Type:
Educational Exhibit
Keywords:
Musculoskeletal bone, Musculoskeletal soft tissue, Neuroradiology brain, CT, MR, Diagnostic procedure, Connective tissue disorders
Authors:
W. Morales Borrero1, L. R. Rodriguez-Ortiz2, F. G. Rodriguez-Ruiz3, A. Bravo4, J. Vidal2; 1San Juan/US, 2San Juan, PR/US, 3Caguas, Puerto Rico/US, 4San Juan, PR - PUERTO RICO/US
DOI:
10.1594/ecr2018/C-1320
Findings and procedure details
Central Nervous System
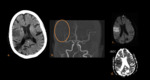
CNS Ischemia
Overview:
-
SLE is an independent factor for ischemic events in patients younger than 50 years of age.
[1]
-
Patients are most prone to suffer these events in the first 5 years following diagnosis.
[1]
-
Most common etiologies are cardiogenic emboli (i.e.
Libman-Sacks endocarditis),
antibody-mediated hypercoagulable state in Antiphospholipid Syndrome and platelet and fibrin thrombus formation.
[1]
-
Smaller lesions can be seen in cortical,
or deep gray,
areas believed to be secondary to endothelial hyperplasia and intimal fibrosis leading to vessel occlusion (a.k.a Lupus angiitis or Lupus vasculitis).
Clinical Manifestations:
-
Weakness
-
Dysarthria
-
Altered Mental Status
-
Hemiparesis
Imaging Findings:
-
Small infarcts are seen as hyperintense lesions on T2 weighted fluid-attenuated inversion recovery (FLAIR) imaging.
-
Larger infarcts can be seen on Computed Tomography (CT) or Magnetic Resonance Imaging (MRI).
-
-
Magnetic Resonance Arteriogram (MRA) with Time of Flight is a non-invasive imaging technique that helps to see if the vasculature is patent.
-
Diffuse weighted Imaging (DWI) can help in distinguishing between acute insults from chronic disease.
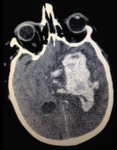
CNS Hemorrhage:
Overview:
-
Intracranial hemorrhages are associated with SLE.
-
Their development in young patients should raise the suspicion of SLE.
-
Large vessels are prone to suffer fibrinoid necrosis leading to vessel wall weakness and rupture.
[2]
-
Spontaneous intracranial hemorrhages in the setting of SLE are usually found intraparenchymal or within the subarachnoid space.
Clinical Manifestations:
-
Weakness
-
Dysarthria
-
Altered Mental Status
-
Hemiparesis
Imaging Findings:
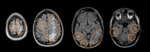
Posterior Reversible Encephalopathy Syndrome (PRES)
Overview:
-
Posterior Reversible Encephalopathy Syndrome (also known as Posterior Leukoencephalopathy Syndrome,
Reversible Posterior Cerebral Edema Syndrome,
Hyperperfusion Encephalopathy or Brain Capillary Leak Syndrome) is a neurologic syndrome composed of multiple etiologies that present similar findings on imaging studies and symptomatology.
-
Its pathogenesis remains unclear,
but is believed to be associated to aberrant cerebral autoregulation and endothelial dysfunction.
[5]
-
PRES is a rare presentation of SLE and it has been associated with hypertension,
lupus nephropathy and use of immunosuppressive drugs.
-
Prompt identification and treatment has been associated with regression.
[5]
Clinical Manifestations:
-
Headaches
-
Altered mental status
-
Seizures
-
Visual changes
Imaging Findings:
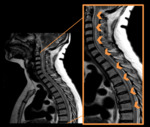
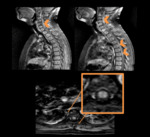
CNS Myelopathy
Overview:
-
Myelopathy is another rare complication of SLE that accounts up to 1-2% of patients.
-
Its most common manifestation is Transverse Myelitis,
a rapidly progressive demyelinating disease with motor,
sensory and autonomic involvement at a single (or multiple) levels of the spinal cord.
-
Clinical Manifestation:
Imaging Findings:
Cardiopulmonary System
Pericarditis
Overview:
-
Pericarditis is the most common manifestation of SLE in the heart.[1]
-
It mostly presents as a sterile pericardial effusion,
but it may progress to a purulent effusion,
with Staphylococcus aureus as the most common infectious pathogen.
-
Present in almost 40% of SLE patients.
[4]
-
Usually not a life-threatening sequelae,
but if untreated it may progress to constrictive pericarditis.
Clinical Manifestations:
-
Chest pain
-
Pericardial friction rub
-
EKG changes
-
Pericardial effusion
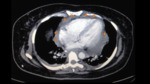
Imaging Findings:
-
Diagnosis by echocardiography is equivocal and insensitive unless an effusion is present.
-
On contrast-enhanced CT,
however,
it may present as thickening of the pericardium,
with or without associated effusions.
[2] (Fig.
6)
Coronary Artery Disease (CAD)
Overview:
-
CAD is among the complications of SLE with highest mortality (approximately nine times that of the general population).
[2]
-
Present in approximately 13%.
[4]
-
SLE patients are at an increased risk of developing SLE due to two possible mechanisms:
-
Clinical Manifestations:
-
Angina
-
Dyspnea
-
Diaphoresis
Imaging Findings:
Valvulopathy
Overview:
Clinical Manifestations:
Imaging Findings:
Acute Lupus Pneumonitis
Overview:
-
Pneumonic process of lung parenchyma without an identifiable infectious pathogen.
[7]
-
It may occur up to 12% of patients suffering from SLE.
-
Associated with high mortality.
-
Unimproved disease may progress to chronic pneumonitis which occurs in approximately 9% of patients.
[1]
-
Clinical and radiologic presentation may be confused with pulmonary hemorrhage.
Clinical Manifestations:
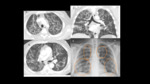
Imaging Findings: (Fig.
9)
-
On conventional radiographs,
pneumonitis may be seen as a patchy consolidation (i.e.
airspace infiltrates) with associated atelectasis,
pleural effusions and hemidiaphragm elevation.
[7]
-
-
On high resolution CT,
it may present as migratory densities,
ground-glass opacities and interstitial reticulation
Diffuse Alveolar Hemorrhage
Overview:
-
Pulmonary hemorrhage is a rare,
and deadly,
complication of SLE with a mortality rate of 50%.
[7]
-
It may initially present similar to acute pneumonitis or parenchymal infection,
making it difficult to differentiate in its early stages.
[1,2]
-
Clinical Manifestations:
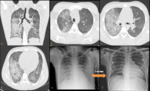
Imaging Findings: (Fig.
10)
-
On conventional radiographs,
hemorrhages can be seen as bilateral ,
symmetric,
ill-defined patchy opacities predominantly in the basal lungs.
[1,7]
-
-
On CT,
images may vary according to the chronicity of the disease:
-
Pulmonary Embolism
Overview:
-
SLE patients are at higher risk than their counterparts for developing pulmonary embolisms,
particularly if associated to Antiphospholipid Syndrome.
[2]
-
Mortality from PE can range as high as 65% within the first hour of onset.
[8]
Clinical Manifestations:
-
Dyspnea
-
Chest Pain (pleuritic)
-
EKG abnormalities
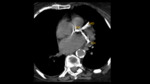
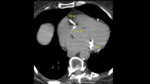
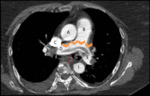
Imaging Findings:
-
On conventional radiographs,
acute pulmonary embolism may not show any visible manifestations.
-
On CT angiography,
pulmonary embolisms may present as intraluminal filling defects within the pulmonary vasculature.
(Fig.
11)
Gastrointestinal System
Lupus Enteritis
Overview:
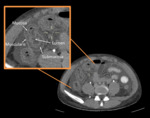
-
Lupus enteritis is a visceral vasculitis that typically involves the small bowel,
particularly the jejunum and ileum.
-
-
Prevalence documented in the literature is variable,
ranging from a rare to a common systemic manifestation in patients with SLE.
-
Proposed pathophysiology is immune complex deposition leading to inflammatory vasculitis and circulation of antiphospholipid antibodies leading to thrombosis of mesenteric blood vessels.
-
Also described as “lupus mesenteric vasculitis”,
“acute gastrointestinal syndrome”,
“mesenteric arteritis”,
and “lupus vasculitis”.
Clinical Manifestations:
Imaging Findings:
Renal System
Lupus Nephritis
Overview:
-
The kidneys are commonly affected organs in patients with SLE.
-
Common cause of death in patients with SLE.
-
Pathophysiology is the result of cross reaction of autoantibodies with antigens at the glomerular surface,
mesangial matrix or basement membranes,
and deposition of such complexes in the subepithelial and subendothelial glomeruli.
[2]
-
Clinical Manifestations:
Imaging Findings:
-
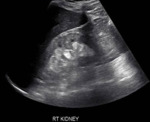
Imaging findings of acute renal manifestations of SLE in ultrasound and CT scan are considered nonspecific.
US can be used to identify and evaluate for progression of renal disease to scarring and atrophy,
although it has low specificity for identifying intrarenal causes in the setting of acute renal failure.
[12]
-
Evaluation with US may reveal normal,
decreased,
or increased size of the kidneys,
based on the duration of disease.
Echogenicity may be variable.
(Fig.
13)
-
Evaluation with CT scan can reveal chronic kidney changes such as atrophy and loss of corticomedullary differentiation.
[12]
Musculoskeletal System
Avascular Necrosis (AVN) of Bone
Overview:
-
Also known as osteonecrosis,
it is defined as the cellular death of bone tissue due to loss of blood supply.
Bone structures collapse as a result.
-
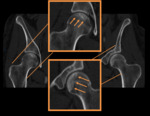
Most commonly affects the head of the femur,
particularly the superior sub-articular surface.
Also affects the head of the humerus,
the femoral condyle,
and the tibial plateau.
-
Can affect bilateral or unilateral joints.
-
Has been reported as a sequelae from corticosteroid therapy,
but it is also seen in patients that have not received such therapy.
[13]
-
Other factors associated with this manifestation include Raynaud’s phenomenon,
antiphospholipid syndrome,
fat embolism syndrome and vasculitis.
Clinical Manifestations:
-
May be asymptomatic during early stages.
-
Joint pain while performing weight bearing activities develops as necrosis progresses.
-
Leads to joint stiffness and limited range of motion.
-
Patients with avascular necrosis of the femoral head can present with pain localized to the groin,
buttock or thigh.
Steinberg Classification:
Imaging Findings:
-
Plain film radiography
-
-
Recommended views: ipsilateral and contralateral anteroposterior and frog-lateral views of the hip
-
May be normal during early stages of disease (Stage 0 and I)
-
Radiolucent and sclerotic changes are initial signs indicative of AVN (Stage II)
-
AVN progresses as follows:
-
-
Crescent sign: lucency in subchondral plate indicative of joint collapse (Stage III)
-
Flattening of the head of the humerus (Stage IV)
-
Involvement of the acetabulum (Stage V)
-
Degeneration of articular surface of the acetabulum and femoral head
Jaccoud Arthropathy
Overview:
-
Jaccoud arthropathy is a non erosive deforming joint disorder.
-
The causes for deformities are reversible and soft tissue related,
including ligament laxity,
capsular fibrosis,
and imbalances of the muscles.
[17]
-
-
Most commonly affects the metacarpophalangeal (MCP) and interphalangeal joints of the hand.
-
First described in patients with rheumatic fever,
later identified as a common manifestation in patients with SLE.
Clinical Manifestations:
Imaging Findings: