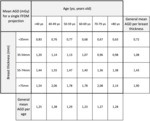
Based on dose data retrieved from our archive,
we created a table displaying the AGD in a single FFDM projection varying with age and breast thickness; in this table,
we included a general dose value for each age and thickness range (tab.
1).
As shown in table 1,
AGD increases with breast thickness and decreases with age.
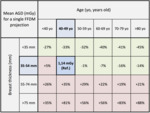
In order to help communication between clinicians/radiologists and patients,
we transformed the absolute dose results (mGy) in dose percentage variations (tab.
2).
We found the modal values of age and breast thickness to identify the reference,
assessed in the 40-49 age range and in the 35-54 mm breast thickness range (tab.
2).
Table 2 can therefore be a valid support to explain to patients the dose radiation risks concerning the exams proposed.
As known,
in FFDM the main issue is the overlap of mammary tissues,
especially in dense breasts.
Women with dense breast could benefit from other imaging techniques such as DBT and CEM,
which permit to obtain a better lesion detection [1,
2].
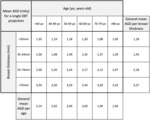
As done for FFDM,
we obtained a similar table for DBT showing the modification of AGD values in a single projection across different age and breast thickness ranges (tab.
3).
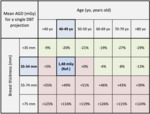
Also in this case,
the transformation of the absolute values of AGD in dose percentage variation is functional to improve patient comprehension about DBT risks (tab.
4).
The modal values of age and breast thickness in DBT were the same found in FFDM.
In table 4 the percentage variability of radiation dose in DBT is shown: similarly to FFDM,
the radiation dose increases with breast thickness and decreases with age.
Resulting from a literature review,
the new approach of Contrast Enhanced Mammography introduces at least two adjunctive risk factors for women.
First,
this procedure requires additional acquisitions increasing the administered radiation dose.
We created an easy-to-read table for improving women awareness about the procedure they are proposed to undergo (tab.
5) [3].
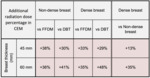
As shown in table 5,
in comparison with FFDM and DBT the global exam dose (expressed as percentage increase of AGD) in non-dense and dense breast phantoms and in different breast thickness are:
- non-dense phantom at 4.5 cm + 37.5% vs.
FFDM and + 30% vs.
DBT;
- non-dense phantom at 6 cm + 36.2% vs.
FFDM and + 41% vs.
DBT;
- dense phantom at 4.5 cm + 33.3% vs.
FFDM and + 28.8% vs.
DBT;
- dense phantom at 6 cm + 35.4% vs.
FFDM and + 48.0% vs.
DBT.
Finally,
dense phantoms receive 12.5% and 35% additional radiation dose at 4.5 cm and 6 cm,
respectively (tab.
5) [3].
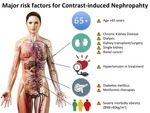
From a recent comprehensive review of literature about contrast media and contrast-induced nephropathy emerges that the major risk is related to pre-existing severe chronic renal insufficiency.
Other renal diseases could increase the risk of CIN,
including dialysis,
kidney transplant,
single kidney,
renal cancer and renal surgery [4-6].
With the increasing prevalence of obesity,
BMI has become a new index that has to be considered in renal diseases.
New mechanisms of renal damage have been discovered as associated with metabolic disease and this could have an important role in the development and progression of chronic kidney disease,
directly or indirectly,
through hypertension and diabetes,
generally related to morbidly obesity (BMI>40/m2) [7].
Another risk factors of CIN is age >65 years [4].
In addition to history of renal disease and age,
other CIN risk factors are:
- hypertension in treatment;
- diabetes mellitus;
- metformin therapies.
In figure 1 the main risk factors that have to be considered as increasing risk of CIN are represented in an iconographic way in order to facilitate communication [4,
6].