We will illustrate anatomical and clinical significances of cortical branches and critical perforating arteries including the internal carotid artery (ICA),
ophthalmic artery (OA),
vertebral artery (VA),
basilar artery (BA),
anterior cerebral artery (ACA),
middle cerebral artery (MCA),
and posterior cerebral artery as listed in Fig.
4 depicted by UHRCT.
Imaging Acquisition
CT scanner; Aquilion Precision™; Toshiba Medical Systems,
Tokyo,
Japan
Scan parameters and image reconstruction; We present scan and image reconstruction parameters in Table 1.
Injection method; We place a 20-G needle in the right antecubital vein of the patient.
At the beginning,
we inject 10 ml each of high concentration (350 mgI/ml) contrast medium and saline as a test injection using a power injector,
and measure the peak time of M1 segment of the MCA.
Subsequently,
the administration is performed using a high concentration contrast medium at the fractional dose of 30 mgI/kg/sec for 15 seconds,
then saline flash of 40 ml was injected at the same rate.
Scan is started at the M1 peak time.
Findings
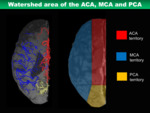
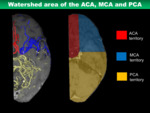
The cerebrum is mainly perfused by three pairs of main cerebral arteries; the ACA,
MCA and PCA.
As UHRCT has enabled depiction of cortical branches of these main arteries,
it is possible to identify the watershed area that is the boundary of perfusion area of each main cerebral artery (Figs.
5,
6).
Furthermore,
UHRCT has made it possible to depict critical perforating arteries.
We will explain the anatomical significance and clinical significance of the intracranial cortical branches and perforating arteries below.
<Internal carotid artery>
1) Ophthalmic artery
- Anatomical characteristics
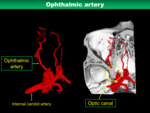
The OA is the first branch of the intracranial ICA and often originates from inside the anterior wall at the distal dural ring of the ICA and run inward of the optic nerve and passes anteriorly through the optic canal and the orbit (Fig.
7).
- Clinical significance
The origin and route of the OA affect the site of occurrence and protrusion direction of the ICA-OA bifurcation aneurysm.
By them the extent to which the aneurysm compress and shift the OA is different.
So,
identification of origin and route of the OA is important in considering the posture and approach in order to ensure a sufficient field of view for direct surgery.
The central retinal artery is the first branch of the OA and supplies the inner retinal layers and related to visual function.
It is important that the OA is usually one end-artery with poor vascular anastomosis,
but it is difficult to visualize on CTA because the diameter is extremely small.
2) Posterior communicating artery
- Anatomical characteristics
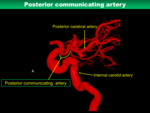
The posterior communicating artery (PCoA) passes between the ICA and the PCA,
and becomes a collateral between the anterior and the posterior circulations (Fig.
8).
Depending on the relationship between the diameter of the PCoA and the P1 segment of the PCA,
it is classified into the following three types.
Normal type: the diameter of the PCoA is 1 mm or more and narrow than the P1 segment.
Hypoplastic type: the diameter of the PCoA is 1 mm or less.
Fetal type: the diameter of the PCoA is 1 mm or more and larger than the P1 segment.
- Clinical significance
About seven perforating arteries arise from the upper wall of the PCoA and supply the optic tract,
the optic chiasm,
the mammillary body,
the gray tuber,
the posterior part of the hypothalamus,
the anterior part of the thalamus,
the genu of internal capsule and anterior third of the posterior limb of internal capsule.
If the PCoA gets occluded,
it causes hemiplegia,
hemisensory disturbance,
alalia,
memory disturbance,
affective disorder,
and visual field disturbance.
The role of collateral is irrelevant to the diameter of the PCoA,
and the damage by surgery tends to occur in cases where the diameter of the PCoA is narrow [1].
As many perforating arteries arise from the anterior part of the PCoA,
if you have to sacrifice the PcoA by surgery,
the PCA side is safer.
Usually,
the oculomotor nerve exists lateral inferior of the PCoA,
but there are many variations in the positional relationship between the oculomotor nerve and the PCoA,
so attention is required during surgery.
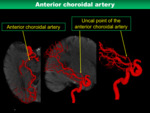
3) Anterior choroidal artery
- Anatomical characteristics
The anterior choroidal artery (AchoA) originates from the posterior wall of the ICA slightly distal from the origin of the PCoA.
The AchoA runs to the posterior medial side and passes through the inferior of the optic tract,
and goes upward drawing a S-shaped curve passing outside the cerebral peduncle.
Then it forms a convex vertex upwards and enters the choroidal fissure.
The top of AChoA is called the uncal point (Fig.
9).
- Clinical significance
Branches of AchoA supply medial temporal lobe,
optic tract,
middle third of cerebral peduncle,
posterior two-thirds of posterior limb of internal capsule,
lateral geniculate body and choroid plexus.
Therefore,
if the ACoA get occluded,
it causes hemiplegia,
hemisensory disturbance and hemianopia.
It is known as Abbie or Monakow syndrome. Especially,
as the collateral of posterior limb of internal capsule is poor,
hemiplegia appears with high probability when the AChoA is occluded.
Since all these branches of AchoA originate proximal to the uncal point,
identification of the uncal point is important during transcatheter embolization.
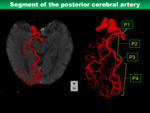
<Posterior cerebral artery>
The PCA originates from the distal end of the BA,
and it is divided into four segments (Fig.
10).
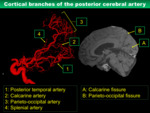
Cortical branches of the PCA (Fig.
11)
1) Temporal arteries
- Anatomical characteristics
Temporal arteries are classified into the hippocampal artery,
anterior temporal artery,
middle temporal artery,
posterior temporal artery and common temporal artery depending on the region of the temporal lobe which is supplied.
- Clinical significance
They supply the ventral surface of the temporal lobe and anastomose with branches of the MCA.
2) Parieto-occipital artery
- Anatomical characteristics
The parieto-occipital artery arises from the P3 segment,
and runs inside of the parieto-occipital fissure and supply the parietal lobe,
the posterior medial part of occipital lobe,
the cuneus and the pre-cuneus.
- Clinical significance
The posterior pericallosal artery branching from parieto-occipital artery runs on the superior surface of corpus callosum and anastomoses with the pericallosal artery which branches from the ACA.
As in moyamoya disease,
this branch often develops working as collateral pathways.
3) Calcarine artery
- Anatomical characteristics
The calcarine artery arises from the P3 segment,
and runs through the calcarine fissure.
- Clinical significance
It supplies the major part of the visual cortex,
and it is important to identify this artery before surgery for preservation of visual function.
4) Splenial artery (posterior pericallosal artery)
- Anatomical characteristics
The splenial artery runs on the superior surface of the corpus callosum.
- Clinical significance
It supplies the splenium of the corpus callosum.
Perforating arteries of the PCA
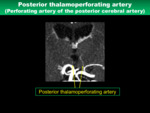
5) Posterior thalamoperforating artery
- Anatomical characteristics
The posterior thalamoperforating artery originates from the top of BA or P1 segment,
and its diameter on average is 0.7 mm (Fig.
12)
- Clinical significance
It supplies the internal thalamus and the midbrain.
Its branch originating from the P1 segment that supplies both sides of the thalamus and midbrain is called the artery of Percheron.
If it is occluded,
bilateral paramedian thalamic infarction syndrome is caused even by one side of the P1 occlusion,
resulting in disturbance of consciousness and ocular movement disorder such as vertical gaze paresis and convergence palsy.
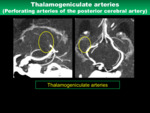
6) Thalamogeniculate arteries
- Anatomical characteristics
Thalamogeniculate arteries arise from P2 segment,
and diameter of this arteries are 0.2-0.4 mm (Fig.
13).
- Clinical significance
They supply the geniculate nucleus,
pulvinar,
posterior part of the thalamus,
posterior limb of internal capsule,
superior colliculus and optic tract.
So,
obstruction of this arteries causes disturbance of contralateral superficial and deep sensibility,
severe thalamic pain,
light hemiplegia and involuntary action known as Dejerine-Roussy syndrome.
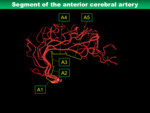
<Anterior cerebral artery>
The ACA is smaller and more medial terminal branch of supraclinoid ICA,
and it can be classified into five segments (Fig.
14).
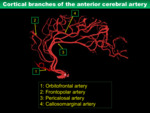
Cortical branches of the ACA (Fig.
15)
1) Orbitofrontal artery
- Anatomical characteristics
The orbitofrontal artery is usually the first cortical branch of the A2 segment,
and ramifies over inferior surface of frontal lobe.
2) Frontopolar artery
- Anatomical characteristics
The frontopolar artery is the next cortical branch arising from the mid-A2 segment over the corpus callosum,
and extends anteriorly to the frontal lobe.
- Clinical significance
Both the orbitofrontal and the frontopolar arteries are orbital branches and supply over the orbital surface of the frontal lobe: olfactory cortex; gyrus rectus; medial orbital gyrus.
3) Pericallosal artery
- Anatomical characteristics
The pericallosal artery arises from the A2 segment near the corpus callosum genu,
and runs posterosuperiorly above the corpus callosum.
- Clinical significance
It gives off many small branches to the corpus callosum.
4) Callosomarginal artery
- Anatomical characteristics
The callosomarginal artery arises from the A3 segment and runs posterosuperiory in the cingulate sulcus.
- Clinical significance
The pericallosal-callosomarginal arterial junction is the site of predilection for distal anterior cerebral artery aneurysm (DACAAN).
In the case of DACAAN,
the operative field is narrow.
Particularly when the aneurysm exists below the corpus callosum genu,
it is difficult to reach the parent artery,
so it is important to understand the location of the aneurysm and the direction of protrusion before surgery.
Perforating arteries of the ACA
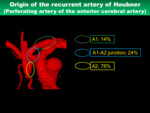
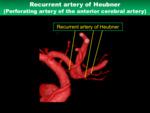
5) Recurrent artery of Heubner
- Anatomical characteristics
The recurrent artery of Heubner arises typically from the nearby A1-A2 junction,
and curves back parallel to the A1 segment.
The diameter of this artery is 0.8-1.0 mm (Figs.
16,
17).
- Clinical significance
It supplies the anterior part of the caudate nucleus and putamen,
anterior limb of internal capsule and fasciculus uncinatus.
Obstruction of this artery causes facial paralysis,
upper-limb hemiparesis and aphasia on dominant side.
6) Medial lenticulostriate arteries
- Anatomical characteristics
The medial striate arteries (MSAs) are generally arising from the A1 segment.
- Clinical significance
The MSAs supply the globus pallidus and medial part of the putamen.
Although,
some investigators divide the lenticulostriate arteries that arise from the M1 segment into medial (those arising proximally) and lateral (those arising more distally) groups.
In fact,
the frequency of occurrence of the MSAs is low,
and clinically the infarction of this perfusion area is rare.
<Middle cerebral artery>
The MCA arises from the ICA and continues to the lateral sulcus where it then branches and projects to many parts of the lateral cerebral cortex.
The MCA supplies the majority of the lateral surface of the hemisphere,
except the superior portion of the parietal lobe and the inferior portion of the temporal and occipital lobes.
In addition,
it supplies part of the internal capsule and basal ganglia.
In its territory lie the motor and sensory areas excluding leg and perineum and auditory and speech areas.
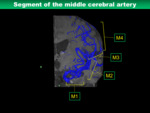
The MCA are classified into four segments (Fig.
18). M4 segment coursing over surface on the cortex are cortical branches and those names are based on their perfusion area (Fig.
19).
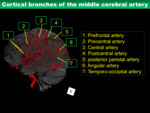
Cortical branches of the MCA
Supply the anterior lobe
1) Orbitofrontal artery
2) Prefrontal artery
3) Precentral artery
4) Central artery
Supply the parietal and occipital lobe
5) Postcentral artery
6) Posterior parietal artery
7) Angular artery
Supply the temporal and occipital lobe
8) Temporo-occipital artery
9) Posterior temporal artery
10) Middle temporal artery
11) Anterior temporal artery
12) Temporopolar artery
Perforating arteries of the MCA
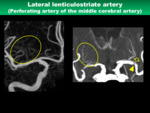
13) Lateral lenticulostriate artery
- Anatomical characteristics
The lateral lenticulostriate artery (LSA) usually arises from the mid- and distal M1 segment (Fig.
20).
Variations of origin are as follow: M1,
40%; both M1 and M2,
20%; M2,
25%; M1-2 bifurcation,
12% and accessory MCA,
3%.
Branching patterns are also variable as follows: branching from one trunk,
40%; branching from two trunks,
30%; direct branching from M1 segment,
30% [2].
- Clinical significance
LSAs are small perforating arteries with a diameter of 0.5 mm or less,
but they supply very important areas such as the caudate nucleus,
the globus pallidus,
the putamen and the part of the posterior limb of internal capsule.
These small arteries are particularly susceptible to damage from hypertension.
They may rupture,
resulting in an intracerebral hemorrhage that is initially centered in the region they supply.
Especially,
outermost branch of LSAs is known as Charcot-Bouchard artery that commonly causes external putamen hemorrhage with hypertension.
Moreover,
LSAs are "end arteries",
meaning that the regions they supply do not have significant collateral blood supply.
When occluded,
it produces a lacunar infarct in the tissue they supply.
The origin of LSA is also a common site of MCA aneurysm.
So,
in the case of M1/M2 stenosis or before surgery of aneurysm or brain tumor,
it is important to understand the origin and branching of LSAs.
<Basilar artery>
The BA courses superiorly in the prepontine cistern.
Branches of the BA
1) Anterior inferior cerebellar artery
- Anatomical characteristics
The anterior inferior cerebellar artery (AICA) usually arises from the proximal BA.
- Clinical significance
The AICA supplies anterolateral part of the cerebellum.
2) Superior cerebellar artery
- Anatomical characteristics
The superior cerebellar artery (SCA) arises from the distal BA,
and course posterolaterally around the midbrain.
- Clinical significance
The SCA supplies the superior vermis,
superior cerebellar peduncle,
dentate nucleus,
brachium pontine,
superomedial surface of cerebellum and upper vermis.
3) Posterior cerebral artery
Refer to the PCA.
Perforating arteries of the BA
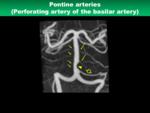
4) Pontine arteries
- Anatomical characteristics
Usually 3-5 pair branches arising from the BA between the AICA and SCA (Fig.
21).
- Clinical significance
Pontine arteries supply the pons and anatomies adjacent to the pons.
The pontine arteries arising from the lower third of the BA supply the foramen cecum and medulla oblongata,
and thus are especially important because their obstruction can lead to severe motor paralysis.
<Vertebral artery>
After the VA enters skull through foramen magnum is V4 segment,
and unites with the contralateral VA at pontomedually junction to the BA.
Branches of the VA
1) Posterior inferior cerebellar artery
- Anatomical characteristics
The posterior inferior cerebellar artery (PICA) arises from distal VA.
It curves around tonsil,
and gives off perforating medually,
choroid,
tonsillar and cerebellar branches.
- Clinical significance
The PICA supplies lateral medulla,
choroid plexus of fourth ventricle,
tonsil and inferior vermis and cerebellum.
Perforating artery of the VA
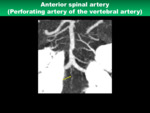
2) Anterior spinal artery
- Anatomical characteristics
The anterior spinal artery (ASA) arises from the VA at the level of the medulla oblongata and descends along the anterior median fissure located on the anterior surface of the spinal cord (Fig.
22).
- Clinical significance
The ASA supplies the anterior portion of the spinal cord.
Occlusion of it causes anterior spinal artery syndrome.