This was a prospective observational single-center study enrolling neonates delivered by cesarean section (either elective or emergency) in our University Hospital in a period from December 2016 to March 2017.
All infants with a prenatal diagnosis of congenital heart or pulmonary disease,
other major congenital malformation or chromosome abnormalities were excluded from the study.
The criteria for the definition of respiratory distress were a breath rate ≥ 65 breaths/minute associated with at least one other symptom such as tachycardia (heart rate > 190 bpm),
chest wall or jugular retractions,
nasal flaring,
expiratory grunting and hypoxia (SpO2 < 85% in room air) [1]. Umbilical-cord blood gas analysis (pH and Base Excess) and O2-Saturation (Sat-O2) were included in the clinical evaluation.
To predict the risk of hospitalization we considered also: Gestational Age (GA),
Birth Weight (BW),
intra-uterine growth restriction (IUGR),
sex,
Apgar score (1 minute and 5 minutes after birth),
type of caesarean delivery (elective or in urgency),
type of pregnancy (single or twin pregnancy) and presence of gestational diabetes.
LUS was carried out in the first 30 minutes of life (T0) directly in the delivery room,
with infants in supine position in the incubator.
The operator was blinded to the clinical status of the patient.
A second check was performed 4 hours after birth (T1). All examinations were performed using a portable sonographic scanner (Cx50,
Philips,
USA) equipped with a high frequency (7,5-13 MHz) linear array probe (also known as “hockey stick”) with a depth of 3 cm.
We divided each hemitorax into 4 areas delimited by parasternal,
anterior and posterior axillary lines: antero-superior / antero-inferior / lateral-superior / lateral-inferior.
We didn’t examined posterior areas of the chest to minimize the handling of the infants.
Longitudinal (probe perpendicular to the ribs) and transversal (probe parallel to the ribs) scans of each zone were obtained.
We assigned a score to each lung using a three point scale adapted from a previously validated score by Raimondi et al.
and based on the presence and density of B-lines, hyperechoic vertical comet-tail artifacts that reflect the presence and the entity of fluid accumulation in the alveolar-interstitial space [4-5].
Each lung was classified as:
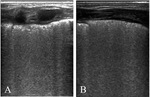
- “Type 1”: uniform hyper echoic appearance of the lung caused by the presence of coalescent B-lines (White Lung) [Fig.1];
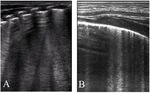
- “Type 2”: characterized by numerous non compact B-lines (Black and White lung) [Fig.2];
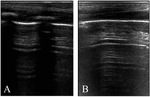
- “Type 3”: normal aerated lung,
without B-lines and with the presence of A-lines,
horizontal hyper echoic lines parallel to the pleural line (Black lung) [Fig.3].
Patients were then classified in 5 different profiles based on the appearance of both lungs: A (both lungs type 1),
B (one lung type 1),
C (both lungs type 2),
D (one lung type 3),
E (both lungs type 3).
Statistical Analysis:
Statistical analysis was performed using the IBM software SPSS Statistic v.20.
The univariate relation between hospitalization and possible predictive factors of admission to the NICU was assessed using the Chi Square test for categorical data and the Students t test for continuous variables.
Then,
multivariate logistic regression analysis was performed,
using hospitalization as dependent variable and the significant variables identified on univariate analyses as independent variables.
In all tests p values ≤ 0,05 were considered statistically significant.
We defined as “True Positive” (TP) all infants with Profile A and B (ie total LUS score ≥ 2,5) admitted to the NICU,
“False Positive” (FP) infants with Profile A and B who did not required admission to the NICU,
“True Negative” (TN) infants with Profile C,
D and E (ie total LUS score < 2,5) who did not required hospitalization,
and “False Negative” (FN) infants with Profile C,
D and E admitted to the NICU.
Sensitivity is defined as TP/(TP+FN),
Specificity as TN/(TN+FP); Positive Predictive Value (PPV) is defined as TP/(TP+FP) and Negative Predictive Value (NPV) as TN/(TN+FN).