Global concepts
SFT represents an uncommon type of neoplasm with mesenchymal origin,
accounting for approximately 1%-2% of all tumours located in soft tissues.
Initially,
it was believed to affect exclusively the pleura,
however,
in the recent years,
numerous cases with extrapleural localization have been described,
rising to approximately 40% of all cases [1],
involving practically every organ system.
Histologically,
SFT is composed of a fusocellular proliferation (fibroblasts,
myofibroblastst),
admixed with an extracellular hyaline matrix and vascularization.
Different subtypes according to the dominating component are described,
being the most common forms those which vary from a more cellular (SFT) to a more fibrotic content (Giant Cell Angiofibroma).
Hemangiopericytoma is also considered as a subtype of SFT according to the last WHO soft tissue tumours classification,
representing a mesenchymal fibroblastic neoplasm with a prominent vascular component in a characteristic (‘hemangiopericytoma-like’) pattern [2].
Macroscopic fat has also been described in uncommon forms of SFT (lipomatous hemangiopericytoma).
Clinically it appears as a slow growing mass,
commonly asymptomatic,
but sometimes associated with compressive local effects depending on size and localization.
Despite appearing typically at middle age,
the age of presentation includes a wide range.
No clear sex predilection has been described in the literature.
At imaging,
the finding of a solid well-defined lesion,
with variable size,
located deeply in the abdominal cavity or proximally in extremities and with a hypervascular behavior,
suggests the diagnosis of soft tissue SFT.
The complete resection represents the treatment of choice,
with a 5-year survival rate of nearly 100%.
Surgical resecability is the most important factor in terms of prognostic impact.
According to some series,
up to 53% of cases present histopathological characteristics of malignancy,
with local relapse and metastatic taxes of 20% and 36% respectively [3].
Clinical results in our study
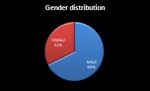
In our study,
the gender distribution showed male predominance (3:1) (fig.
1).
The mean age at presentation was 51 years old,
being the minimum and maximum age of 24 and 78 y.o.
respectively.
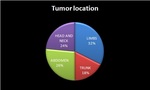
The most common localization was the extremities (32%),
followed by the abdominal cavity (26%),
head and neck (24%),
and less frequently the trunk (18%) (fig.
2).
Considering depth,
75% were located in deep planes,
taking the muscular fascia as a reference in most cases.
Mass sensation was the most usual form of presentation (70%).
Incidental finding represented a 14% of cases.
The remaining patients presented pain and other symptoms due to mass efect (f.e.
deep venous thrombosis in a retroperitoneal lesion,
dysphonia and dysphagia in when located laterocervical and burning sensation in a lesion located superficially at the thigh).
Sistemic symptoms such as secondary hypoglycemia (Doege-Potter syndrome) or hypertrophic osteoarthropathy [3] were not registered.
One case with pulmonary metastasis at diagnosis was found.
Radical exersis of the tumour represented the main therapeutic option.
Cases with positive margins after resection,
local compressive effects or invasion to adjacent structures were treated with complementary radiotherapy.
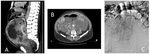
Previous embolization to surgery was performed in a huge and hypervascularized lesion to reduce the risk of intraoperatory haemorrhage (fig.
8).
Unresectable tumours and cases with multiple metastases were treated with chemotherapy.
A case with a unique pulmonary metastasis was resected (fig.3).
The mean time for radiological surveillance was 52 months (maximum and minimum of 144m and 7m respectively).
Depending on the localization and the extension of the tumour,
different imaging modalities were used.
Non disseminated disease was controled with CT if located at trunk or head and neck,
and with MRI if located at limbs.
Cases with metastatic disease were controled with PET-CT.
A total of 6 patients developed metastasis,
5 of them being metachronic and 1 synchronic.
The mean of distant-disease-free interval was 56 months,
including a wide range of time (5 to 120 months).
3 cases of local relapse after surgery were registered,
with a mean of local-disease-free interval of 31 months.
Histopathological results
Of the 36 patients included in our series,
13 (36%) presented at least one pathologic characteristic of malignancy (mitotic index > 10 x 10 HPF,
cellular atypia or tumoral necrosis).
KI-67 proliferation index was also registered.
In this group of patients,
superficial localization was slightly more frequent than in cases without malignant hystopathologic characteristics (fig.
4 & 5).
Radiological results
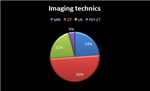
The most used imaging modality in our series (fig.
6) was CT (50% of all explorations),
due to the high quality images obtained to evaluate different radiological features of the tumor.
In certain localizations such as trunk and head and neck,
CT presented a similar efficiency to MRI for tumor characterization.
MRI represented the 24% of all explorations,
and was basically used in primary diagnosis and surveillance for lesions located at limbs,
but used in any localization as a complement to CT.
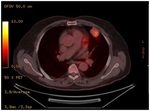
Finally,
PET-CT only represented the 4% of all explorations,
mainly for metastatic disease and for surveillance (fig.
3).
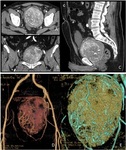
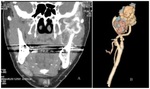
At CT,
soft tissue SFT appears as a solid well-defined lesion,
with avid enhancement,
often heterogeneous due to the presence of cystic/necrotic areas (fig.
7 to 13).
Mass effect to contiguous structures was common,
as SFT can achieve big sizes (almost 30cm).
Presence of calcification visible on CT has been described in the literature [4,
6].
In our series calcification was present in two cases.
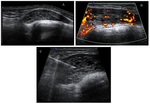
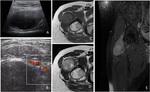
At ultrasound,
sort tissue SFT appears as a heterogeneous well-defined lesion,
predominantly hypoecogenic,
hypervascularized with prominent perilesional vessels,
visible in different modalities.
Evidence of a vascular pedicle was visible in nearly a 50% (13/27) (fig.
9 to 12).
In some series,
perilesional vessels have been described in every single lesion conscientiously studied [5],
and despite being an unspecific finding,
becomes a useful diagnostic feature [3].
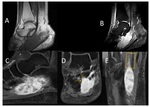
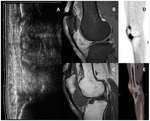
At MRI,
soft tissue SFT shows T1 isointensity or mild hypointensity compared to muscle.
T2 signal intensity (SI) turns to be variable according to the histologic composition; tumors with high fibrotic content,
show low T2 signal.
In malignant tumors,
high T2 SI is observed due to vascularization and edema [2].
MRI is almost useful in determining depth with regard to the muscular fascia,
thanks to its spatial resolution compared to other modalities.
Invasion to contiguous structures is also valuable with MRI.
At least 5 cases showed local invasion,
which correlated with big size (>10 cm) and signal heterogeneity (fig.
8,
10 & 12).
Enhancement pattern varies according to cellularity,
vascularization and fibrous stroma density.
Hypervascular areas show avid enhancement,
where as cellular component show a less avid but more persistent enhancement.
Fibrous stroma show poor enhancement at early phases,
but increasing progressively and being evident at later phases.
Correlation
In all cases developing metastasis with images of the primary lesion (4 of 6),
the size of the SFT was higher than 10 cm.
At least one pathological characteristic of malignancy was present in all patients.
This fact diverged clearly with benign lesions (fig.
14).
Despite this correlation,
some series describe cases with late local relapse and metastases in histologically benign lesions,
suggesting an unpredictable biologic behavior.
Therefore,
long term surveillance is strongly recommended [3].