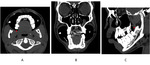
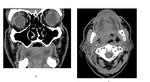
Anatomy of the oral cavity
The oral cavity has two main subdivisions – the vestibule,
which lies anteriorly and laterally,
and the central part - the oral cavity proper (OCP).
[ Fig. 1]
The borders of the vestibule are:
- the lips anteriorly,
- the buccal mucosa laterally,
- the gingivobuccal sulci (GBS) inferiorly and superiorly,
- the gingival mucosa medially.
The borders of the oral cavity proper are:
- the gingival mucosa of the upper and lower alveolus laterally,
- the hard palate superiorly,
- the mucosa of the mouth floor inferiorly,
- the oral tongue is a part of the OCP and is located centrally.
The oral cavity lies anteriorly to the circumvallate papillae of the tongue,
the anterior tonsillar pillars and the soft palate.
Posteriorly,
the two spaces are connected behind the third molars.
The mucosal fold,
extending behind the last mandibular and maxillar molars along the ascending ramus of the mandible is known as the retromolar trigone (RMT).
In neutral position the mucosal surfaces are in close contact with each other,
which makes them difficult to assess radiologically.
[Fig. 2]
Tumors the oral cavity
According to WHO tumors of the oral cavity can be classified in 8 major histological groups [ Table 1].
Of all malignant neoplasms of the oral cavity more than 90% are squamous cell carcinomas (SCC) of the lining mucosae.
Oral cavity cancers are the sixth most common type of cancer worldwide,
and the eighth most common in Europe,
with around 60 000 new cases per year in the European Union [1,
2].
The dominant risk factors are tobacco use and alcohol abuse,
which are strongly synergistic.
HPVs,
especially those genotypes of known high oncogenic potential /HPV 16 and 18/,
are found in a variable but small proportion of oral SCCs,
but they have not yet been conclusively linked to SCC of the oral cavity [3].
Clinical presentation may vary,
depending on the primary tumor origin site and the extent of spread.
The initial assessment of the disease is mostly clinical,
but deep local spread is often underestimated [3,
4,
5].
Imaging
The currently available multi-detector computed tomography (MDCT) techniques provide critical information about locoregional spread (mucosal surfaces deep soft tissue,
muscles and bone),
lymph node dissemination and perineural spread – important factors in preoperative assessment and staging [4,
5].
Anatomical accuracy in locoregional assessment (epicenter,
dimentions,
mucosal extent) can be beneficial for the selection of the most effective treatment strategy.
Unfortunately it can oftentimes be hindered by the mobility of small structures and apposition of mucosal surfaces.
Small tumors in particular can be a challenge for the radiologist and may even go unnoticed in standard CT examination [6,
7].