Breast cancer is the second leading cause of cancer death in women,
exceeded only by lung cancer. Evaluation of tumor biologic features represents an evolving area of great interest in treatment and is becoming increasingly important.
However, the short term survival rate is largely dependent on the disease stage.
The role of imaging in breast cancer staging has evolved rapidly over the past few years,
and radiologic findings are now incorporated into clinical staging.
Anatomy
The internal mammary lymph nodes (IMLN),
also known as internal thoracic lymph nodes and parasternal nodes, are situated in the parasternal region, adjacent to the internal mammary vessels in the first through fifth intercostal spaces.
It represents a primary lymphatic pathway in the breast,
accounting for up to 25% of its lymphatic drainage,
predominantly from deep and medial structures,
retromammary lymphatics,
anterior chest wall,
and structures of the upper anterior abdomen. Fig. 1 Fig. 2
Efferent lymphatics drain into the venous system via the right lymphatic duct, thoracic duct,
and inferior deep cervical nodes.
Pathological IMLN in patients with breast cancer
There are several factors that increase the possibility of metastases in this territory: age less than 35 years,
medial location and nonpalpable tumor,
the presence of involved axillary lymph nodes,
higher tumor grade,
lymphovascular invasion and triple-negative hormone receptor status.
Concurrent internal mammary lymph node and axillary node metastasis has proven to be an indicator of poor prognosis in terms of overall survival when compared with involvement of only one of the nodal basins. Fig. 3
The study of this lymphatic pathway has its handicaps,
due to the morbidity associated to the approach of enlarged IMLNs,
that requires advanced surgical experience.
Besides,
the treatment of breast carcinoma that has apparently spread to the internal mammary lymph nodes is controversial.
It is important to identify the presence of internal mammary nodal metastases,
which not only changes the nodal stage and prognosis of the patient but also affects the planning of radiation therapy,
requiring a wider irradiation field.
Imaging modalities
US
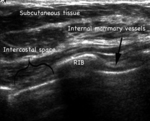
Parasternal US scanning may be useful and costeffective to stage this nodal basin,
allowing an excellent view of the intercostal spaces. Normal nodes are not easily seen in the intercostal spaces,
so if there is any visible node it should be considered suspicious. Fig. 4
Normal IMLNs usually measure less than 5 mm in the long axis but even nodes as large as 9 mm can be nonpathologic.
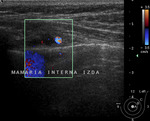
Suspicious IMLN would appear hypoechoic,
enlarged, with rounded morphology,
diminished to absent fatty hilum, thickened or eccentrically bulged cortex and hyperemic. Fig. 5
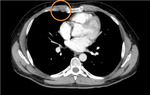
CT
Pathological IMLNs on CT will appear as enhancing soft-tissue masses in the intercostal spaces adjacent to the IT vessels. Fig. 6
PET/CT
Detection of IM lymphadenopathy on PET/CT scans is more sensitive than with CT alone.
IMLN metastases on PET/CT images manifest as fluorodeoxyglucose (FDG)–avid soft-tissue adenopathies in the parasternal region,
with SUVs greater than that of mediastinal blood pool or the adjacent pectoral muscle. Fig. 7
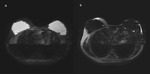
MRI
When using imaging modalities with a higher resolution than US,
one cannot presume that because a node is visible that it is suspicious.
Physiologic IMLNs were most frequently seen in the second and third intercostal spaces and were more often on the left.
It should be considered especially the morphology and size of the IMLN.
Enhancement and hyperintensity on STIR images can be pathologic but,
unfortunately,
imaging metastatic and non-metastatic features frequently overlap. Careful imaging follow-up or tissue sampling may be warranted. Fig. 8
Differential diagnosis of IMLNs includes breast cancer or second primary nodal metastases,
infection/nonspecific inflammation and granulomatous silicone lymphadenitis.
Siliconoma:
When an extracapsular prosthetic rupture occurs in patients with breast silicon prosthesis,
this material may deposit in the surrounding tissues and migrate to ganglionar chains,
forming a granulomatous reaction that is called ‘siliconoma’.
It shows some specific sonographic and MRI imaging features that could help with the differential diagnosis with other benign and malignant entities.
The typical sonographic features are an echogenic pattern of scattered and reverberating echoes with a well-defined anterior margin and loss of detail posteriorly,
showing a “snowstorm” appearance. Fig. 9
MRI can be a useful way to confirm this findings, especially in women with breast cancer that shows suspicious IMLN,
that would lead to an upgrading staging and different treatment if considered pathological.
Using T2-weighted and silicon selective suppressed sequences,
we could confirm this diagnosis.
Siliconomas in the IMLN will be hyperintense in T2,
less than water-like substances,
hyperintense in STIR and hypointense in Silicon-suppressed sequences,
while pathological IMLN will persist with high signal intensity. Fig. 10