- Normal thyroid anatomy
The thyroid is a gland located anteriorly in the lower neck,
in the infrahyoid region,
overlying the trachea and inferiorly to the sternothyroid and sternohyoid muscles,
extending from the level of the fifth cervical vertebra down to the fist thoracic.
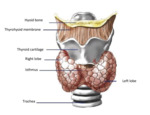
[1] It is formed by 2 lateral lobes located on both sides of the trachea,
connected by a median isthmus, Fig. 1
The arterial supply to the thyroid gland comes from the superior thyroid artery,
which is the first anterior branch of the external carotid artery,
and inferior thyroid artery,
a branch of the subclavian artery.
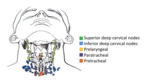
Lymphatic drainage courses predominantly from cervical level VI nodes (pretracheal,
paratracheal,
prelaryngeal,
perithyroid,
and perirecurrential nodes). Fig. 2
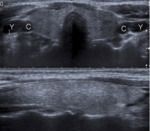
Ultrasound is the modality of choice to assess the thyroid gland.
Normal thyroid tissue appears homogeneously echogenic with a uniform echotexture.
It has a higher echogenicity than the overlying strap muscles of the neck and less than the subcutaneous tissue.
Fig. 3 The thyroid lobes are normally 4-6 cm in craniocaudal length and 1.3–1.8 cm in their anteroposterior dimensions; being the AP diameter the most accurate to determine the increase in size of the gland,
which is considered pathological when it is greater than 2 cm.
The isthmus normally has an anteroposterior thickness of 0.4 - 0.6 cm.
- Hashimoto's thyroiditis
Hashimoto's thyroiditis,
also known as chronic lymphocytic thyroiditis,
is the most common autoimmune disease of the thyroid and the most frequent cause of spontaneous hypothyroidism in adults.
This disease is 15 – 20 times more frequent in women than in men.
It occurs mainly during the 2nd to 5th decades,
but may be seen in any age group.
Hashimoto’s thyroiditis has a broad spectrum of sonographic appearances,
from almost normal thyroid parenchyma to alterations that often mimic other thyroid disease.
The etiology of the disease is unknown,
it is thought to be multifactorial,
including genetic susceptibility and environmental factors (infections and high iodine intake) [2].
In this autoimmune disease the thyroid gland becomes infiltrated by B and T lymphocytes,
which are activated by thyroid antigens.
Activated B cells secrete antibodies against thyroglobulin (anti-TG) and thyroid peroxidase (anti-TPO).
Thyrotoxic T cells are responsible for the destruction of the glandular parenchyma,
with consequent initial thyrotoxicosis followed by hypothyroidism.
Clinically it is characterized by a diffuse enlargement of the thyroid gland and gradual development of hypothyroidism,
with or without pain and cervical adenopathies.
The clinical diagnosis is confirmed with serology,
where we can find low levels of thyroxine (T4),
increase of the stimulating hormone of thyrotropin (TSH) and high levels of anti-TPO antibodies in 95% cases and anti-TG in 70% of them.
However,
it is not uncommon that patients with Hashimoto`s thyroiditis do not have clinical symptoms,
and neither elevated antibodies.
Taking this into account,
the diagnosis based on clinical findings and laboratory would under-diagnose the disease.
The performance of a thyroid ultrasound study,
together with clinical and serological data,
increases diagnostic sensitivity and specificity [2].