From January 2015 to September 2017,
94 patients with abdominal pain and clinical-diagnostic suspect of ASBI,
primary or secondary to bowel obstruction,
have been admitted to the Department of General Surgery of our Emergency Hospital,
to undergo surgery in regime of emergency/urgency.
Patients with ASBI secondary to neoplasms,
vasculitis,
inflammatory bowel diseases and traumatic events were excluded from our sample,
due to the large number of comorbidities that could affect a correct evaluation of ASBI CT signs.
Before every surgical procedure,
an abdominal CT has been performed with the 64-slice CT scan present in our Emergency Radiology Department.
First of all,
a scan without contrast was performed in the cranio-caudal direction,
with patient in supine position,
during an inspiratory apnea.
Secondly,
with the bolus-tracking technique (threshold = 100 UH) an angiographic study of abdominal aorta and splancnic arterial circle was performed,
by intravenous administration of iodinated contrast medium (100-130 ml; speed of injection: 3-4 ml/s).
40 ml of saline solution followed contrast injection.
Then,
after 80s from the contrast administration,
a portal venous phase was acquired.
Technical parameters employed were the following: 120 KV,
300 mAs; slice thickness ranged from 0.75 to 2.5 mm.
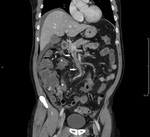
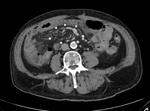
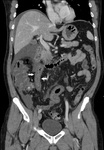
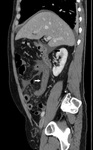
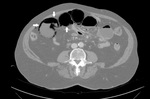
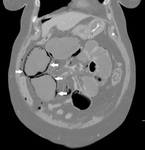
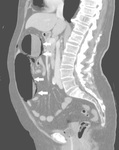
Presence of the following CT indicators of ASBI has been blindly assessed by two experienced Radiologists:
- vascular (arterial/venous) obstruction (Fig.1);
- "Whirlpool" sign (Fig.
2);
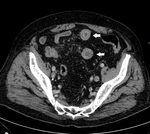
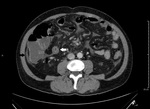
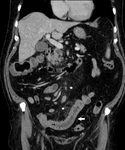
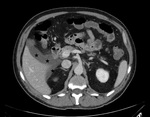
- "Target" sign (Fig.
3-4);
- altered enhancement,
evaluated as:
- increased;
- reduced in submucosa (Fig.
5-6);
- reduced in the whole bowel wall;
- altered thickness,
evaluated as:
- increased (Fig.
7);
- reduced;
- free abdominal fluid (Fig.
1-4-5-6-8);
- intramural bowel gas (Fig.
9-11).
Discrepancies were solved by consensus.
Chi square test was used for statistical analysis.