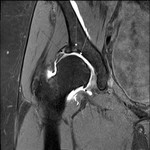
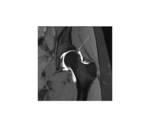
SHOMRI scoring system1 incorporates 8 features including articular cartilage loss,
bone marrow lesions,
subchondral cysts,
labral abnormalities (Figure1),
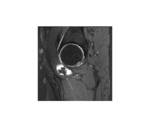
loose bodies (Figure 2),
joint effusion,
paralabral cyst and ligamentum teres abnormalities.
Yet it excludes evaluating some of the well known features of OA for example osteophytes and subchondral sclerosis because they assume these features can be better and more time effectively evaluated on plain radiographs.
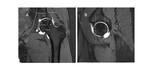
SHOMRI scoring systems1 divides hip joint in 10 different subregions to evaluate articular cartilage morphology,
subchondral bone marrow lesions and subchondral cyst (Figure 3A,
3B),
4 definitive locations for assessing labrum and no definitive location for scoring synovitis.
SHOMRI scoring system is based only on non–contrast imaging which is a weakness in articular cartilage assessment and it is done on a 3T machine.
HOAMS scoring system2 scores 14 different articular features including cartilage morphology,
subchondral bone marrow lesions,
subchondral cysts,
osteophytes,
acetabular labrum,
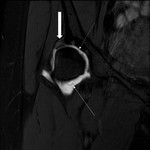
synovitis (Figure 4),
joint effusion,
loose bodies,
attrition,
dysplasia,
labral hypertrophy (Figure 5),
trochanteric bursitis or insertional tendonitis of the greater trochanter (Figure 6),
paralabral cysts and herniation pits.
According to HOAMS scoring system2 hip joint is divided on 15 subregions for evaluating subchondral bone marrow lesions and subchondral cysts (Figure 7A,
7C),
on 9 subregions for scoring articular cartilage (Figure 7B and 7D),
5 definitive locations for assessing osteophytes and labrum and 4 definite locations for assessing synovitis.
Although HOAMS scoring system includes all known features of degenerative changes and even some possible causes for OA evaluating all 14 features can be quite time consuming.
HOAMS is based on 1,5T imaging without use of contrast however in case of synovitis they applied intravenous contrast to correctly score given features.
Neumann`s scoring system3 on the other hand marks only 6 features including articular cartilage,
labrum,
bone marrow edema,
osteophytes,
subchondral cysts and subchondral sclerosis.
Using only 6 features reduces its` sensitivity compared to the other two.
Neumann et al.3 divided hip into five compartments for assessing features of their scoring system (Figure 8).
Neumann`s scoring system is the only scoring system based on direct MR arthrography where all pacients receive contrast and is developed on 1,5T imaging.
The three scoring systems differ in number of evaluated features,
use of intraarticular or intravenous contrast,
usage of 1,5T or 3T imaging.
They also subdivide hip joint regions differently.
Another difference in aforementioned scoring systems is the grading scale for scoring articular cartilage.
Scoring system by Neumann et al.3 uses 6-point scale to score articular cartilage while HOAMS2 uses 5-point scale which enables better accuracy in reporting and scoring.
On the other hand,
SHOMRI1 uses simplified 3-point scale which enables better time efficiency and ease of use on dispense of accuracy.
More accurate grading systems are shown in Table 1.
|
SHOMRI scoring system
|
HOAMS scoring system
|
Neumann`s scoring system
|
|
Cartilage damage
0-normal
1-partial thickness loss
2-full thickness loss
|
Cartilage damage
0-normal
1-focal partial thickness defect
2-focal full thickness defect
3-several partial thickness defects
4- several large full thickness defects
|
Cartilage damage Size
0-normal A <1cm
1-signal B 1-2cm
heterogenity C 2-3cm
2-fissuring D3-4cm 3-thinning<50%E>4cm 4-thinning>50%
5-full thickness loss
|
|
Bone marrow lesions
0-absent
1-less than 0,5cm
2-0,5cm-1,5cm
3-greater than 1,5cm
|
Bone marrow lesions(% of subregional volume)
0-absent
1-mild (<33%)
2-moderate(33-66%)
3-severe (>66%)
|
Bone marrow lesions
0-absent
1-less than 0,5cm
2-0,5cm-1,5cm
3-greater than 1,5cm
|
|
|
Osteophytes
0-absent
1-questionable
2-small beak-like definite
3- intermediate-size
4-proliferative large osteophyte
|
Osteophytes
0-absent
1-1-2mm
2- 2-5mm
3- >5mm
|
|
Labrum
0-normal
1-intralabral abnormal signal
2-simple tear
3-labrocartilage separation
4-complex tear
5-maceration
|
Labrum
0-no signal changes
1-intralabral signal alteration
2-definitive labral tear
3-partial/complete labral maceration
|
Labrum
0-normal
1-intrasubstance degeneration
2-simple tear
3-complex tear
4-diminutive apperance of labrum
|
|
Subchondral cyst
0-absent
1-less than 0,5cm
2-greater than 0,5cm
|
Subchondral cyst (% of subregion volume)
0-absent
1-mild (<33%)
2-moderate(33-66%)
3-severe (>66%)
|
Subchondral cyst
0-absent
1- <2cyst
2- 3-4cyst
3- >5cyst
|
|
Loose bodies,
0-absent
1-present
|
Loose bodies
1-single loose body
2-two loose bodies
3- three or more loose bodies
|
|
|
Ligamentum teres
0-normal
1-signal abnormalities
2-partial tear
3-complete tear
|
Synovitis (with intravenous applied contrast)
0-synovium thickness <2mm
1- synovium thickness 2-4mm
2- synovium thickness >4mm
|
|
|
Joint effusion,
paralabral cyst
0-absent
1-present
|
Joint effusion,
attrition,
dysplasia of the hip,
trochanteric bursitis,
labral hypertrophy,
paralabral cysts,
herniation pits
0-absent
1-present
|
Subchondral sclerosis
0-absent
1-present
|
Another discrepancy between scoring systems is variance in correlation of their findings.
Standard of clinical application is correlation to surgical or pathologic findings.
The only semi-quantitative MRI scoring system that correlated their findings to surgical outcomes was scoring system by Neumann et al.3 and even they had available surgical outcomes for only 23 out of their 100 patients.
Furthermore they did not include correlation to other OA parameters such as radiographs or clinical symptoms.
SHOMRI1 and HOAMS scoring systems2 on the other hand correlated their findings only to radiographic and clinical parameters.
Of the latter two,
SHOMRI scoring system2 correlated significantly with radiographic scores and clinical parameters while in HOAMS scoring system1 there was no significant correlation between MRI findings and clinical outcomes.
Regarding reproducibility SHOMRI scoring system1 is most reproducible with intraclass correlation coefficient from 0.93 to 0.98 for intra–reader reliability and from 0.91 to 0.94 for inter– reader reliability.
Other two systems had lower coefficients.