A) COMMON LESIONS
In this group we can find the cystic variants of classical solid lesions.
1) Relatively uncommon (2-3% of all cases of RCC),
it shows the best prognosis of all cases of RCC,
it was forst described in 1928,
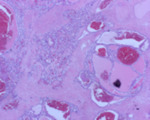
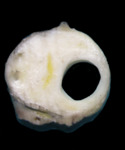
multilocular cystic clear cell carcinoma (Fig 1,
Fig 2) was included in the WHO 2004 classification.
They are characterized by a malignant cell lining and small collections of cells without formation of a malignant nodule (Fig. 1 ).
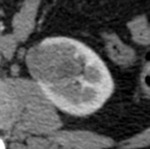
The patologic criteria for the diagnosis are strict in order to reduce the overlap with clear cell renal cel carcinomas (ccRCCs) (Fig. 2 ,
Fig. 3 ) undergoing necrosis (Furham 3 or 4),
with a worse prognosis.
Infact multilocular cystic clear cell carcinoma is considered a less aggressive subtype of ccRCC (Furham grade 1 or 2) with a benign behaviour; there are no reported cases of progression to metastasis.
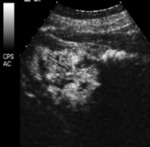
On Imaging evaluation multilocular cystic clear cell renal cell carcinoma appears as a Bosniak III or IV lesion ( Fig. 4 ),
with thickening enhancing internal septations and without solid enhancing nodules.
A good evidence can be obtained with CT ,
with MRI and with CEUS as well; in this case the high spatial resolution gives a detailed depiction of the septa (Fig. 6) .
2) Accounting for 13-15 % of RCCs,
papillary RCCs (PRCC) may be cystic as gross feature ( Fig. 7 ).
It is known that tumors of type 2 - characterized by higher nuclear grade and containing more than one layer of abundant eosinofilic cytoplasm - are often characterized by a larger size and associated with areas of hemorrhage.
In some cases it can be due to their inherent architecture.
Generally speaking a uniloculkar cystic RCC tends to be of the papillary subtype; it is characterized by a simple cyst with a nodule within it or with tumor growth filling part of it (Fig. 8).
Although cystic degeneration can occur in pRCCs as well as in ccRCCs,
the analysis of enhancement characteristics helps differentiate between the two subtypes.
When can be performed - in the solid portions of the lesion - ARFI can be useful because observed values in ccRCCs tend to be higher than values observed in pRCCs.
At MRI pRCC shows a pseudocapsule and after contrast administration - as in CT ( Fig. 9) - enhancement is less intense.
At CEUS evaluation a pseudocapsule and a low-enhancing solid portion can be detected ( Fig. 10) .
B) UNCOMMON MESENCHYMAL TUMORS
In this group we can find the so-called Renal Epithelial and Stromal Tumors - REST - (i.e.
cystic nephroma and Mixed Epithelial and Stromal Tumors) and the Angiomyolipoma with Epithelial Cyst - AMLEC.
1) Cystic nephroma (Fig. 11) is a circumscribed mass of cysts with fibrous septa,
uncommon areas of calcification and regions of ovarian-like stroma.
Unlike in multilocular cystic ccRCC the cysts - wich do not communicate with each other - are lined by cubouidal cells epithelium and do not exhibit evidence of clear cell proliferation ( Fig. 12) .
On CT Imaging it is a well marginated mass with septa enhancing slowly after contrast medium administration (Fig. 14).
The same can be see when performing CEUS ( Fig. 14).
2) MEST is a tumor occuring almost exclusively in post menopausal women.
They are complex solid and cystic lesions ( Fig. 15) with stromal components consisting of spindle cells mimicking ovarian stroma and expressing hormonal (i.e.estrogen and progesterone) receptors.
Their classical CT apparence is a septate cystic or solid mass ( Fig. 16) characterized by a delayed enhancement ( Fig. 17) ; this characteristics can well be seen also at US with contrast administration ( Fig. 18) .
The delayed enhancement can depend on the spindle cell components of these tumors,
and it is generally more intense in densely cellular areas.
3) Angiomyolipoma with epithelial cysts (AMLEC) is an extremely rare subtype of fat poor angiomyolipoma,
i.e.
those containing too little fat to be detected ewith unhenanced CT.
It is characterized by myomatous component with poorly arranged bundles of smooth muscles and dysplastic blood vessels.
Mullerian-like or endometrioid stroma stanning positively for estrogen and progesterone and variable cysts ranging from 1 to 6 cm,
lined with epithelium.
In the majority of the reported cases AMLEC was seen as a multilocular cystic mass containing a solid portion hypointense on T2 w images - due to smooth muscle component - and homogeneously enhancing after contrast medium administration.
C) NEW EPITHELIAL TUMORS
In this group we can include MiTF family tumors and tubulocystic renal cell carcinoma as well as acquired cystic disease-associated RCC macro and microcystic,
hereditary leiomyomatosis RCC syndrome-associated RCC; clear cell papillary can rarely be macro or micro-cystic.
1) Traslocation RCCs (i.e.Xp11,
t(6:11) ( Fig. 19) were first included as a separate entity in the 2004 WHO classification.
They show a cystic pattern in 15% of the cases ( Fig. 20) .
Histological presentation is characterized by a papillary or a nested architecture with a granular eosinophilic cytoplasm.
The prognosis is poor.
At CT scans is is characterized by high attenuation at unenhanced scans and frequent calcifications ( Fig. 21).
After contrast medium administration the lesion enhances poorly wqhen compared with the renal cortex (Fig. 22) ; the same pattern can be detected using CEUS (Fig. 23) .
Differential diagnosis is expecially with papillary RCCs which are characterized by smaller diameter,
less frequent calcifications and lower enhancement.
2) Tubulocystic renal cell carcinoma is a newly identified pathological entity,
first described in 2005; it is mainly cystic and rarely metastasizes.
It is characterized by duct-like structures with cysts lined by a single layer of low cuboidal epithelial cells with areas of hobnail appearence.
These structures are separated by a fibrous stroma.
The US pattern is characteristic,
showing a combination of high echogenicity and posterior acoustic enhancement; this is due to the presence of very small acoustic spaces separated by multiple septa.
No vessels can be detected by Doppler mode although it is clearly showed using CEUS ( Fig. 24).
CT evaluation is very difficult because the detection of enhancement at CT scans is critical,
due to the very low vascularity ( Fig. 27,
Fig. 25) .
MRI - due to its high sensitivity to detect fluid content - appears more helpful to characterization ( Fig. 26) .
3) Acquired cystic disease associated RCC (ACD-RCC) is the most common subtype of RCC occuring in end-stage kidneys,
expecially in those with acquired cystic disease.
Long duration of dyalisis has a stronger association with ACD-RCC compared with other subtypes arising in this setting.
They appear as nodules arising from cyst wall,
occasionally filling these cysts,
although they can also be solid masses separated from the cysts.
Multifocality can be seen in >50% and >20% of the cases respectively.
They can show different architectural pattern - acinar,
tubular,
papillary,
micro and macrocystic.
Since papillary architecture is quite frequent misinterpretation as type 2 PRCC is not uncommon.
It has a goood prognosis also because most cases are diagnosed early in Patients on long term follow up for CKD.
4) Clear cell papillary RCC is composed of clear cells of low nuclear grade with variable papillary,
tubular/acinar and cystic architecture; a linear arrangement of nuclei,
away from the basal aspect of the cells - is characteristic.
They are well cisrcumscribed and usually encapsulated,
with fibrotic areas; their apparence range from completely solid to predominantely cystic; they usually are unicentric and small; the largest one reported in Literature is 6 cm.
No metastases have been reported although follow up cases are very few.
5) Hereditary leiomyomatosis RCC-sindrome associated RCC (HLRCC) eas first described in WHO 2004 classification but defined as an hereditary counterpart of type 2 PRCC,
which is very similar.
Now - due also to its aggressive behaviour - is considered as a different subtype.
Tye syndrome is an autosomal dominant one and is associsated with a mutation of a gene (funarate hydratase) located at 1q42 chr.
These Patients show multiple cutaneous and uterine leiomyoma; almost 1/3 of them are affected and present with advanced disease.