Leiomyomas are the most common gynaecological and uterine neoplasm,
affecting up to 20 to 30% of women over the age of 351.
Case 1: Urethral leiomyoma
Clinical history:
Patients may present with a long history of right iliac fossa pain and alternating bowel habit.
Imaging:
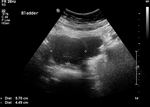
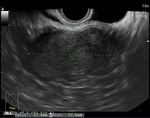
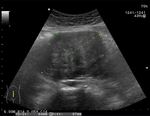
Ultrasound: This typically shows a hypoehocic mass noted posterolateral to the base of the bladder.
Fig. 1
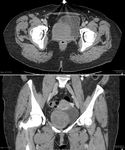
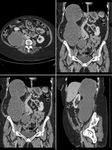
CT: This typically shows a mass arising from the pelvis which indents one side of the bladder,
can appear inferior to the uterus or may appear separate from it. Fig. 2
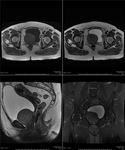
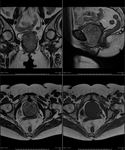
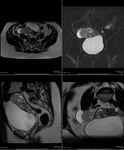
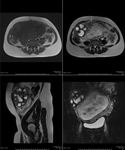
MRI Pelvis: A well-defined right sided pelvic mass can be demonstrated arising from the urethra.
It is isointense on T1 and T2 with multiple hypointense internal foci.
No adjacent oedema is found. Fig. 3 Fig. 4
Differential diagnosis:
Urothelial lesion
Transitional cell carcinoma
Summary:
Urethral leiomyoma is an uncommon presentation of extrauterine leiomyoma with approximately 120 cases reported in the literature. At ultrasound,
the tumors appear homogeneous,
solid and smooth walled and have a typical whorled appearance.
At MR imaging,
the tumors have intermediate signal intensity on T1-weighted images and low to intermediate signal intensity on T2-weighted images,
in addition,
they enhance homogeneously after the administration of contrast material2.
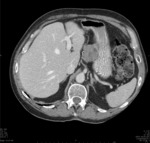
Case 2: Gastric leiomyoma
Clinical history:
Patients typically present with gastrointestinal discomfort and anaemia.
Imaging:
CT: Most gastric leiomyomas present as endogastric submucosal lesions and may be pedunculated,
however they may also present as an exopytic mass if they originate from the serosa (as per our case). Fig. 5
Differential diagnosis
GIST
Schwannoma3
Summary:
Leiomyomas are almost always seen in the gastric cardia as homogeneous,
low-attenuation masses with an endoluminal growth pattern up to 5cm in diameter.
Tumours larger than 2 cm can have central ulceration.
Case 3: Intravenous leiomyoma
Clinical history:
Patients typically present with normal symptoms of uterine leiomyomas,
however,
they can present with syncopal episodes,
if the leiomyoma spreads to the heart.
Imaging:
US: Patients can present with a mass situated at the fundus of the uterus,
this consists of mainly homogeneous internal echoes Fig. 6.
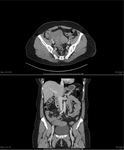
CT: Typically appears as a well defined mass which is isoattenuating to the muscle (as per our case) Fig. 7 .
It can also contain calcification.
MRI: Patients may present with a complex solid/cystic mass in the right adnexa.
Fig. 8
Summary:
It is characterized by intravascular proliferation of benign smooth muscle,
either in the absence of a leiomyoma or beyond the limits of a leiomyoma.
It can arise either by extension of a leiomyoma into adjacent veins or by vascular intimal smooth muscle proliferation.
Because of its atypical location it can mimic malignancy,
and can be a histological rather than radiological diagnosis4.
Case 4: Benign metastasising leiomyoma in a pregnant uterus
Clinical history:
Our patient presented with an enlarged gravid uterus with multiple bilateral pedunculated fibroids with degenerative changes.
US: Incidentally on a dating scan,
a well circumscribed mass,
hypoechoic to the myometrium was identified Fig. 9 .
MRI: Multiple masses in the abdomen and pelvis were noted.
They cause
mild mass-effect on the left kidney and displaced the abdominal contents to the right.
There is a mass of intermediate size related predominantly to the anterior abdominal wall.
These have a thick and low signal wall with disorganised internal architecture containing multiple irregular cystic spaces.
Some have internal content with mild increased T1 signal but there is no frank haemorrhage Fig. 10 .
Summary:
Benign metastasising leiomyomas are rare and are found typically in patients post hysterectomy.
They typically may present with nodules within the lungs,
however,
other sites include lymph nodes,
peritoneum and retroperitoneum5. Less commonly it can present with a miliary pattern.
Patients are normally asymptomatic,
but can present with a cough,
chest pain or dyspnoea.
Case 5: Retroperitoneal leiomyoma
Clinical History:
Our patient presented with a retroperitoneal mass.
Imaging:
CT: Multiple cystic masses were noted arising from the right retroperitoneum,
causing mass effect.
This was confirmed histologically as a retroperitoneal leiomyoma. Fig. 11.
Differential diagnosis:
Lymphadenopathy
Leiomyosarcoma
Summary
This is a rare entity of leiomyoma,
they are usually seen in patients with concurrent uterine leiomyomas.
They are most commonly seen in the pelvic retroperitoneum and can rarely extend into the upper retroperitoneum.
They typically present with non specific symptoms and tend to respond to hormones6.