Case 1
A 25 year old male presented to the emergency department with a stab wound to left flank.
The patient was haemodynamically stable however,
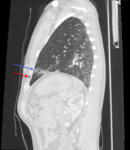
no details regarding weapon type or size or the suspected depth of the wound was provided by the attending clinical team (Fig. 1).
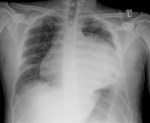
Admission CXR demonstrates a fractured 9th rib on the left side,
at the wound site (Fig. 2) suggesting a significant penetrating injury.
A CT thorax,
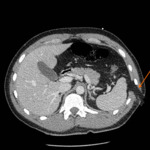
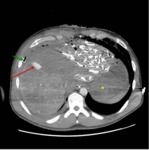
abdomen and pelvis was performed which demonstrates a left sided entry wound with a defect in the overlying skin and the underlying muscles of the lateral chest wall and herniation of intra abdominal fat through the defect (Fig. 3, Fig. 4).
In addition,
there is a left sided haemopneumothorax (Fig. 4, Fig. 5) and a diaphragmatic defect with herniation of a small knuckle of the gastric fundus through the defect (Fig. 6, Fig. 7).
Key learning point: The immediate imaging in this case highlights the importance of image reconstruction and illustrates that the extent of internal injury may often be underestimated.
It is therefore vital for the reading radiologist to attempt to predict the trajectory of the injury (Fig. 8) in order to identify potential injury sites related to the path of the wound.
The diaphragmatic injury was treated conservatively at this stage and a wide bore chest drain was inserted into the hydropneumothorax; the patient was then transferred to the intensive care unit for supportive care.
48 hours after injury a CXR demonstrated a large gas filled structure in the lower zone of the left hemithorax which was concerning for progression of the traumatic diaphragmatic hernia (Fig. 9).
A subsequent CT confirmed progressive herniation of the stomach through the diaphragmatic defect into the left hemithorax with complete collapse of the underlying lung (Fig. 10,
Fig. 11).
The patient underwent surgical repair and splenectomy.
3 days post repair ultrasound and CT demonstrated a complex left sided pleural effusion in keeping with an empyema (Fig. 12, Fig. 13).
This was drained percutaneously and treated with antibiotics.
15 days post surgical repair the patient deteriorated acutely and was in respiratory distress following removal of the chest drain.
The CXR demonstrates gross enlargement of the cardiac contour (Fig. 14) and an urgent CT was then performed.
The CT demonstrates a small persistent left sided empyema and a large pericardial effusion (Fig. 15).
Pericardiocentesis was performed which drained serosanguinous fluid.
The patient made a good recovery and following an extended inpatient stay was eventually discharged home.
The patient was reviewed periodically in outpatient clinic and 11 months post injury a CT was performed,
this demonstrates a recurrence of the diaphragmatic hernia complicated by a fistula between the herniated gastric fundus and a chronic left sided empyema (Fig. 16).
The patient unfortunately refused to attend follow up appointments and has subsequently been lost to follow up.
Diaphragmatic injuries following penetrating trauma from stab wounds are uncommon.
These types of diaphragmatic defects are usually small and therefore diagnostically challenging5.
Signs of traumatic diaphragmatic injury on CT include:
- Discontinuity of the diaphragmatic contour
- The "collar" sign - waist-like constriction of a hollow viscus

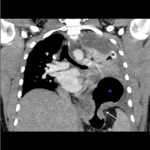
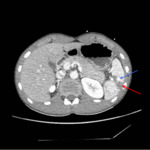
Fig. 10: Case 1: Coronal CT image demonstrating the diaphragmatic defect (white arrow) with progression of the diaphragmatic hernia, now containing most of the stomach (blue asterisk). The waist-like constriction of the stomach is also known as the "collar sign".
- Herniation of abdominal contents3
Key learning point: The presence of a haemothorax in the context of penetrating abdominal injury should prompt careful evaluation of the diaphragmatic contour on imaging. Herniation of abdominal contents are usually delayed and may present days to months after injury4.
Case 2
A 47 year old male presented following a knife stab wound to left side of the chest / upper abdomen.
Admission CT demonstrates a single skin entry point with multiple blebs of gas tracking laterally within the subcutaneous tissues of the lateral chest wall (Fig. 17, Fig. 18).
There is a small left sided pneumothorax as well as a small bleb of gas within the pericardial fat (Fig. 19).
In addition,
multiple small traumatic pneumatocoeles are seen within the underlying lung forming a linear orientation along the trajectory of the knife track and extending up to the adjacent hemidiaphragm (Fig. 19,
Fig. 20,
Fig. 21).
The hemidiaphragm itself is intact.
The patient was treated conservatively and made a full recovery.
Key learning point: The entry point may not exactly correspond to the trajectory of internal injury due to the movement of structures.
As illustrated in this case, the entry point is a few centimeters inferior to the trajectory of the lung injury.

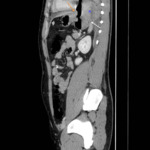
Fig. 21: Case 2: Sagittal CT image demonstrating multiple small pneumatocoeles in the linear orientation along the trajectory of the penetrating injury (blue arrow). This image highlights that the entry point (red arrow) may not exactly correspond to the trajectory of internal injury (blue arrow) due to the movement of structures.
Case 3
A 47 year old male presented to the emergency department following a stab injury to the left side of the abdomen.
He was complaining of severe abdominal pain and abdominal examination revealed guarding and generalised tenderness.
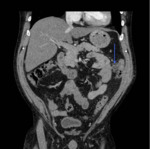
A CT abdomen and pelvis performed on admission demonstrates a single entry point (Fig. 22) with a defect in the lateral abdominal wall musculature deep to the entry wound.
The descending colon abutting the abdominal wall defect is thickened with surrounding inflammatory changes and there are small blebs of free intraperitoneal gas remote to the site of injury,
consistent with bowel wall injury (Fig. 23,
Fig. 24).
The patient was taken to theatre as an emergency and a defunctioning ileostomy was performed.
The patient made a full recovery following a short post-operative inpatient stay.
Key learning point: Free intraperitoneal gas can be introduced from a penetrating wound, therefore the presence of intraperitoneal gas is not a reliable sign for hollow visceral injury in the context of penetrating stab injuries.
However,
the presence of gas remote to the trajectory of the injury should promote careful evaluation for secondary signs of bowel injury1:
- Bowel wall thickening
- Pericolonic inflammatory stranding
- Bowel wall defect
- Mesenteric fluid or haematoma
This is particularly true in patients presenting with abdominal pain or guarding following penetrating injury and a low index of suspicion should be had for surgical exploration under these circumstances even in the absence of any firm evidence of bowel injury on CT.
Case 4
A 29 year old male presented following a stab injury to the right upper quadrant.
He was haemodynamically unstable on arrival and was therefore transferred directly to theatre.
Exploratory laparotomy revealed multiple liver lacerations but the IVC was intact.
The liver was packed but the patient remained haemodynamically unstable and continued to deteriorate.
A CT was performed to guide further management,
which revealed multiple abnormalities.
The CT of the thorax demonstrates pneumomediastinum and a small right sided pneumothorax with a right sided chest drain appropriately sited within the pneumothorax (Fig. 25).
There are multiple points of active intra-abdominal haemorrhage.
Despite the presence of extensive packing material in the left lobe of the liver,
there is active haemorrhage within the right lobe (Fig. 26).
Active intra-gastric haemorrhage is also noted arising from a vessel in the anterior wall of the lesser curve of the stomach with a large clot within the lumen of the stomach (Fig. 27, Fig. 28).
In addition,
CT demonstrates active haemorrhage within the anterior abdominal wall superior to the laparotomy wound (Fig. 29).
The patient underwent mesenteric and abdominal wall angiography and embolisation via a right femoral artery approach.
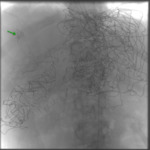
Selective coeliac and hepatic artery angiography demonstrated two clear intrahepatic bleeding points (Fig. 30,
Fig. 31),
these bleeding points were selectively catheterised and embolised with a combination of coils and Gelfoam (Fig. 32).
In addition,
the inferior epigastric angiography demonstrated acute subcutaneous extravasation projected over lateral end of cutaneous clips (Fig. 33). This was also selectively catheterised and embolised.
No active haemorrhage was seen on SMA angiography,
the patients condition then stabilised.
48 hours following embolisation the patient's condition deteriorated.
Initial investigations showed a significant deterioration in liver function (LFTs).
A CT was performed which demonstrates a thrombosed left portal vein and non-enhancement of the left lobe of the liver (Fig. 34,
Fig. 35) in keeping with hepatic infarction.
The precise cause of the liver failure was not entirely understood however,
this was thought to be due to a combination of left portal vein thrombosis secondary to vascular injury,
selective hepatic artery embolisation,
intra-abdominal compartment syndrome related to the packing material and a generalised hypo-volaemic state.
Key learning point: This case demonstrates the added role of CT in guiding management in the unstable patient following initial surgical temporising measures.
CT is invaluable in this particular setting in diagnosis and to aid further interventional management.
Abdominal compartment syndrome from hepatic packing is rare however the "overpacking" of the liver to attempt to establish haemostasis is a described cause of abdominal compartment syndrome 6,7.
Hepatic dysfunction should prompt consideration of abdominal compartment syndrome as a cause of deterioration in this cohort of patients.
Case 5
A 17 year old male presented to the emergency department following a stab wound to left flank,
he was haemodynamically unstable on admission.
He was stabilised with initial resuscitation measures.
Admission CT demonstrates a single skin entry site in the left flank,
with a cranial wound trajectory demonstrated by multiple small blebs of subcutaneous gas that extend superiorly (Fig. 36, Fig. 37).
There is a large haematoma as well as active haemorrhage within the muscles of the lateral abdominal wall along the knife wound track (Fig. 37,
Fig. 38).
The wound track extends to a full thickness splenic laceration,
which reaches the splenic hilum (Fig. 39, Fig. 40).
A rounded high density focus within the laceration was presumed to be active extravasation of contrast consistent with active haemorrhage at the time of reporting (Fig. 39,
Fig. 40).
On re-review this was felt to possibly represent a traumatic pseudoaneurysm (Fig. 39,
Fig. 40,
Fig. 41).
Selective catheterisation of the coeliac and splenic arteries was performed via a right CFA approach. No pseudoaneurysm was seen on angiography (Fig. 42). Follow up CT 4 days later also confirmed resolution of the previously seen vascular abnormality at the splenic hilum.
The patient underwent surgical evacuation of the splenic haematoma and settled thereafter. Follow up CT two weeks later demonstrated a resolving haematoma with no vascular splenic abnormality,
the patient made a full recovery.
Key learning point: Delayed haemorrhage is common in the setting of the traumatised spleen,
there should be a low threshold for early interval re-imaging in this cohort to exclude delayed complications; or earlier if the patient becomes symptomatic.
Case 6
A 60 year old male presented following a stabbing to left side of neck.
The patient was haemodynamically unstable on admission therefore underwent primary surgical neck exploration.
Surgical exploration revealed a transected left internal jugular vein,
which was surgically ligated.
Active bleeding was also identified from left vertebral artery between the C5 and C6 transverse processes. This was not amenable to suturing but haemostatic material was applied to the area to attempt to stem the bleeding.
The patient was transferred to intensive care where there was a subsequent sudden neurological deterioration. CT of the head and neck was performed to look for a vascular or haemorrhagic cause for the sudden deterioration.
Pre and arterial phase CT from the aortic arch to circle of Willis was performed.
This demonstrates post-operative changes throughout the left side of the neck (Fig. 43),
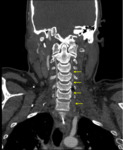
there is no evidence of active haemorrhage or dissection however the left vertebral artery has an abrupt transition at the C7/T1 level with no contrast seen distal to this point (Fig. 44,
Fig. 45).
The intracranial vessels are also very poorly opacified and the CT brain demonstrates diffuse cerebral swelling with hydrocephalus in keeping with hypoxic brain injury.
Key learning point: It is important in the post-operative patient to pay close attention to the absence of flow in vessels as a sign of vascular injury as this may not be apparent at surgical exploration.
In haemodynamically stable patients who proceed immediately to CT,
surgical exploration is still advised even in the absence of visceral or vascular injury on imaging in the context of a deep penetrating injury.