Radiological diagnosis:
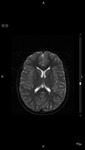
MRI
Although historically visible on myelography,
cross-sectional imaging (especially MRI) is needed to diagnose accurately and assess for Chiari I malformations,
for that reason the technique of choice is magnetic resonance imaging (MRI) for the diagnosis in both symptomatic and asymptomatic patients.
Fig. 9
In either case,
the diagnosis is made by measuring how far the tonsils protrude below the margins of the foramen magnum.
The distance is measured by drawing a line from the inner margins foramen magnum,
and measuring the inferior most part of the tonsils.
Some authors say that tonsils above foramen magnum,
and tonsillar ectopia <3 mm are normal,
between 3 to 6 mm are indeterminate,
and needs to be correlated with symptoms and presence of syrinx,
finally a tonsillar descente of >6 mm are considered (CM-I).
Ohter authors advocate a simpler rule,
above foramen magnum are normal,
tonsillar descent <5 mm are also normal and tonsillar descent of >5 mm are considered (CM-I).
MRI volumetric studies of the posterior fossa and studies of flow dynamics can also be performedmay also be useful to assess flow surrounding the cervicomedullary junction,
because the secuence provide quasi-real-time dynamic assessment of the CSF flow characteristics.
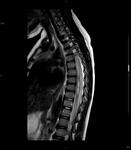
The diagnosis of syringomyelia should be made by a complete spinal MRI (cervical,
dorsal and lumbar). Fig. 6 Fig. 4
CSF flow abnormalities
Several investigators have studied CSF flow abnormalities in Chiari I malformation.
A prolongation of CSF systole is observed in the area above the foramen magnum.
In the anterior subarachnoid space below the foramen magnum and in the posterior subarachnoid space immediately below the tips of the cerebellar tonsils,
systolic velocities are reduced,
and the duration of CSF systole and the ratio of systolic-to-diastolic CSF displacement are decreased.
These findings indicate impaired CSF systolic (craniocaudal) pulsations.
Diastolic flow is unimpaired.
A reduction of CSF flow can be observed in the subarachnoid space of the posterior cranial fossa (cisterna magna; retrocerebellar,
premedullary,
and prepontine cisterns),
along with a compensatory pulsatile downward motion of the cerebellar tonsils.
These flow abnormalities have been shown to revert to normal levels after cranial decompression.
However,
CSF flow abnormalities are not correlated with the degree of tonsillar ectopia or the presence of clinical symptoms or their severity.
Fig. 13
Protocols:
A useful MRI protocol for preoperative and postoperative evaluation of Chiari I malformation may include axial and sagittal T1-and T2-weighted fast spin-echo sequences,
sagittal cardiac-gated phase contrast cine-mode images,
sagittal cardiac-gated cine true fast imaging with steady-state precession (true FISP),
and sagittal high-spatial-resolution cisternography sequences.
In addition,
DW images and FLAIR are useful for acute infarcts,
and contrast-enhanced T1-weighted sequences may be included if infection is suspected.
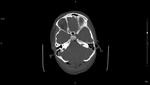
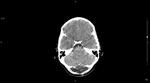
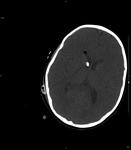
CT
Cranial CT: is useful for the control of hydrocephalus and postoperative controls and also TC helps to find obliterated cisterna magna,
hydrocephalus,
flattened spinal cord,
tonsillar ectopia,
peglike cerebellar tonsils,
normally positioned fourth ventricle.
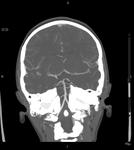
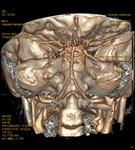
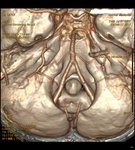
Angio-CT: is used for the assessment of the vascular system,
especially the vertebrobasilar axis.
It is very important evaluate the variants of normality or any vascular anomaly that could change the surgical procedure.
Fig. 10 Fig. 11 Fig. 12
CT can also be used to assess associated bony abnormalities of the skull base and vertebral column.
CT scanning may be of value in patients in whom MRI is absolutely contraindicated
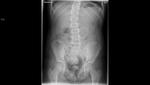
X-rays:
X-rays are used to study bone abnormalities and to perform catheter controls if necessary to place a bypass valve. Fig. 18 Fig. 17
Treatment:
Some Chiari malformations are asymptomatic and do not interfere with the person's daily activities.
In other cases,
medications can relieve certain symptoms,
such as pain.
Surgery is the only treatment available to correct functional disturbances or stop the evolution of damage in the central nervous system.
There are several techniques to treat this malformation,
but all have in common the decompression of the foramen magnum that serves to create more space for the cerebellum and decrease the pressure on the spine. Fig. 14 In general,
decompression is achieved through a suboccipital incision in the midline,
which goes from the occipital protuberance to approximately the third cervical vertebra.
After resecting the bony portion,
usually is an abnormally thickened membrane that acts as an element of constriction of the meninges at this level,
It is called atlanto-occipital membrane and should be removed for the most part,
also depending on the neurosurgeon decompression can be completed by a duroplasty Fig. 15 .
Hydrocephalus can be treated with a bypass system that drains the CSF and decreases the PICs.
The surgery consists of the placement of an intraventricular drainage tube,
surgically inserted connecting to a flexible tube that is placed under the skin,
where it can drain CSF into the chest or abdomen where the CSF is absorbed Fig. 16
In cases of syringomelia,
surgeons can insert an intramedullary shunt to maintain continuous drainage.