled patients.
At CT,
the findings consist of SBO with evidence of a foreign body at the transition point. Fig. 21
3.2.
GALLSTONE ILEUS
Gallstone ileus is a rare complication of recurrent cholecystitis,
caused by migration of a large gallstone through a biliaryintestinal fistula with subsequent impaction in the small bowel.
CT findings are pathognomonic,
corresponding to the radiographic triad of pneumobilia,
ectopic gallstone,
and small bowel obstruction.
3.3. MECONIUM ILEUS (or meconium ileus equivalent,
distal intestinal obstruction syndrome).
Distal intestinal obstruction syndrome is a cause of obstruction that usually occurs in older children and adults with cystic fibrosis.
The obstruction is secondary to impaction of thick stool,
which is probably related to inadequately controlled intestinal absorption secondary to pancreatic insufficiency.
This condition responds to medical treatment.
At CT,
the findings consist of SBO with feculent filling defects in the small bowel.
- LARGE BOWEL OBSTRUCTION (LBO)
Large bowel obstructions are far less common than small bowel obstructions,
accounting for only 20% of all bowel obstructions
The causes of LBO may be classified into three categories:
1. LUMINAL OBSTRUCTIONS: intussusceptions,
fecal impaction,
fecaliths,
gallstones and foreign bodies.
1.1.
FAECAL IMPACTION / FAECALOMA (most common cause in debilitated elderly).
Fecal impaction occurs when a hard piece of stool becomes lodged in the colon.
It is most often seen in people with long-term constipation,
as the stools become dry,
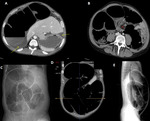
hard and difficult to pass. Fig. 22, Fig. 23
2. INTRINSIC CAUSES (colonic wall lesions): colorectal tumors,
diverticulitis,
inflammatory bowel disease,
and ischemic colitis.
2.1.
COLON CARCINOMA
Colon carcinoma is the most common cause of LBO (60% of cases),
and mortality is high (10%–30%) in patients requiring emergency surgery.
The two most frequent locations of obstruction due to colonic malignancy are the sigmoid colon and the splenic flexure. Fig. 24
Right-sided tumors with an incompetent ileocecal valve can mimic SBO.
Left-sided malignancies cause diffuse distension of the colon up to the level of obstruction.
CT findings include asymmetric and short-segment colonic wall thickening or an enhancing soft-tissue mass centered in the colon that narrows the colonic lumen with or without findings of ischemia and perforation.
Colonic malignancy may mimic diverticulitis if there is pericolonic spread with infiltration of the pericolonic fat.
The identification of pericolonic lymph nodes larger than 1 cm in short axis should raise the suspicion of malignancy.
2.2.
COLONIC DIVERTICULITIS
Although less common (10% of all cases of LBO),
patients with acute diverticulitis can present with LBO due to bowel wall edema and pericolonic inflammation.
High-grade obstruction is less common in the setting of diverticulitis; more commonly,
obstruction occurs in the setting of multiple episodes of diverticulitis,
which causes narrowing and stricture formation.
Chronic diverticulitis can produce both LBO and a chronically dilated colon.
2.3. ISCHEMIC COLITIS
Ischemic colitis refers to inflammation of the colon secondary to vascular insufficiency and ischemia. Fig. 25
Complications of ischemic colitis can include bowel perforation,
peritonitis,
persistent bleeding,
protein-losing colopathy,
and symptomatic intestinal strictures causing obstruction.
3. EXTRINSIC CAUSES: volvulus,
hernia,
adhesion,
peritoneal dissemination,
and compression by diseases in adjacent organs.
3.1 VOLVULUS
Acute colonic volvulus accounts for approximately 10%–15% of LBO.
Volvulus is defined as a twisting of the intestine upon itself that causes obstruction.
If the twist is greater than 360°,
the volvulus is unlikely to resolve without intervention.
Vascular compromise at the site of volvulus leads to ischemia,
necrosis,
and perforation.
Sigmoid volvulus is more common than cecal volvulus. Fig. 26
A major predisposing factor leading to a colonic volvulus is a mobile redundant colon on a mesentery and a fixed point about which the colon can twist.
3.2.
HERNIA
It’s less common than small bowel hernias.
CT: the colon will be found in a hernia with dilated proximal colon and decompressed distal colon. Fig. 27
4.
HOW SEVERE IS THE OBSTRUCTION?
The objective is to grade the severity of obstruction: complete or high-grade obstruction versus partial or low-grade obstruction.
It’s determined by the degree of distal collapse,
proximal bowel dilatation and transit of ingested contrast material (used on rare occasions).
In a high-grade obstruction,
there is a 50% difference in caliber between the proximal dilated bowel and the distal collapsed bowel and can be the presence of the "small bowel feces" sign.
Passage of contrast material through the transition zone into the collapsed distal bowel indicates a partial bowel obstruction.
5.
ARE THERE ANY COMPLICATIONS ASSOCIATED?
It’s very important to differentiate a simple obstruction from a complicated one,
such as a closed loop or strangulated bowel obstruction.
A closed-loop obstruction is a form of mechanical obstruction in which a loop of small bowel is occluded in two points along its course,
virtually isolating the segment between those two points from the remainder of the GI tract. Fig. 28
In a closed loop or incarcerated small-bowel obstruction,
a U-shaped or radial configuration of fluid-filled dilated bowel loops is typically seen,
with mesenteric vessels converging toward the point of obstruction.
At the site of obstruction,
there may be a whirl sign,
a beak sign,
or triangular configuration of adjacent collapsed loops.
Strangulation obstruction indicates that blood flow is compromised, which may lead to intestinal ischemia, necrosis,
and perforation. Obstruction to venous outflow is the most common cause of ischemia in bowel obstruction. Fig. 29
This condition often results from an increase in intraluminal pressure as a function of bowel distention,
the bowel becomes edematous and leaks fluid into the lumen,
resulting in progressive dilatation,
and into the peritoneal cavity,
causing ascites. There is more risk of intestinal perforation due to the great distension. Fig. 30
The CT findings associated with ischemic bowel include bowel with thickening, mesenteric edema and/or fluid in the adjacent mesentery or peritoneal space,
abnormal decreased bowel wall enhancement,
and pneumatosis with or without associated gas in mesenteric or portal veins.
Intestinal ischemia and infarction are the major causes of morbidity and mortality in patients with bowel obstruction.