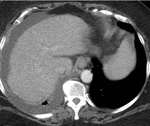
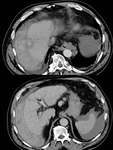
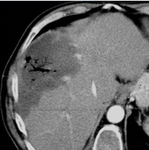
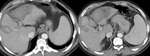
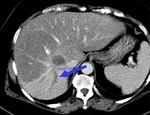
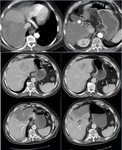
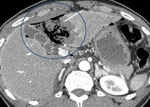
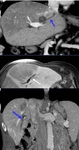
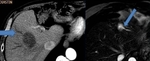
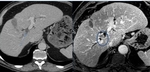
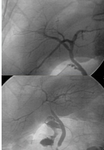
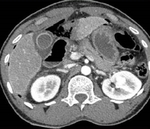
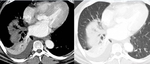
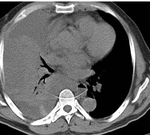
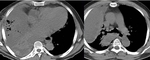
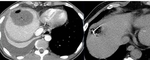
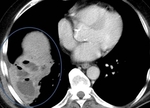
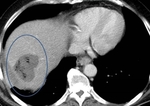
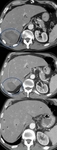
Liver Ablation
The liver has been the most common target organ for ablative percutaneous treatment of both primary and secondary neoplasms.
The ablation of hepatic lesions from the beginning has been considered very safe with very low mortality rates and major complications; oscillating generally from 0.7 to 1.4%.
Some recent series says a slightly higher mortality rates of up to 2% (Wong et.
al.).
Causes of death includes bowel perforation,
portal vein thrombosis,
hepatic failure,
septic shock from peritonitis and massive hepatic hemorrhage or hepatic infarct.
The main complications have always been low with rates of up to 5.7%.
A large multicenter study by Livraghi et.
al.
in which 3,554 injuries were treated and reported 50 major complications with a rate of 2.2%.
In this study,
a greater number of ablation sessions were associated with a higher rates of complications.
Another large study by Rahim and colleagues cite a similar major complication rate of 2.4%.
A more recent study reports a slightly lower rate of major complications,
1.9% for treatment,
and 1.8% per session.
These more recent figures are not statistically significant from the above data,
they may indicate a downward trend of major complications as the operator's competence increases and as RF techniques are refined.
This hypothesis has been previously supported by Poon et.
al.,
who report a decrease in the rate of complications and a higher rate of complete ablation as a result of accumulated experience with hepatic RF.
Although these reported rates on literature are very low and acceptable,
the feeling that we professionals have about it,
is not that.
Since the implementation of RF as a minimally invasive method and its widespread use in many centers and especially since the introduction of the microwave as thermal therapy that allows us to perform ablations of greater volume,
the rate of complications has increased significantly,
an increase that confirms the daily clinical experience but not the literature.
We analyze which are the causes of this potential increase in complications.
When the use of these ablative techniques is generalized,
we are undoubtedly experiencing a learning curve for many professionals who have been using these techniques in recent years.
The relaxation on behalf of the radiologists and hospitals committees in outlining the indications strictly means that we are treating patients on borderline clinical situations with questionable indication.
The appearance of new "more aggressive" ablative techniques such as the microwave that allows us to treat larger volumes lesions makes treatments a challenge for the radiologist,
to try to treat "something else" sometimes without adequately considering the involved risk.
The generalization of these techniques means that there is no record of what is done,
neither in terms of results nor in terms of complications.
There is no general registry of complications and very few professionals publish their experience.
We stick to what literature tells us,
which is undoubtedly biased.
There are many procedures,
in many whose results,
good or bad are not recorded.
That is why the figures reported in the literature,
undoubtedly real for those who publish them and optimists do not correspond fully with reality.
Vascular Complications
Hemorrhage
Hemorrhage is the main and most common vascular complication in the hepatic RF.
The overall risk of bleeding is low (<2%),
and is influenced by both the location of the tumor and the underlying liver parenchyma.
An increased risk of hemorrhage is associated with cirrhosis due the coagulopathy,
and hepatocellular carcinoma (HCC) due to its inherent risk of bleeding for the hypervascularity.
When it occurs,
it is usually intraperitoneal,
but it can be subcapsular,
intralesional,
or into the pleural space.
Obviating the risk of increased bleeding in coagulopathies,
the risk is greater in case of subcapsular access without underlying parenchyma that "protect",
lesions that require a tangential incidence respect to the liver capsule,
increasing the risk of capsular laceration and,
above all,
lesions that require the insertion of several needles,
or frequent repositioning,
Treatment of severe bleeding after the procedure includes coagulation transfusion (with sufficient frequency to control bleeding),
arterial embolization,
pleural drainage or surgery.
How to decrease the hemorrhagic complications?
Minimum requirements prior to the procedure,
with prothrombin time values of at least 50 and at least 70,000 platelets.
Confirm that the patient has suspended the anticoagulant therapy before the procedure.
Ensure safe access,
protecting the access with healthy parenchyma in case hypervascular lesions are treated or treating directly the lesion if it is very fibrous.
Avoid tangential access to the capsule.
Perform a slow needle withdrawal once the procedure is finished,
coagulating the path.
Other Vascular Complications
They include portal venous thrombosis,
hepatic venous thrombosis,
hepatic infarction,
arteriovenous fistula,
and pseudoaneurysm.
Portal Thrombosis
Most of the studies report portal thrombosis (De Baere 1.7%).
It has been proven that there is only potential repercussion and a special management is required if the thrombus affects the main portal trunk.
The incidence of portal thrombosis has increased with the use of microwaves.
The great hepatic vessels were protected from the potential thrombosis by the refrigerant effect of the flow in the vessel.
With the microwave,
this protection disappears.
The risk of portal thrombosis is also increased significantly in cases of open ablations,
where Pringle procedures is performed.
How to avoid portal thrombosis?
Avoiding portal branches during the procedure.
Using low power source,
and perform the RF more time,
to have perfect control overf the treated area.
Use mixed treatments embolization,
RF and alcohol to not perform an early ablation,
decreasing the risk of vascular damage.
Liver Infarct
A very infrequent complication using RF treatments,
although is more and more frequent with MW.
Its rarity will undoubtedly be due to the dual contribution of blood to the liver parenchyma (portal and artery).
Most of the infarcts that occur affect segments or subsegments,
in these cases the treatment is conservative with good evolution in general,
although the tissue usually solves without incidence,
the infarcted area tends to favor the appearance of biliomas,
abscesses and portal thrombosis.
When the infarction is lobar,
the situation can be serious due to the liver failure.
The risk of secondary mortality is high in these cases.
Avoiding liver infarcts
Especially using MW treatments.
Ensure the position of the needle and calculate the area included in the advance of the treated area to avoid vascular branches being located in it.
Perform ablations at low power and increase it in function of the treated volume and the potential damage of visible structures.
Avoid as much as possible to reach vascular structures in the treated area.
BILIARY COMPLICATIONS
These arise from direct penetration or thermal injury of the biliary tract.
Are relatively frequent,
and stands out the hepatic abscess,
which has been well documented,
and it has the highest incidence (De Baere up to 2%).
The risk is higher in diabetics and especially in patients on whom there has been a previous manipulation on the biliary tract (resections,
previous ERCP,
biliary derivations,
where the biliary ducts is already colonized),
that can end up in sepsis.
How can we improve?
Some authors advocate antibiotic coverage always.
Others limit it to patients at risk,
diabetes,
and previous surgical history of gallbladder,
biliary tract or liver manipulation.
Avoid as much as possible the damage of the tract or at least the main.
Once the abscess is diagnosed,
consider urgent percutaneous drainage.
Bilomas
The formation of bilomas has been reported in almost all the relevant case series,
with rates of up to 1.5% (Choi et.
al.).
Although the biloma,
if it is not large,
is not a major complication.
It can be complicate it with severe pain,
infection or significant increase in volume that requires drainage.
Other frequent complications are biliary stenosis,
hemobilia,
biliary peritonitis,
acute cholecystitis and biliary fistulas (biliary-enteric,
cutaneous or bronchial) that are less frequent.
How to improve?
Basically,
a correct technique,
with a right needle position controlling the volume.
Early drainage.
EXTRAHEPATIC COMPLICATIONS
The extrahepatic complications of the hepatic RF are extensive,
and include direct penetration and thermal injury in adjacent organs,
tumor seeding,
as well as thermal effects on remote organs.
Injury On Neighbor Organs
When the hepatic lesion,
located at subcapsular level,
is in proximity or contact in neighboring organs (vesicle,
right colon,
stomach,
kidney,
adrenal,
and diaphragm) there is a real risk of thermal injury of these organs.
This complication,
although rare,
has been reported consistently in all series.
The gallbladder is the most susceptible structure to damage.
Thermal cholecystitis has been reported but usually have no consequences although they can lead to biliary peritonitis.
Gallbladder damage can be avoided by making retrograde ablations,
that is,
by placing the tip of the needle so that the RF or MW energy in its advance does not affect the gallbladder and also performing mixed treatments.
The stomach is another structure that can be damaged by treating lesions in the LHL.
The gastric wall is usually thick,
but gastric lesions has been reported,
they are usually limited to edematous thickening of the wall that is self-limited with symptomatic treatment.
The right colon in the most dangerous organ,
since its thin wall,
and perforation is usually complicated with peritonitis or abscess.
To avoid the injury of peritoneal or even retroperitoneal structures,
the possibility of instilling serum or CO2 into the peritoneum is successfully reported to create a barrier that protects neighbor visceras.
Pneumothorax and Pleural effusion
Pneumothorax and pleural effusion that requires drainage has been reported in the majority of series.
A slightly number of cases has been reported performing an open RF in comparison with percutaneous (2.1% and 1.3% respectively).
Also a less cases using low power with progressive ablation.
Pneumothorax has been reported when treating lesions subdiaphragmatic,
particularly when using thoracic access.
Exquisite technique.
Well control of the tip of the needle when performing copula lesions.
Early and immediate drainage once detected.
TUMORAL SOWING
Tumor sowing along the pathway usually manifests between 3 and 12 months after RF and carries a very low risk,
(from 0.3 to 4%).
Multiple multicentric studies minimize the risk of seeding in the needle pathway.
It usually manifests as nodular lesions at the perihepatic level in a location adjacent to the point of insertion of the needle.
The behavior of the lesions may be similar to the hepatoma.
Immediate resection should be considered after detection.
This complication was a controversial issue for years,
which even led to question the safety of ablative procedures.
There is a greater risk of tumor seeding in subcapsular lesions,
in poorly differentiated lesions,
when there has been previous percutaneous biopsy.
When a single puncture is not made,
but several attempts are made in the placement of the needle,
also the risk increases when the subcapsular lesions are approach directly,
without interposing healthy parenchyma in the puncture.
How can we improve?
Avoiding as much as possible the circumstances that promotes dissemination.
Avoiding treating subcapsular lesions,
at least avoiding a direct approach,
instead of the shortest path,
we must access via a path that allows us to interpose healthy parenchyma between the lesion and the access point to the liver.
Try to perform clean,
direct punctures,
give a single attempt,
without repositioning the needle once punctured.
We must do treatment in the outflow tract.
The previous biopsy of lesions,
especially subcapsular ones,
should be avoided.
It is very difficult to determine if the tumor seeding occurs during the ablative procedure or during previous biopsy.
LOCAL RF BURNS
Thermal energy not only interacts locally where it can cause complications,
it can also cause remote damage due to heating effects.
The area where these effects occur most frequently is the skin,
where the electrodes are placed that will close the RF circuit.
Normally burns do not occur.
The ground connections are designed with a large surface so that the transmitted energy is dispersed.
Sometimes,
the pads are not placed well or during the procedure they partially detach,
decreasing significantly the dispersion surface,
with which the energy is concentrated on a smaller surface.
In the case of microwaves,
burns can occur in the abdominal wall,
in very small lesions,
and subcapsular localization when ablation is performed in long periods or in unconscious displacement of the needle to the surface during the procedure as a consequence of a deep breathing of the patient.
How can we avoid it?
Correct placement of the ablation pads.
If you use more than one needle simultaneously or use two dispersion pads.
Use cooling devices such bags of cold serum to be applied on the skin.
Be jealous in monitoring the needle.
Normally the needles are calibrated.
We must confirm that the marks do not move during the process once the needle is placed.
TUMORAL EXPLOSION
It is a controversial point on recent years,
and we decided to emphasize it at the end.
HCC is a tumor with a variable behavior,
although in many cases it is quite well differentiated tumors,
of progression,
at least during the first years,
slowly.
There have been cases of patients with HCC,
treated,
with immediate complete response,
and without signs of recurrence,
at least in the initial controls,
and that without apparent cause,
in the follow-up,
show a massive,
multifocal tumor explosion,
many times with epicenter in the treated lesion,
but however,
at a local level,
it still shows no signs of tumor recurrence.
Several theories suggest that tumor growth factors are released during the procedure that facilitate aggressive,
multifocal recurrence that is totally atypical for hepatocellular carcinoma.
This behavior has not been reported in patients treated with embolization or with cryoablation,
which is why it is directly related to thermal treatments.
How can it be avoided?
The ignorance of the cause of this treatment makes it difficult to prevent it,
is postulated by "more secure" treatment using low energies at the beginning of treatment with a progressive increase of the power at the end to achieve a high safety margin.
It is a topic on which we must focus and there is no doubt that in the future we will find answers.