Type:
Educational Exhibit
Keywords:
Lung, Respiratory system, Thorax, CT, CT-High Resolution, Diagnostic procedure, Education and training
Authors:
�. Vetešková, K. Zelenak, M. Stevik; Martin/SK
DOI:
10.1594/ecr2018/C-0981
Findings and procedure details
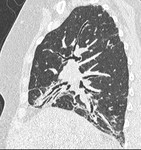
Following the official 2011 ATS/ERS/JRS/ALAT diagnostic criteria for IPF,
the characteristic HRCT UIP pattern includes reticular opacities,
often associated with traction bronchiectasis (Fig.
1) in bibasal and peripheral distribution (Fig.
3) and the appearance of honeycombing (Table 1),
which is critical for making a definite diagnosis.
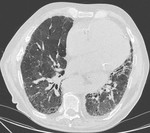
Honeycombing (Fig.
2) appears as variable-sized cystic spaces,
with irregularly thickened walls composed of fibrous tissue.
Several studies have shown,
that honeycombing is consistent with the histopathological diagnosis of UIP.
Furthermore,
honeycombing has also a predictive value,
since it portends a shorter survival compare to individuals with alternative HRCT patterns.
In cases,
where honeycombing is absent but other imaging criteria for UIP are present,
the imaging features are regarded as representing possible UIP and a lung biopsy is indicated.
The official diagnostic criteria have also defined HRCT features,
that are inconsistent with the diagnosis of IPF. This category includes ground glass opacities,
which presence on HRCT scan does not rule out histopathologically proven UIP,
but if they are extensive an another diagnosis should be suggested.
The areas of ground glass opacities on HRCT scans often correlate with histological finding of inflammation within the interstitium or alveolar spaces.
But in patients with UIP it may reflect the presence of interstitial fibrosis.
In such case,
ground glass opacities will be accompanied by other findings suggestive of fibrosis.
Several clinical conditions presence with the pattern of UIP,
and should be considered in differencial diagnosis such as nonspecific interstitial pneumonia,
chronic hypersensitivity pneumonitis,
amiodarone lung,
systematic sclerosis and asbestosis.