Pulmonary Infections In Immunocompromised Patients
Bacterial Infections
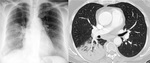
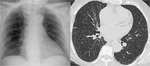
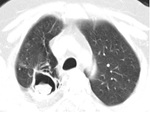
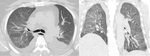
Bacterial Pneumonias have a similar radiographic pattern in immunocompetent and imunnosupressed patients.
Findings are usually inespecific and include consolidation,
which may be focal (segmental ou lobar),
cavitation,
groud-glass opacities,
broncocentric nodules,
pleural effusion and lymphadenopathy ( Fig. 1 ).
Computed Tomography may demonstrate lesions earlier than chest radiographs,
when only ground-glass pattern might be seen.
Patiens in septicaemia may quickly progress to acute respiratory distress patterns.
Tuberculosis
Immunity integrity is the major predicting factor of the imaging pattern in tuberculosis.
In immunocompetent patients,
a reactivation pattern is seen,
whereas the immunosuppressed patiens present with the primary pattern of the disease.
In severe immunosupressed individuals disseminated or miliary patterns are seen.
Chest radiographs can be useful for diagnosis and follow-up,
but generally a CT scan is perfomed,
mostly because it lacks proficiency in identifying opacities in the lung apex and enlargement of hilar/mediastinal lymph nodes in primary tuberculosis.
Besides,
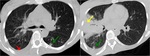
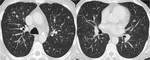
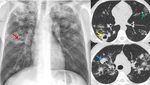
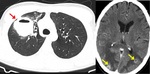
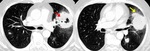
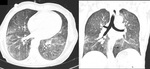
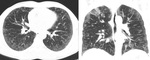
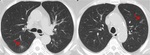
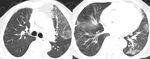
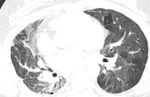
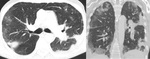
CT can also signs sugestive of activity of the disease,
like cavitation within a consolidation,
centrilobular nodules and tree-in-bud pattern ( Fig. 2 ,
Fig. 3 ,
Fig. 4 ,
Fig. 5 and Fig. 6 ).
Some complications are best assessed with CT,
namely pleural effusions,
empyema and broncopleural fistulae.
In patients that are also diabetic,
multiple cavitation foci,
non-segmental in distribution,
are common.
Atypical patterns can also be present in the context of idiopathic pulmonary fibrosis,
which may be difficult to differentiate from a bacterial pneumonia or neoplasma.
Non-Tuberculous Mycobacteria
Mycobacterium Avium Complex (MAC),
is the most common nontuberculous species identified in patients with AIDS.
The most common presentation is disseminated disease,
which usually coexists with other pulmonar infections.
Chest radiographs and CT show multifocal consolidation and nodules,
which may present cavitation.
Pleural effusion and,
rarely,
a miliary pattern can also be seen.
Mediastinal lymphadenpathy,
often with a low-attenuation necrotic on CT,
is reported to be the most common imagiologic feature.
Nocardiosis
The prevalence of Nocardia infections has recently decreased,
presumably as a consequence of establishment of widespread use of antibiotic prophylaxis.
They usual occur beyond the first month of transplantation.
Dissemination to extrapulmonary sites (brain,
skin and soft tissue) can develop in up to a third of the infected patients ( Fig. 7 ).
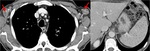
The main imagiologic findings include multifocal lung consolidation,
nodules or masses,
all of which can cavitate.
Sometimes it is possible to detect foci of decreased attenuation within the consolidation,
that are more conspicuous after contrast admnistration with rim enhacement,
reflecting abcess formation.
Infection can spread to the chest wall,
with pleural effusion or chest wall abcess.
Lympahenopathy is not a usual finding in this type of infection.
Fungal Infections
Pulmonary fungal infection,
either hospital acquired or commuinity accquired,
is a severe problem with increasing incidence worldwide.
These infections occur associated with profound neutropenia.
When a patient is receiving broad-spectrum antibiotics and shows radigiophaphic abnormalities,
fungal infectios should always be suspected.
Simultaneous pulmonary and paranasal sinus infection raise the suspicion of Aspergillosis.
Aspergillosis
In immunocomprimesed patients,
aspergillosis pulmonary is classified as airway invasive when Aspergillus invades the basement membrane of the airways,
and angioinvasive when organisms invade the small blood vessels,
leading to hemorrhagic necrosis and pulmonar infarcts.
High-Resolution CT (HRCT) is more sensitive and more specific for early detection in invasive aspergillosis.
The characterist CT appearance of angioinvasive aspergillosis is solitary or multiple lung nodules surround by groud-glass opacity (halo sign),
corresponding with pathologic changes of central consolidation and surrounding hemorrhagic infartaction.
Cavitation occurs in the later stages and is associated with neutrophil recovery,
usually around 2 or 3 weeks after the initial treatment ( Fig. 8 ).
On CT,
airway-invasive aspergillosis manifests as peribronchial consolidation,
centrilobular nodules,
and tree-in-bud opacities reflecting bronchopneumonia and bronchiolitis.
Semi-invasive aspergillosis is found associated with moderate immunity dysfunction,
regularly seen in heavy tobacco smokers,
chronic pulmonary obstructive disease patients and associated with alcoholism.
Chest radiography and CT show a slowly growing nodule or focus of lung consolidation,
sometimes associated with an aspergilloma ( Fig. 9 ).
Underlying structural lung disease such as bronchiectasis or emphysema may be present.
Pleural thickening is also common.
Imaging pattern is similar to reactivation tuberculosis.
A rare manifestation of aspergillosis manly seen in patients with AIDS is obstructing bronchial aspergillosis,
characterized by airways occluded by fungi without inflammation of the bronchial walls.
Radiographs and CT show lower lobe predominant consolidation with dilated mucus-filled airway.
Candidiasis
Pulmonary candidiasis is common in immunosuppressed patients with intravenous catheters,
especially in those receiving broad-spectrum antibiotics and in diabetics.
Candida spp can cause pulmonary infection in two different forms: hematogenous spread or aspiration.
On CT,
the hematogenous type manifests as miliary nodules or larger pulmonary nodules in a random distribution.
Nodules can show either centrilobular distribution,
when associated with pneumonia,
or random distribution,
when associated with haematogenic dissemination.
Random distribution is more common in candidiasis when compared with aspergillosis.
Halo sign,
cavitation and
nodule sizes are similar in both diseases.
Candidiasis from aspiration of oropharyngeal secretions causes bronchopneumonia and manifests on CT as peribronchial consolidation,
usually in a gravitationally dependent distribution.
Pneumocystis Pneumonia
The characteristic CT finding of Pneumocystis Pneumonia is diffuse ground-glass opacity,
which typically has an upper lobe and perihilar predominance,
sometimes with peripheral sparing or a mosaic pattern.
Septal thickening with superimposed ground-glass opacity (crazy paving) and consolidation have also been reported.
Pneumatoceles of varying morphology develop in as many as one-third of patients ( Fig. 10 ).
Pneumatoceles are associated with an increased frequency of spontaneous pneumothorax,
although pneumothorax can develop in the absence of detectable pneumatoceles.
Pleural effusion and lymphadenopathy are uncommon.
There seems to be a different imagiologic pattern regarding the presence of HIV infection.
In patients without HIV infection,
the extent of ground-glass opacity is often greater,
and lung consolidation is more common,
tending to develop more rapidly.
In addition,
the incidence of pneumatoceles has been reported to be greater in patients with HIV infection.
Viral Pneumonia
There is significativ overlap of CT features of viral pneumonia,
and sometimes a distinction from pneumocystis pneumonia can be not possible.
CMV pneumonia generrally presents with of diffuse or focal ground-glass opacity,
patchy or lobar consolidation,
septal thickening,
and small nodules.
Some of the nodules may be surrounded by a halo of ground-glass opacity ( Fig. 11 and Fig. 12 ).
Non-Infectious Pulmonary Complications In Immunocompromised Patients
Non-infectious lung involvement occurs in 25–50% of immunosuppressed patients presenting with lung infiltrates in chest radiographs.
The major causes include pulmonar oedema ( Fig. 13 ),
pulmonar hemorrhage,
drug-induced injury,
idiopathic pulmonar syndrome and bronchiolitis obliterans.
Pulmonary hemorrahage usually presents on HRCT with extensive bilateral consolidation or ground-glass opacities,
sometimes with superimposed intralobular lines (crazy paving pattern).
Drug-induced injury manifestations are non-specific and the presentation can be in form of diffuse alveolar damage,
hypersensitivity reaction,
non-specific interstitial pneumonia and organizing pneumonia ( Fig. 14 ).
Idiopathic pulmonar syndrome is used to describe diffuse pulmonary involvement when no infectious cause is identified.
HRCT demonstrates consolidation with a basilar predominance,
similar to non-cardiogenic pulmonary oedema or infection.
Bronchiolitis obliterans is related to chronic GVHD and is an obstructive pulmonary disorder that affects the small airways.
HRCT findings include areas of decreased attenuation and vascularity (mosaic perfusion),
air trapping and bronchial dilatation ( Fig. 15 ).
There are some neoplasms or neoplasic-like conditions associated with immunosupression,
particularly Kaposi’s sarcoma which presents on HRCT with bronchovascular interstitial thickening and irregular or ill-defined nodules in a predominantly peribronchovascular distribution ( Fig. 16 ).
AIDS-related lymphoma and lymphocitic interstiticial pneumonia should also be kept in mind.