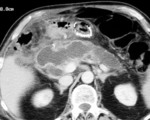
Pancreatitis refers to an inflammatory process of the pancreas.
There exists a spectrum of presentations of pancreatitis,
with each patient running a variable clinical course.
Pancreatitis can carry with it significant morbidity,
including a range vascular complications which can be life threatening.
Internationally,
the incidence of acute pancreatitis is increasing (1,2). Data suggest the range in incidence of acute pancreatitis across Europe is 4.6 – 100/100,000 population (3). The approach to the diagnosis and management of pancreatitis is multi-disciplinary,
with diagnostic and interventional radiology fundamental to both.
Early recognition of the associated vascular complications and an understanding of treatment options available is essential,
particularly to the radiologist in training.
Vascular complications are more commonly seen in the setting of chronic pancreatitis but are not infrequently seen in the acute setting.
In broad classification,
they can be considered as arterial or venous.
Arterial complications encompass direct erosion into a local artery,
pseudoaneurysm formation as well as local and distant ischemic sequelae.
Data suggest 5% of cases of pancreatitis are complicated by peri-pancreatic haemorrhage (4). Pseudoaneurysms can arise as a result of enzymatic digestion of the vessel well,
or,
when a visceral artery becomes incorporated into the wall of a pseudocyst (5). The splenic artery is most frequently associated with the formation of pseudoaneurysms in the setting of pancreatitis.
The gastroduodenal artery,
pancreaticoduodenal,
left gastric and hepatic arteries can all be affected,
in decreasing order of frequency (6).
Venous complications encompass thrombosis of the splanchnic venous system with or without associated varices.
Splanchnic thrombosis may be seen in up to 20% of acute pancreatitis patients (4). The splenic vein is most consistently cited as the most frequently affected,
with an incidence of just under 20% (4,7). Data from different case series are conflicting,
but in general it is thought that the portal vein is next most commonly affected with an incidence of 14%,
followed by the superior mesenteric vein (4,7). Significant haemorrhage can also ensue in the setting of venous thrombosis where gastric,
colonic or mesenteric varices develop.
The conventional modalities for the imaging and diagnosis of vascular complications arising in pancreatitis include (i) Ultrasound: Conventional and duplex (ii) CT (iii) Angiography: CT angiography,
DSA and catheter angiography.
Catheter angiography may be required for the diagnosis and management of some of the vascular complications arising in pancreatitis.
Conventional ultrasound may be useful in the detection of peri-pancreatic fluid collections.
These can be further characterised with the application of duplex USS,
which can identifty aneurysms.
A hypoechoic mass with turbulent blood flow is highly suggestive of a pseudoaneurysm.
Doppler ultrasound may identify splenic vein thrombosis.
CT has an important role to play in confirming the diagnosis of pancreatitis,
identifying possible aetiologies as well as identifying vascular (both arterial and venous) and other complications.
Prognosis can be guided using the Balthazar score (8).
The use of CT angiography can rapidly identify sources of haemorrhage in the setting of pancreatitis and can assist with planning definitive treatment.
Smaller pseudoaneurysms may occasionally be missed on CTA.
They may be more readily detected on DSA or on cathether angiography.
Catheter angiography may be used for therapeutic intervention through embolisation,
as well as being diagnostic.
Transcatheter arterial coil embolisation is an effective minimally invasive approach for the management of pseudoaneurysms and in the setting of haemorrhage.
An alternative to be considered where a pseudoaneurysm cannot be traversed are liquid embolic agents (5). Although catheter-directed thrombolysis may be considered for patients with splanchnic thrombosis due to pancreatitis (9), this treatment is rare owing to alternatives including therapeutic anti-coagulation.
Furthermore,
spontaneous recanalisation is reported in pancreatitis (7). Data also suggest that splanchnic thrombosis tends to run a benign course in the setting of patients with pancreatitis (10).