RLQ is examined with ultrasound at first.
When signs of appendicitis or other peculiar features can’t be found,
CT scan with administration of contrast media,
is performed.
For its high spatial and contrast resolution,
multidetector CT is the best non-invasive technique for exploring RLQ and the whole abdomen in few seconds.
CT is the most accurate imaging modality in the diagnosis of acute appendicitis,
but also a helpful tool for the differential diagnosis of the many uncommon causes of RLQ pain.
Crohn Disease
Crohn disease (CD) is an idiopathic intestinal inflammatory condition.
The highest annual incidence of CD in Europe is estimated to be around 12.7 per 100,000 person-years and the peak age of incidence is between 16 and 30 years.
While involvement of any segment of the gastrointestinal tract is possible,
typically the distal ileum is affected,
making direct endoscopic evaluation and biopsy difficult.
It remains a challenging entity to diagnose clinically,
especially with an acute onset.
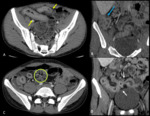
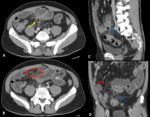
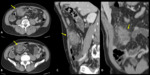
CT features of active inflammatory Crohn disease are:
- mural hyperenhancement and stratification with bowel wall thickening (> 3mm)
- involvement of one or more intestinal tracts,
especially the distal ileum
- transmural inflammatory process with perenteric fat stranding and in a later stage,
fistulas and strictures
- engorgement of the vasa recta (“comb sign”)
- reactive lymphadenopathy in the mesentery adjacent to the affected bowel segments.
Young age,
history of abdominal pain with diarrhea and two or more intestinal tracts affected make the diagnosis of Crohn disease more likely (Fig. 1).
Infectious enterocolitis
Infectious enterocolitis can affect the ileo-cecal region in particular when caused by pathogens like Yersinia enterocolitica,
Campylobacter jejuni and Salmonella enteritidis.
In patients with compromised clinical status and history of chemiotheraphy a CT scan can be perform to assess intestinal changes.
Like other “colitis”,
imaging findings are not specific.
CT images show:
- mural thickening of the bowel wall
- hyperenhancement or homogeneous enhancement
- lymphadenopathies,
fat stranding and fluid
Segmental involvement (10-30 cm) and patient's history are the best clues for the diagnosis of colitis.
Malignancies
Acute RLQ pain can be the initial presentation of a ileo-cecal neoplasm.
It occurs more commonly in older patients with anemia,
weight loss,
pain and palpable mass.
95% of these tumors are adenocarcinomas,
but also lymphoma can be diagnosed.
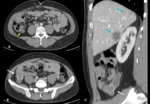
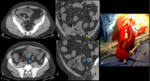
CT images show:
- focal thickening of the bowel wall (usually < 5 cm)
- irregular margins,
loss of the mural stratification,
irregular enhancement
- fat stranding and lymphadenopathy make malignancy more likely.
Although rare,
also appendix neoplasms must be considered in the differential diagnosis of RLQ pain (Fig. 2).
Right colon acute diverticulitis
Like the most common left sided diverticulitis,
this condition occurs in older patients,
with no peculiar clinical features.
The incidence of right colon diverticulosis has been estimated to be approximately 8.5% in western countries.
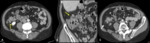
CT images of right colon acute diverticulitis show:
- focal thickening of the colonic wall adjacent to a diverticula
- fluid,
inflammation or abscess in the mesocolon
- diverticula can also perforate and free air can be detectable
RLQ pain in older patients with segmental involvement and the presence of other diverticula can suggest the diagnosis (Fig. 3).
Small bowel diverticulitis (SBD)
Diverticula of the small bowel are rare out-pouchings of the bowel wall.
SBD is far less common than the colonic one,
because their larger dimensions and fluid content,
make them less prone to complications.
It is typical of younger patients,
in whom is mandatory to exclude acute appendicitis at first.
Prevalence of SBD is unknown.
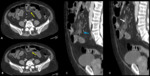
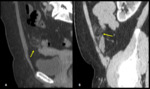
CT images show:
- abnormal distension of these outpouchings filled with fluid and/or air
- fat stranding of the surrounding mesentery
- they can also perforate,
or can cause intestinal obstruction
The diagnosis of acute diverticulitis is often difficult.
In case of small bowel obstruction the inflamed area corresponds to the site of the stop (Fig. 4; Fig. 5).
Meckel’s diverticulitis
Meckel diverticulum (MD) is the most common congenital anomaly of the gastrointestinal tract.
It is located on the antimesenteric border,
approximately 100 cm from the ileo-cecal valve,
whereas other small bowel diverticula are located on the mesenteric border.
More commonly it affects childrens,
but complications can occur also in adults.
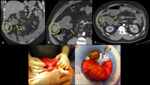
Acute complications include gastrointestinal bleeding from ectopic gastric mucosa,
intestinal obstruction,
perforation,
inflammation and torsion (Fig. 6).
Inflammation can be caused by the presence of a entherolith or a foreign body inside the diverticulum (Fig. 7).
The diagnosis is often challenging but the “rules of 2” can help:
- Meckel’s diverticulitis occurs in about 2% of the population
- usually is 2 inches long
- located within 2 feet of the ileo-cecal valve
- can affect children <2 years old
Epiploic appendagitis
Epiploic appendagitis is a rare and self-limited condition due to torsion of the vascular stalk with subsequent ischaemia of the appendage.
On CT images it appears as:
- oval shaped fatty lesion
- less of 5 cm in diameter
- located anteriorly to the colonic wall
- it is visible only when surrounded by fluid,
due to inflammatory changes of the adjacent omentum
- the typical appearance is a small fatty lesion with an hyperattenuating rim
Sometimes it can be difficult differenciate between epiploic appendagitis and omental infarction: the size of the lesion (<5 cm) is a helpful tool (Fig. 8).
Omental infarction/abscess
Omental infarction and abscess are rare entities,
typically simulating acute appendicitis for their location in RLQ and involvement of the pediatric population.
Omental infarction is related to trauma or thrombosis of the omental veins.
An infectious process can overlap causing an abscess with air-fluid level and inflammatory changes of the surrounding fat tissue.
On CT images it is characterized by:
- solitary inhomogeneous enhancing mass
- usually larger than 5 cm
- located anteriorly to the bowel loops with a air-fluid level
Unlike epiploic appendagitis,
omental abscess lacks the hyperattenuating rim and unlike diverticulitis is not associated with bowel wall thickening (Fig. 9).