Imaging techniques:
• High resolution computed tomography (CT) and magnetic resonance (MR) imaging are both necessary modalities that complement each other to evaluate the patients with sensorineural hearing loss.
• CT is used for visualize the osseous structure and classify the inner ear malformation.
Also,
preoperative CT examination is a good guide for surgeon that allows the additional information about middle ear and mastoid aeration,
the course of fascial nerve and anatomic variations.
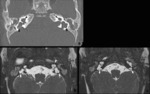
• CT of the temporal bone should be obtained in coronal and axial planes.
Axial plane should be parallel to the lateral semicircular canal.
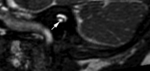
• MR is essential for detecting the presence of cochlear nerve.
It is an important issue because absent cochlear nerve is a contraindication to cochlear implantation surgery.
• 3D fast-recovery fast spin-echo pulse sequence with oblique sagittal plane should be obtained to see the nerves.
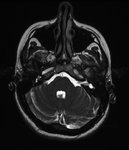
• Axial T2 weighted imaging of the brain should be done to evaluate the brain parenchyma if there is any associated malformation.
Anatomy and development of the inner ear:
• The inner ear arises from the otic placode in the 3th week of gestation.
The development of the cochlea and vestibule is completed by the 8th week and 11th week,
respectively.
The semicircular canals formed between 19th and 22nd weeks.
Inner ear malformations occur if there is a developmental arrest in this embryological process.
• The inner ear occurs from osseous labyrinth that contains membranous labyrinth.
The osseous labyrinth consists of cochlea,
vestibule,
semicircular canals (SCC),
vestibular and cochlear aqueduct.
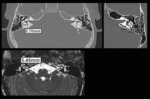
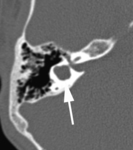
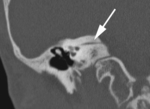
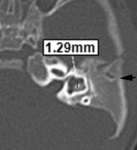
• The normal diameter of the vestibular aqueduct should be less than 1.5 mm or approximately equal to the diameter of posterior semicircular canal.
• The normal diameter of internal acoustic canal is 2-8 mm and less than 2 mm is called stenotic.
• The transverse diameter of the lateral SCC bony island is between 2.6 and 4.8 mm and < 3.3 mm defined as dysplasia.
• The vestibule should be smaller than or equal to the bone width between the lateral vestibular wall and the inner wall of the lateral SCC.
Vestibule diameter is between 4-6 mm and lateral SCC diameter is nearly equal to horizontal and mastoid portion of the facial nerve canal.
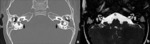
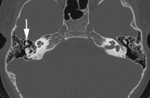
Fig. 1
Congenital malformations of the inner ear:
The classification of inner ear malformations are based on embryogenesis and the gestational age at which developmental arrest occurred making the list severe to mild.
1.
Labyrinthine Aplasia: The most severe form,
occurs only 1% of all inner ear malformations.
• Time of arrest: 3rd week
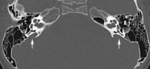
• Imaging findings: Fig. 2
- Complete absence of the inner ear structures (cochlea,
vestibule and semicircular canals)
- Aplasia or hypoplasia of the otic capsule
- Aplasia or hypoplasia of the internal auditory canal
- MRI: absence of vestibulocochlear nerve
• Associated middle ear and/or external auditory canal malformations: Normal or hypoplastic middle ear.
Ossicles might be normal or malformed stapes can be associated.
• Associated brain abnormalities: Posterior fossa abnormalities such as large cerebellopontin angle cistern,
arachnoid cyst or pontine anomaly can be seen. Fig. 3
• Additional findings and clues:
- Follow the facial nerve canal on CT.
An anomalous course of facial canal can be found.
- A flat medial wall of the inner ear,
hypoplasia of the petrous apex are the best clues to differentiate from labyrinthine ossificans.
- Look carefully for the contralateral inner ear.
Other malformations such as common cavity,
inner ear hypoplasia or IP-I anomaly can be associated.
2.
Cochlear Aplasia:
• Time of arrest: Late 3rd week
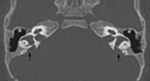
• Imaging findings: Fig. 4 Fig. 5
- Complete absence of the cochlea
- Vestibule and semicircular canals may be normal but they are often malformed
- Cochlear promontory is flattened
- Internal auditory canal is usually hypoplastic
- MRI: absence of cochlear nerve
• Associated middle ear and/or external auditory canal malformations: Middle ear has a normal view and size.
Stapes may be normal or malformed.
• Associated brain abnormalities: Not defined
• Additional findings and clues:
- Differentiation cochlear aplasia from labyrinthine ossificans is an important issue.
Look for the shape of the cochlear promontory.
Flattened promontory indicated cochlear aplasia whereas the bulge of the promontory produced by basal turn shows labyrinthine ossificans.
3.
Common Cavity
• Time of arrest: 4th week
• Imaging findings: Fig. 6
- Cochlea and vestibule form one cystic cavity with no internal structure.
- Posterior and superior semicircular canals may be normal but usually malformed.
Horizontal semicircular canal includes in common cavity.
- If the cystic cavity is large,
internal auditory canal can be also dilated.
- MRI: Vestibulocochlear nerve is small or absent component
• Associated middle ear and/or external auditory canal malformations: Stapes may be normal or malformed.
• Associated brain abnormalities: Not defined
• Additional findings and clues:
- Differentiation common cavity from cochlear aplasia with vestibular dilatation is very important,
because cochlear implantation may have good results in common cavity but in cochlear aplasia there will be no stimulation.
- Common cavity has a round shape and is located more anteriorly.
On the other hand in cochlear aplasia with vestibular dilatation,
the outer border of vestibule and semicircular canals seem to be normal and they are located in normal position.
4.
Cystic cochleovestibular malformation (incomplete partition type 1,
IP-1)
• Time of arrest: 5th week
• Imaging findings: Fig. 7
- Cystic cochlea without internal structure separated from dilated vestibule and horizontal semicircular canal.
- The modiolus is absent
- Internal auditory canal is usually dilated
- Vestibular aqueduct is usually normal
- MRI: Vestibulocochlear nerve is hypoplastic or absent
• Associated middle ear and/or external auditory canal malformations: Oval window stenosis and abnormal stapes can be seen.
• Associated brain abnormalities: Not defined.
Spine anomalies can be seen.
• Additional findings and clues:
- Figure 8 view helps to distinguish IP-1 from common cavity.
- Normal vestibular aqueduct might be helpful to differentiate from IP-2,
because vestibular aqueduct is usually dilated in IP-2.
5.
Cochlear hypoplasia:
• Time of arrest: 6th week
• Imaging findings: Fig. 8
- Small cochlea often with lack of internal structure and has less than 2 turns
- Vestibule and semicircular canals can be normal,
hypoplastic or enlarged
- Vestibular aqueduct can be normal or dilated
- MRI: Cochlear nerve is often absent or hypoplastic Fig. 9
• Associated middle ear and/or external auditory canal malformations: Not defined.
They are usually normal.
• Associated brain abnormalities: Not defined.
• Additional findings and clues:
- Three types of cochlear hypoplasia have been described;
- Type 1: The cochlea is small and derive from internal acoustic canal like a bud.
Modiolus and interscalar septum can not be described.
- Type 2: The cochlea is small and cystic appearance.
Modiolus and interscalar septum can not be described.
- Type 3: The cochlea has less than 2 turns.
Shortened modiolus and interscalar septum can be seen.
6.
Incomplete partition type 2 (IP-2) :
• Time of arrest: 7th week
• Imaging findings: Fig. 10
- Absence of interscalar septum between apical and middle turns giving a view of cystic apex.
The modiolus of basal turn is present.
- Vestibular aqueduct is typically large
- Vestibule can be normal or enlarged
- MRI: cochlear nerve is usually normal
• Associated middle ear and/or external auditory canal malformations: Not defined.
• Associated brain abnormalities: Not defined.
• Additional findings and clues:
- Baseball cap cochlea can be a sign to remember easily.
- Mondini’s triad: cystic apex,
dilated vestibular aqueduct,
enlarged vestibule.
7.
Incomplete partition type 3 (IP-3): In this type,
the interscalar septum is present but modiolus is completely absent.
The cochlea is located immediate lateral to internal acoustic canal rather than its anterolateral position.
This malformation has been described in X linked deafness.
Large vestibular aqueduct and endolymphatic sac:
• The most common imaging abnormality in pediatric population with sensorineural hearing loss.
• Patients often present with fluctuating hearing loss after a trauma.
• Mostly bilateral (90%) but it can be also asymmetric.
• Large vestibular aqueduct is a result of a developmental anomaly in the 7th week of gestation but vestibular aqueduct continues to develop until birth.
Therefore it may be seen isolated or accompany with other inner ear anomalies.
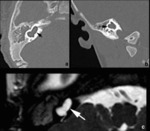
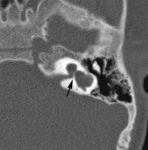
• CT findings: The width of the vestibular aqueduct is larger than 1.5 mm or simply larger than posterior semicircular canal.
Fig. 11 Fig. 12
• MRI findings: Enlarged endolymphatic sac
• Associated abnormality: Large vestibular aqueduct is frequently seen in Pendred syndrome which is described with sensorineural hearing loss and euthyroid goiter.
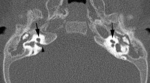
Semicircular canal aplasia and dysplasia:
• The developmental process of the semicircular canals is between 8th and 22th weeks of gestation.
• Superior semicircular canal develops first and lateral semicircular canal last.
Therefore,
when superior and posterior semicircular canals are malformed,
lateral semicircular canal is expected to be anomalous.
• The malformed canal is usually short and wide but it may be narrow.
Also,
in some cases a dilated vestibule may communicate with lateral semicircular canal dysplasia forming a single cavity.
Fig. 13
• Associated abnormality: Waardenburg and Alagille syndromes are associated with isolated hypoplasia of the posterior semicircular canal.
Absence of all semicircular canals and vestibular dysplasia may be seen in CHARGE syndrome.
Cochlear nerve anomaly:
• Aplasia or hypoplasia of the cochlear nerve.
• It is best evaluated on oblique sagittal MR images obtained in a plane perpendicular to the long axis of the internal acoustic canal.
In this plane,
cochlear nerve should be seen at anteroinferior position.
Also,
cochlear nerve diameter should be almost equal to facial nerve (0.4 mm).
• On CT,
less than 2 mm of the internal acoustic canal is described as stenotic.
This finding may refer to the cochlear nerve anomaly,
but it is important to know that normal internal acoustic canal and inner ear do not exclude a cochlear nerve deficiency.
Fig. 14
Acquired conditions as a cause of sensorineural hearing loss:
• Acquired sensorineural hearing loss may be the result of labyrinthitis,
trauma,
autoimmune disorders,
posterior fossa or internal acoustic canal tumors.
Therefore,
they must be ruled out before diagnosing congenital inner ear malformations.
Other imaging findings:
• Imaging findings that may help the surgeon before the operation and may cause complications in this process should be reported.
• Increased internal acoustic canal diameter is not an anomaly but should be noticed due to the risk of CSF leak after surgery.
Fig. 15
• On CT examination,
mastoid and middle ear aeration should be controlled before surgery.
Also,
mastoid sclerosis should be reported because it may complicate the surgery.
Fig. 16
• Anomalies of external and middle ear may rarely associate with inner ear malformations but still should be noticed because malformed ossicle can be the main cause of hearing loss.
Fig. 17 Fig. 18
• Aberrant carotid artery,
high jugular bulb,
carotid or jugular dehissence are variations that should be evaluated.
Also,
emissary veins should be noticed because of the possible complications after surgery.
Fig. 19
• Abnormal course of the facial canal is not an uncommon finding in congenital inner ear malformations.
It is important to report this abnormality to prevent a facial nerve injury during the operation.
Fig. 20