Diplopia,
or double vision,
is the hallmark of retinal disparity.
This phenomenon usually occurs when fusion is disturbed,
which is defined as the unification of visual excitations from the corresponding retinal images into a single visual percept.
A complete neuro-ophthalmological examination is essential for accurate localisation.
Because of a very high prevalence of structural,
infectious and inflammatory causes,
the patient’s age at presentation is an important consideration when working up for causes of binocular diplopia.
Younger adults and pediatric patients will need comprehensive evaluation,
which includes neuroimaging.
(I) Causes of diplopia
Monocular diplopia: Diplopia persists in the affected eye even when the other eye is closed,
due to local ocular causes.
[1,2]
Causes:
1] Refractive error
2] Corneal defects
3] Media opacities eg: cataract
4] Subluxated cataractous lens or intraocular lens
5] Iridodialysis
Binocular diplopia: Present when both eyes are open and disappears on closing one eye,
usually due to neuro ophthalmological relay failure.
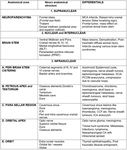
[1,2] [Table 1]
Causes:
1] Sudden onset palsies of third,
fourth or sixth cranial nerves
2] Sudden onset extraocular muscle restriction.
Eg: Thyroid ophthalmopathy,
muscle entrapment in fractures of the orbit,
mass impinging on the muscle
3] Dysfunction of neuromuscular junction: myasthenia.
4] Orbital disorders
5] Cranial nerve nuclei affected in brain stem injury
6] Supranuclear pathway injury
7] CNS demyelination eg: multiple sclerosis
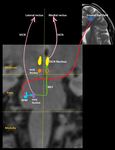
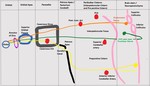
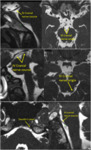
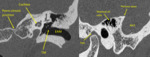
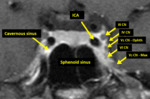
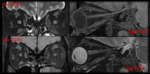
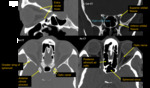
(II) Neuro ophthalmological relay pathway:
Refer Figure 1 - 7
(III) Clinical presentations and physical exam: [2,
3]
As with any clinical symptom,
diplopia requires a detailed evaluation in terms of history-taking and clinical tests.
(A) Salient points in history-taking:
-Is it uniocular or binocular?
-Does it increase in any particular gaze? – Vertical vs Horizontal vs Isolated
-Onset - acute or longstanding
-Duration
-Temporal course
-Associated with pain/headache
-Diurnal variation
-Associated with other neuromuscular abnormalities like proximal muscle weakness,
ptosis,
shortness of breath,
difficulty swallowing
-History of protrusion of the eye,
periorbital pain and swelling - orbital disease
-Associated neurological symptoms - vertigo,
paresis/paralysis of limbs (upper or lower)
-Past medical history - diabetes,
hypertension,
thyroid disease
-History of trauma/surgery
-Past history of strabismus or surgery for the same
(B) Physical exam:
A complete neuro-ophthalmological examination is essential for accurate etiological differentiation of diplopia:
(i) Visual acuity assessment
(ii) Slit lamp examination (will exclude any causes of monocular diplopia)
(iii) Fundus examination.
Presence of papilledema on fundus examination,
along with abduction deficit of either eye suggestive of lateral rectus will point toward the presence of raised intracranial tension,
the cause for which will need to be looked into.
Restriction of motility in any specific direction will invariably have an increase in the diplopia in that particular direction,
which can be assessed by doing a diplopia charting,
the reason for the impaired motility could be a restrictive process,
neuromuscular junction abnormality or impaired innervation to that particular muscle.
Ocular alignment can be assessed by doing the Hirschberg test [corneal light reflection test].
Orbital and lid abnormalities such as proptosis,
ptosis,
periorbital edema,
features of thyroid ophthalmopathy should be looked for.
Examination of pupillary reactions is vital as it may indicate optic neuropathy,
third nerve palsies [differentiating between vascular or compressive causes].
The presence of a relative afferent pupillary defect is points toward involvement of the optic nerve.
If history is suggestive of features of neuromuscular junction abnormalities such as myasthenia gravis,
specialised tests such as the fatigue test,
ice-pack test,
“Tensilon test” should be done to rule out or confirm the same.
Examination of the 3rd,
fourth and sixth cranial nerves is a must,
assessing extra ocular movements will reveal any external ophthalmoplegia,
indicative of oculomotor nerve,
abducens nerve or trochlear nerve involvement.
(i) 3rd nerve: A typical “down and out” position of the involved eye is seen in case of a 3rd nerve palsy.
Along with that,
the pupil may or may not be dilated and ptosis will be present.
(ii) 4th nerve: Palsy of the 4th nerve will cause difficulty in depression in adduction of the involved eye.
This will manifest as vertical diplopia,
which is exaggerated in downgaze.
The patient will typically complain of difficulty in going down the steps.
(iii) 6th nerve: As it supplies only the lateral rectus muscle,
the eye will be in an esotropic position with limitation of abduction.
Diplopia will be more in the side of the restricted muscle.
Proptosis,
chemosis,
periorbital edema,
conjunctival congestion are some of the specific signs of orbital disease.
The two most common orbital conditions that lead to extra ocular muscle involvement causing diplopia are thyroid eye disease and orbital pseudotumor.
Clinically,
thyroid eye disease can be unilateral or bilateral and is usually painless.
Orbital pseudotumor is generally unilateral and is has a sudden,
painful onset.
In cavernous sinus thrombosis,
superior orbital fissure syndrome,
Tolosa-Hunt syndrome of infiltrative,
inflammatory or compressive causes,
patient will have sudden onset severe headache,
binocular diplopia,
proptosis and painful extraocular movements.
Visual disturbance may be immediate,
in case of Tolosa-Hunt syndrome because of early involvement of the optic nerve,
or can occur at a later stage,
as in superior orbital fissure syndrome and cavernous sinus thrombosis.
The differential diagnosis of Mucormycosis should be kept in mind in patients with diabetes who present with painful ophthalmoplegia,
diplopia,
proptosis.