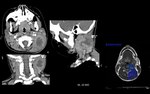
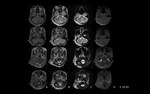
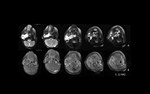
Imaging modalities
US is the initial imaging modality of choice,
as diagnosis can be achieved in many cases.
CT and MR may have a supplementary role,
mainly in profound and atypical lesions.
As CT has ionizing radiation and paediatric patients are especially susceptible to it,
optimal CT protocol is fundamental.
A CT protocol is suggested below.
|
Technical Parameters
|
|
kVp
|
120
|
|
Effective mAs
|
|
40-55
|
|
|
3-6 YO
|
55-70
|
|
|
6-12 YO
|
70-95
|
|
|
>12 YO
|
120
|
|
Time (rotation)
|
1.0
|
|
Average acquisition time
|
6-8 sec
|
|
Collimation
|
64x0.6 mm
|
|
Pitch value
|
0.8
|
|
Scan direction
|
Caudocranial
|
|
Slice thickness
|
3 mm
|
|
Contrast
|
|
Contrast material
|
Non-ionic,
low-osmolar at 300 mg I/ml of concentration
|
|
Standard dose
|
1.5 ml/kg
|
|
Injection rate
|
2.0 ml/sec
|
|
Fixed delay
|
30 sec after injection
|
Space by space approach
The neck can be divided by the hyoid bone in two anatomical compartments: supra-hyoid and infra-hyoid,
each of it can be further divided into spaces.
Each space has its anatomical components and typical lesions.
There is some continuation of supra-hyoid neck spaces into the infra-hyoid neck spaces,
and some continuation of some infra-hyoid neck spaces into the superior mediastinum.
In the study of neck lesions,
the systematic approach should answer to four questions:
- In which space is the lesion located?
- What are the contents of this space?
- What pathology arises from these contents and can we recognize a specific radiological pattern?
- Is the suggested pathology coherent with the clinical information?
Supra-hyoid neck
1. Pharyngeal mucosal space
Relations:
- medial to the parapharyngeal space
- anterior to the retropharyngeal space
Contents and Pathology:
|
Contents
|
Pathology
|
|
Squamous mucosa
|
Tumour
|
|
Lymphoid tissue (Waldeyer's ring)
|
Lymphoma,
abscess
|
|
Minor salivary glands
|
Tumour
|
|
Muscle / cartilage (cartilaginous portion of the Eustachean tube,
superior pharyngeal constrictor,
middle pharyngeal constrictor,
levator palatine)
|
Tumour
|
|
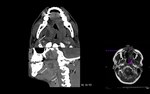
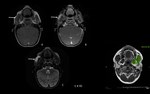
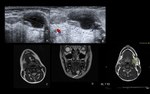
Peritonsillar abscess (Fig. 1)
Peritonsillar abscesses usually result from a bacterial infection and are uncommon in children with less than twelve years old.
Clinical presentation: drooling,
odynophagia,
fever and swelling.
US: hypoechoic to anechoic mass,
with a variable thick rim of solid tissue and adjacent reactive lymph nodes.
CT: low attenuation mass with rim enhancement.
|
2. Parapharyngeal space
Relations
- medial to the masticator space
- lateral to the pharyngeal mucosal space
- anterior to the prevertebral space
- posterior to the medial pterygoid
Contents and Pathology:
|
Contents
|
Pathology
|
|
Fat
|
|
|
Lymph nodes
|
Tumour
|
|
Nerves / vessels (small branches of the fifth cranial nerve,
internal maxillary artery,
ascending pharyngeal artery,
pterygoid venous plexus)
|
Tumour
|
|
Ectopic rests of minor salivary gland tissue
|
Tumour
|
|
|
Secondary extension – tumour,
infection
|
3. Parotid space
Relations:
- lateral to the parapharyngeal space
- medial to superficial space and subcutaneous tissue
- anterior to thecarotid space
- posterior to the masticator space
Contents and Pathology:
|
Content
|
Pathology
|
|
Parotid gland
|
Parotiditis,
abscess,
tumour
|
|
Intraparotid lymph nodes
|
Tumour (metastasis,
lymphoma)
|
|
Nerves / vessels (intraparotid facial nerve,
external carotid artery,
retromandibular vein)
|
Tumour
|
|
Embryologic remnants
|
First branchial cleft anomaly
|
|
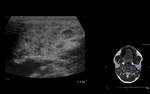
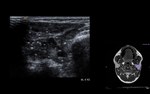
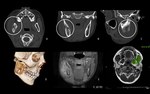
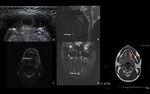
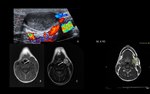
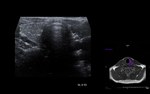
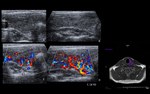
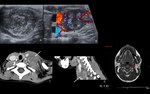
Acute and chronic parotiditis (Fig. 2 and Fig. 3)
The most common aetiology in children is viral.
A particular predilection for the salivary glands is shown by mumps virus and cytomegalovirus.
Clinical presentation: painful and enlarged gland.
US / Doppler:
Acute inflammation – enlarged,
inhomogeneous and hypoechoic gland,
that may contain multiple small,
oval,
hypoechoic areas and increased blood flow on Doppler.
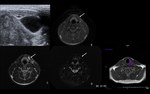
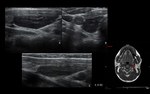
Chronic inflammation - smaller or normal sized,
hypoechoic and inhomogeneous gland,
and usually do not have increased blood flow on Doppler.
|
|
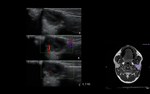
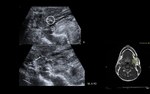
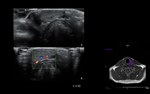
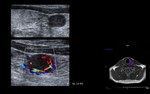
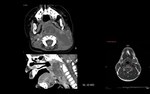
Tumour (Fig. 4)
Primary tumours of the salivary glands are uncommon in children.
However,
the proportion of malignant lesions compared to benign lesions is superior than in adults.
The most frequent malignant tumour of the parotid gland is mucoepidermoid carcinoma.
|
4. Masticator space
Relations:
- anteriorly: buccal space
- posterolaterally: parotid space
- medially: parapharyngeal space
Contents and Pathology:
|
Contents
|
Pathology
|
|
Muscles of mastication
|
Tumour (haemangioma),
benign masseteric hypertrophy
|
|
Ramus and body of mandible
|
Osteomyelitis,
abscess,
tumour
|
|
Nerves / vessels (mandibular division of the trigeminal nerve,
inferior alveolar nerve,
inferior alveolar artery and vein)
|
Tumour
|
|
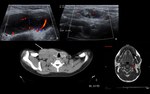
Haemangioma (Fig. 5)
Infantile haemangioma is the most common tumour of the head and neck in infancy,
and consists of a benign lesion,
with hamartomatous growth of capillaries at a high proliferation index.
Most haemangioma regress spontaneously.
Clinical presentation: compressible red-to-blue mass.
US / Doppler: heterogeneously echogenic or hypoechoic,
there may be small hypoechoic areas that demonstrate flow with colour Doppler,
usually with a high vessel density.
CT:
Proliferating haemangioma - lobulated solid tumor isodense with muscle,
with avid and rapid enhacement and rapid washout of contrast.
Involuting haemangioma - may contain foci of fat.
MR:
Proliferative hemangioma - lobulated mass isointense to muscle on T1- weighted MR imaging (T1WI) and moderately hyperintense with flow voids on T2-weighted MR imaging (T2WI),
with robust enhancement.
Involuting hemangioma - increased heterogeneity on both T1WI and T2WI,
fewer signs of fast-flow vascularity,
and variable enhancement.
|
|
Osteomyelitis (Fig. 6)
It consists of infection of both the bone and marrow of the mandible and is rare in healthy individuals due to early administration of antibiotics.
CT: Its radiographic appearance is variable,
including:
Acute suppurative - no imaging findings in the early stages
Chronic suppurative - various bone reactions,
including radiolucent and radiopaque areas
Esclerosing osteomyelitis – bone deposition along the osseous cortex and trabeculae.
|
5. Buccal space
It is located between the buccinator and platysma muscles,
therefore only a small potential space with limited contents.
Contents and Pathology:
|
Contents
|
Pathology
|
|
Parotid duct
|
Ductal obstruction
|
|
Minor salivary glands
|
Tumour
|
|
Nerves / vessels (buccal branch of facial nerve,
buccal nerve of the mandibular division of trigeminal nerve,
facial and buccal arteries and veins)
|
Tumour
|
|
Fat
|
|
6. Sublingual space
It is referred to as the floor of mouth,
corresponds to the space located below the tongue and confined by the mylohyoid muscle and hyoid bone.
Contents and Pathology:
|
Contents
|
Pathology
|
|
Sublingual gland and duct
|
Ranula,
tumour
|
|
Deep portion of submandibular gland and duct
|
Ductal obstruction,
tumour
|
|
Nerves / vessels (glossopharyngeal nerve,
hypoglossal nerve,
lingual nerve,
lingual artery and vein)
|
Tumour
|
|
Embryologic remnants
|
Lingual thyroid,
thyroglossal duct cyst,
dermoid / epidermoid cyst
|
|
Thyroglossal duct cyst (Fig. 7)
It can be located anywhere along the course of the thyroglossal duct from the base of the tongue to the thyroid gland.
At the level and above the hyoid bone it is usually located in the midline,
below the hyoid bone it can be paramedian.
Clinical presentation: painless,
enlarging neck mass or infection.
They typically move with tongue protrusion.
US: hypoechoic or anechoic lesion with a thin outer wall and increased through transmission.
CT: hypodense,
usually unilocular and occasionally septated,
well circumscribed and well defined lesion.
MR: homogeneously hyperintense on T2WI,
with variable signal intensity on T1WI,
depending on the protein content.
Rim enhancement may be seen following contrast administration.
|
7. Submandibular space
The submandibular space is located below the mandible,
inferior to the mylohyoid muscle and the inferior margin is the hyoid bone.
Contents and Pathology:
|
Contents
|
Pathology
|
|
Superficial portion of submandibular gland
|
Ductal obstruction,
tumour
|
|
Lymph nodes
|
Lymphoma
|
|
Nerves / vessels (hypoglossal nerve,
facial artery and vein)
|
Tumour
|
|
Embryologic remnants
|
Second branchial cleft cyst,
thyroglossal duct cyst,
dermoid / epidermoid cyst
|
|
|
Plunging ranula
|
|
Ductal obstruction (Fig. 8)
Salivary stones are most often located in the submandibular gland and may be multiple.
US: strongly hyperechoic lines or points with distal acoustic shadowing,
which represent stones.
In symptomatic cases with duct occlusion,
dilated excretory ducts are visible.
|
|
Plunging ranula (Fig. 9)
Ranulas are created by obstruction of the sublingual salivary glands.
They occur in the floor of the mouth and may protrude producing a ‘plunging’ appearance when involving the submandibular space.
Clinical presentation: generally painless,
slowly accumulating mass.
US: thin walled and hypoechoic mass.
CT: hypodense mass.
MR: hypointense on T1WI and hyperintense on T2WI.
|
|
Second branchial cyst (Fig. 10)
It may occur anywhere along the tract of the second branchial cleft tract from the palatine tonsil to the supraclavicular region.
Clinical presentation: typically fluctuant masses on palpation.
US: well delineated cystic structures appearing centrally hypoechoic,
with posterior acoustic enhancement.
CT: uniformly hypodense.
The “notch” or “beak” sign is considered pathognomonic,
and is characterized by a non-linear narrowing of the cyst between the internal and external carotid arteries.
MR: hyperintense on T2WI and variable appearance on T1WI,
depending on the protein content.
|
Infra-hyoid neck
1. Anterior cervical space
Relations:
- posterior: carotid space
- medial: visceral space
- superior: submandibular space
Contents and Pathology:
|
Contents
|
Pathology
|
|
Fat
|
|
|
Embryologic remnants
|
Second branchial cleft cysts
|
2. Posterior cervical space
Relations:
- superficial: sternocleidomastoid and trapezius muscles
- deep: prevertebral space
- anterior: carotid space
Contents and Pathology:
|
Contents
|
Pathology
|
|
Nerves (spinal accessory nerve (cranial nerve XI,
brachial plexus)
|
Tumours
|
|
Lymph nodes
|
Tumours,
infection
|
|
Fat
|
|
3. Visceral space
The visceral space extends from the hyoid bone to the superior mediastinum and is surrounded by the middle layers of the deep cervical fascia.
Contents and Pathology:
|
Contents
|
Pathology
|
|
Larynx
|
Tumour,
laryngocele
|
|
Hypopharynx / oesophagus
|
Tumour,
Zencker diverticulum
|
|
Trachea
|
Tumour
|
|
Thyroid
|
Thyroid hemiagenesis,
ectopic thyroid,
thyroiditis
|
|
Parathyroid
|
Adenoma,
hyperplasia
|
|
Nerves (recurrent laryngeal nerve)
|
Paralysis
|
|
Lymph nodes
|
Lymphoma,
metastasis,
infection
|
|
Embryologic remnants
|
Thyroglossal duct cyst,
third branchial cleft cysts
|
|
Thyroid hemiagenesis (Fig. 11)
Uncommon anatomic abnormality.
It is more frequent on the left side.
Clinical presentation: asymptomatic or thyroid dysfunction.
US: absence of hemithyroid,
with hypertrophy of contra-lateral hemithyroid.
|
|
Ectopic thyroid (Fig. 12)
Ectopic thyroid can occur anywhere along the initial path of descent of the thyroid,
most commonly occurring as lingual thyroid,
posterior to the foramen cecum at the base of the tongue.
US: homogeneously echogenic mass.
Additionally,
provides assessment for orthotopic thyroid tissue.
CT: typical high attenuation of thyroidal tissue.
|
|
Thyroiditis (Fig. 13)
Several inflammatory and auto-immune diseases can affect the thyroid gland.
Clinical presentation: Hashimoto thyroiditis (hypothyroidism) and Graves disease (hyperthyroidism).
US / Doppler: enlarged heterogeneous gland,
with thin hyperechoic linear bands,
that may simulate a multilobulated or multiseptated appearance.
Exuberant vascularization on Doppler.
|
|
Parathyroid hyperplasia (Fig. 14)
Parathyroid hyperplasia is the diffuse enlargement of the parathyroid gland.
It can be primary (sporadic or familiar) or secondary (renal failure).
Clinical presentation: most commonly an incidental finding in asymptomatic patient.
US: oval,
homogeneous,
solid,
hypoechoic mass.
|
Supra and infra-hyoid
1. Carotid space
Relations:
- anteriorly: masticator space; parapharyngeal space
- laterally: parotid space
- posteriorly: perivertebral space
Contents and Pathology:
|
Contents
|
Pathology
|
|
Deep cervical lymph node chain
|
Lymphoma,
metastasis,
infection
|
|
Nerves (sympathetic,
glossopharyngeal nerve,
vagus nerve,
accessory nerve,
hypoglossal nerve
|
Tumours
|
|
Vessels (Common and internal carotid artery,
internal jugular vein)
|
Aneurysm,
dissection,
thrombosis
|
|
Embryologic remnants
|
Second branchial cleft cysts,
ectopic thymus
|
|
Lymphoma (Fig. 16)
Lymphoma is the most common malignant tumour of the head and neck in children.
Non-Hodgkin’s and Hodgkin’s subtypes typically affecting younger and older children,
respectively.
US / Doppler: well delineated,
rounded lesion,
with reduced internal echogenicity,
altered vascularity and absent hilum.
CT: isodense to muscle.
MR: enlarged nodes are isointense to muscle on T1WI and hyperintense on T2WI with mild homogeneous enhancement.
|
|
Neuroblastoma (Fig. 17)
Neuroblastoma is a common tumour in children and when encountered within the neck generally represent metastatic disease.
Up to 5% of primary cases occur in the neck,
and this is particularly important as conveys a more favourable outcome compared with other primary sites.
Clinical presentation: neck swelling,
or can be a cause of Horner’s syndrome,
dysphagia or stridor.
They can also be secretory and have systemic symptoms.
US: elliptical or round hypoechoic solid masses posterior to the carotid sheath vessels,
with or without calcifications.
CT: calcifications and areas of haemorrhage or necrosis,
particularly in larger lesions.
MR: hypointense on T1WI and hyperintense on T2WI,
with areas of internal restricted diffusion.
|
|
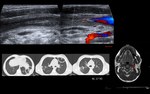
Lemierre’s syndrome (Fig. 18)
Lemierre’s syndrome is a rare and potentially lethal disease.
It results as a complication of an oropharyngeal infection spreading to the carotid space.
It is associated with septic thrombophlebitis of the internal jugular vein and distant septic emboli.
The lungs are the most common location of embolic dissemination.
Clinical presentation: sepsis characterized by fever and several days of sore throat after an apparently resolved pharyngitis.
US / Doppler: internal jugular vein thrombosis.
Contrast enhanced CT: may be useful to demonstrate the vein thrombosis and to study the extension of the embolic dissemination.
|
|
Ectopic thymus (Fig. 19)
Defective pathways of embryologic descent of thymic primordium can present with solid or cystic masses anywhere along the pathway of thymic descent from the angle of the mandible to the superior mediastinum.
Clinical presentation: usually asymptomatic.
US: echotexture similar to that of liver parenchyma.
MR: a slightly higher T1WI signal than muscle,
and a slightly less T2WI signal than fat.
|
2. Retropharyngeal space
Relations:
- anterior to the danger space
- posterior to the pharyngeal mucosal space
- anteromedial to the carotid space
- posteromedial to the parapharyngeal space
Contents and Pathology:
|
Contents
|
Pathology
|
|
Lymph nodes
|
Lymphoma,
metastasis,
infection
|
|
Fat
|
|
|
Retropharyngeal abscess (Fig. 20)
Retropharyngeal abscesses are seen in younger patients,
frequently those under six years of age.
|
3. Danger space
The danger space is a potential space located behind the true retropharyngeal space,
which connects the deep cervical spaces to the mediastinum.
4. Perivertebral space
This space is subdivided into two space by a deep slip of the deep cervical fascia to the transverse process: prevertebral portion,
anteriorly located and paraspinal portion,
posteriorly located.
Contents and Pathology:
|
Contents
|
Pathology
|
|
Cervical vertebral body and disc
|
Osteomyelitis,
tumour
|
|
Muscles (prevertebral,
scalene,
paraspinal)
|
Myositis,
tumour,
infection
|
|
Nerves (phrenic nerve,
brachial plexus)
|
Tumour
|
|
Vertebral artery and vein
|
Aneurysm,
dissection,
thrombosis
|
Multicompartimental
|
Neurofibromatosis (Fig. 22)
Plexiform neurofibromas are common in children with neurofibromatosis type 1.
They are manifested by multiple masses or fusiform enlargement of peripheral nerves,
usually involving a long segment of a major nerve trunk and multiple branches,
producing a bag-of-worms appearance.
US: may simulate a cyst,
with a well-defined hypoechoic mass distal acoustic enhancement or may show a target sign.
CT: slightly hypodense with respect to muscle.
MR: hypointense on T1WI and hyperintense on T2WI,
with contrast enhancement.
A characteristic target sign may be observed,
manifested by a central hypointense region and peripheral hyperintensity on T2WI.
|
|
Cystic hygroma (Fig. 23)
Lymphatic malformations are cystic masses composed of dysplastic endothelium-lined lymphatic channels filled with protein-rich fluid.
Clinical presentation: localized,
cystic,
solid or spongy mass or diffuse infiltration and enlargement of the affected region.
US:
Macrocystic – multi-loculated cystic mass
Microcystic – hyperechoic.
CT: hypodense mass.
MR: hyperintense on T2WI,
and variable signal intensity on T1WI,
depending on the protein content.
The cyst walls and septations enhance but not the fluid within the cystic spaces.
|