We will review the typical radiologic findings of some sites that can be affected by avascular necrosis presenting selected cases from our Imaging Department: femoral head in adults and children,
humeral head,
scaphoid and metatarsal bone.
All the cases were first studied by radiography and some followed by MR and CT.
The clinical history and possible associated cause were correlated with the imaging findings.
The pathology progression was documented by radiography imaging.
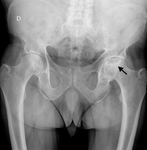
The first radiographic sign in avascular necrosis of the hip occurs weeks or months after the bone infarct.
Sclerosis is the initial radiologic finding,
first because of the hipervascularized bone surrounding the necrotic bone and later due to the new bone formation.
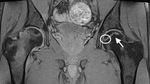
The classic radiographic appearance is patchy areas of lucency and sclerosis,
with the sclerotic bone showing a undulating morphology over the lesion rim (Fig.
1,
arrow).
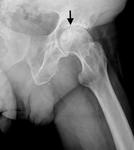
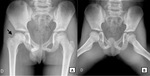
A linear subchondral fracture termed “crescent sign” (Fig.2,
arrow) is the typical finding developed during bone healing that often progresses to subchondral fragmentation,
flattening and deformity.
These complications can evolve to secondary osteoarthritis [3,4].
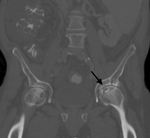
CT scan can demonstrate some later changes of a ischemic bone as serpentine and undulating sclerotic margin (Fig.3,
arrow),
although CT is not the best choice for evaluation and detecting early stages of ON [18].
MR is the most sensitive image modality for diagnosis avascular necrosis.
The initial findings can be nonspecific as diffuse marrow edema.
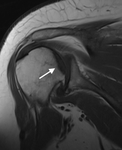
As the condition progresses,
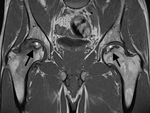
the caracteristic imaging of a serpiginous low-signal-intensity rim with all pulse sequences appears corresponding to a line of sclerosis (Fig.
4,
arrow).
The surrounding yellow marrow maintains the signal intensity as viable and devitalized adipose tissue have an indentical intrinsic MR imaging appearance.
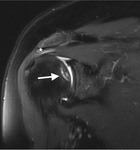
On T2 sequences,
a “double-line” sign can be seen with the outer low-signal-intensity rim representig the sclerosis and the inner rim of high signal intensity representing the reparative granulation tissue of the reactive interface (Fig.5,
arrow) [19,20].
The chosen initial exam for suspected LCP is radiography with frontal and frog-leg lateral projections [21].
The first radiographic sign may be the presence of effusion,
which can mimic infection.
Later on,
due to the loss of blood flow,
the ossific nucleus of the affected femoral head fails to grow resulting in smaller appearance than the contralateral normal side.
The combination of mechanical forces and weakness of the femoral epiphyses by the necrosis and healing process account for fragmentation and flattening of the femoral head (Fig.6).
Growth abnormality results in metaphyseal irregularity with consequent shortness and a wide femoral neck (coxa magna) and a superiorly located (“high-standing”) greater trochanter [3,4] (Fig.6 (A),
arrow).
The main imaging modalities used in the diagnosis of humeral head osteonecrosis are radiography and MR imaging.
The standard radiography is commonly used to stage disease progression,
although,
MR imaging is more sensitive and useful in the diagnosis of the humeral head osteonecrosis.
In earlier stages,
the sclerosis which may be focal or diffuse,
results from subchondral microfracture without articular collaps.
It typically appears in the superior portion of the humeral head and as an hyposignal on T1-weighted images (Fig.
7).
A double-line sign representing lines of alternating high and low signal intensity on T2-weighted images,
as described before in the femoral head,
is observed in over 50% of patients with osteonecrosis of humeral head [22].
The inner hypersignal line corresponds to hyperemic granulation tissue and the outer dark band corresponds to fibrosis or sclerosis (Fig.
8).
In later stages,
fragmentation and articular collapse can occur and be accompained by joint effusion [23].
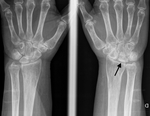
To diagnose Kienbock disease,
as expected,
radiography imaging is usually the inicial imaging.
Sclerosis,
fracture,
flattening and loss of volume of the lunate bone is possible to see on a radiographic exam (Fig.
9).
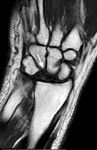
MR is the most sensitive and specific imaging modality to detect early disease and to diagnose the cause of wrist pain in patients with persistent clinic suggesting Kienbock disease but with normal radiographs [24].
The diagnosis is made when diffusely decreased T1-weighted signal intensity involves the entire lunate (Fig.10,
arrow) or suggested when hypointese is seen centrally and within the radial aspect of the lunate.
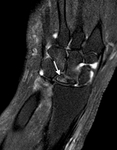
T2-weighted or STIR signal intensity is variable,
and in the acute phase high T2 and intermediate T1 signal can be associated with bone oedema (Fig.11,
arrow).
As the other suspected cases of osteonecrosis,
radiography is often the initial imaging modality to diagnosis Feiberg’s disease.
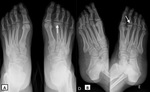
In early stages,
metatarsal head flattening and decreased bone density is seen,
followed by metatarsal head sclerosis,
fragmentation and deformation (Fig.12,
arrow).
Later on,
the presence of metatarsophalangeal osteoarthrosis with intra-articular loose bodies is seen [25].