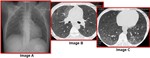
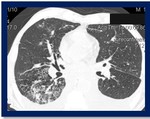
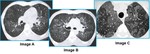
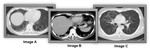
Typical findings:
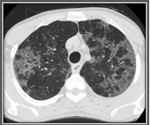
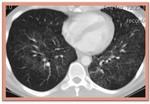
1. Ground glass opacification in the perihilar and mid zones with in some cases (40%) sparing of peripheral subpleural lung - principal finding. In patients receiving prophylactic aerosolized medication,
the upper lobes are frequently involved whereas in patients who are not under such prophylaxis the lower lobes are more prone to infection.
2. Areas-foci of consolidation scattered through the lung parenchyma.
3. Septal thickening-reticular opacities.
Septal thickening which in combination with the ground glass pattern can lead to crazy paving appearance.
4. Pneumatoceles
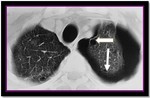
5. Cystic pattern:
- Different shapes,
sizes and various degrees wall thickening
- Multiple and bilateral
- Subpleural or intraparenchymal
- Usually located in upper lobes but may also be present in any location in the lungs
- Must be differentiated from bullae which are typically apical and subpleural in location,
usually thin walled with a regular shape and are an isolated finding and not accompanied with ground glass opacities.
6. Spontaneous pneumothorax is due to rupture of subpleural cysts and in HIV-positive patients it is highly suggestive of PJP.
Moreover,
PJP-related pneumothoraces are resistant in chest tube drainage and pleurodesis or surgical intervention may be necessary.
Atypical findings
1. Lung nodules may be military (2-3mm in diameter) or larger (>1cm),
multiple or rarely solitary.
Masses larger than 7 cm have also been described.
Nodules and masses may rarely cavitate and infrequently present with calcifications.
2. May present as lobar (usually upper lobe) consolidation,
which is more typical for bacterial pneumonias.
3. Interstitial fibrosis – Chronic PCP: septal line thickening,
reticular opacities,
honeycombing and traction bronchiectasis.
4. Bronchiolitis: small,
ill defined centrilobular opacities,
Bronchiolitis obliterans: mosaic pattern,
more prominent on expiratory images and bronchiectasis,
Endobronchial lesion: extremely rare.
5. Lymphadenopathy with or without calcifications.
6. Pleural effusions with or without calcifications: may be due to extension of a subpleural infection into the pleural cavity.
It is considered an infrequent finding and thoracentesis is suggested for a definite diagnosis.
We present 20 patients with PJP on HRCT and low CD4 counts below 200 cells/L,
who were submitted to our Institution and confirmed by identification of fungi in sputum or bronchoalveolar lavage fluid.