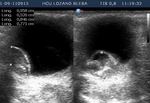
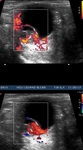
Technique
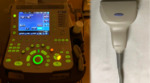
Conventional B Mode US technique requires a high frequency (10-15 MHz) linear transducer,
preferably a small one,
as it will match with the eye socket size. Fig 3
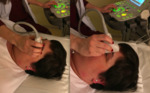
Ocular sonography in the emergency departament is performed with the patient in supine position with his eyelids gently closed.
The sonographer should hold the probe using the thumb and index finger while the remaining fingers stabilize the arm by resting on the maxilla,
supraorbital ridge,
or other bony structures. Fig 4
Careful technique is essential in order to avoid anisotropy due to the contours of the eye.
To avoid this pitfall,
the transducer may be gently placed along the anterior wall of the eye,
with minimum pressure,
especially in a postraumatic context.
A generous amount of gel is necessary,
in order to prevent excesive pressure,
which can cause discomfort and/or damage to the eye,
allowing the examiner to dinamically scan transverse (axial),
oblique and longitudinal sections of both eyeballs. In case of unilateral symptoms,
the healthy eye acts as a control to confirm or exclude pathology.
Ideally patients must perform extraocular movements to perform a dynamic scan.
The examiner should also evaluate movements of ocular tissues,
such as convection and aftermovements.
Convection represents slow spontaneous motion of particles within a cavity (i.e.
in endophthalmitis); aftermovements are defined as continued tissue motion after cessation of eye movement (i.e.
after vitreous detachment).
Depth should be set to appropriately visualize all the ocular structures,
including the optic nerve,
and the gain should be set to create a hypoechoic posterior chamber.
Setting the gain too high can cause the sonographer to overestime some findings as small artifacts in the posterior chamber that can mimic blood or foreign bodies.
Working with low gain will cause the sonographer to miss subtle pathology.
Finally,
adding Color and pulsed Doppler is useful in cases difficult to diagnose otherwise,
and in cases of suspected vascular abnormalities such as central retinal vessel occlusion,
as well as in inflammatory diseases or tumors.
Low-flow settings and a small gate should be chosen for Doppler studies.
Indications and contraindications
Main indication is when opacification of light-conducting transparent media occurs,
because the complete assessment of the posterior segment through clinical ophthalmoscopy is not posible.
Scenarios include patients with cataracts,
hyphema,
hypopyon,
vitreous opacifications (hemorrhage),
extreme miosis or eyelid problems,
and with ocular globe lesions such as posterior wall masses,
vascular abnormalities or detachments.
US can also demonstrate or provide aditional information in cases of anterior segment pathology (i.e. Cristallyne luxation).
Ocular US must not be performed if there is a suspicion or signs of ocular rupture in post-traumatic patients (i.e.
an asymmetrical eyeball) or in those who recently underwent surgery because it may cause extrusion of ocular content.
Imaging features
Frequent pathology of the anterior chamber
Prior knowledge of surgical history of patients is important.
IOL implants can produce a posterior reverberation artifact,
depending on the incidence of the ultrasonic beam.
In the presence of hyphema,
the anterior chamber appears hyperechoic,
but the main purpose of US is to rule out associated injuries.
Post-traumatic abnormal position of the crystalline lens (Ectopia lentis) is the most common condition of the anterior chamber that can also be demonstrated by US,
usually posterior and rarely anterior.
We will appreciate the lens "floating" in the vitreous chamber as a sign of luxation,
or partially attached to the ciliary body in partial dislocations (subluxation).
It is sometimes useful to scan patients in different positions.
Important pathology of the posterior segment
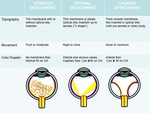
The main role of the US is in evaluating opacified structures posterior to the lens and depict associated membrane detachments. Table 1.
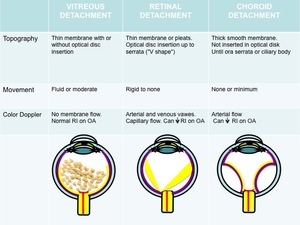
Table 1: Differential diagnosis of the posterior segment detachments.
References: © Raquel Navas Campo, MD.
Vitreous
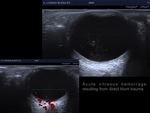
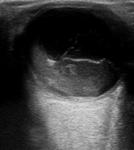
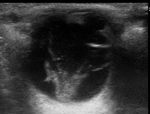
Vítreous haemorrhage: Fig 5 to 6
Vitreous haemorrhage spreads diffusely into the gelatinous vitreous and frequently obscures the retina from funduscopic visualization,
and as such constitutes one of the main clinical signs to indicate a US scan to rule out aditional findings in the emergency room.
Hemovitreous appearance varies with the severity and onset of the bleeding,
from subtle mild hemorrhages in early phases to more stiffed and echogenic membranes with organized fibrinous appearance.
Can be spontaneous,
traumatic,
related to retinopathy or tumors.
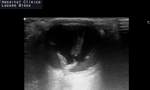
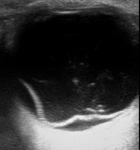
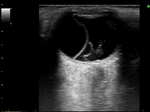
Posterior vitreous detachment (PVD): Fig 6
The posterior capsule or hyaloid membrane detaches from the underlying retina anywhere posterior to the vitreous base,
depending of the severity.
Hyaloid membranes are not usually attached to the optic disc or ora serrata and are visualized as structures with weaker echogenicity and more variable thickness.
PVD is seen as an undulating membrane freely moving on the dynamic scanning (aftermovement), with greater mobility than retinal detachments.
Retrohyaloid space can be also occupied with haemorrhage. Fig 7
PVD is associated with myopic or macular degeneration and can be encountered as an asypmtomatic incidental find¡ng.
Retina
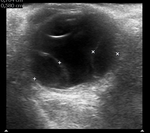
Retinal detachment: Fig 8 to 11
The neurosensory retina separates from the outer pigmented layer.
Three types are described based on the underlying mechanism:
Rhegmatogenous detachment,
associated with a retinal tear,
is the most common type and is seen in elderly patients,
and associated with myopia.
Tractional detachment originates in adjacent vitreous strands.
Exudative detachment is due to fluid,
blood,
or lipids in the subretinal space and can be associated with tumors of the choroid.
Complete separation appears as an echogenic line fixed at the papilla and extends to the ora serrata.
The detached retina forms a typical V shape with the apex at the optic disc.
Differentiating retinal detachment from others in the posterior segment is difficult in cases where the detachment is shallow or focal (different morphologic characteristics),
other structures are attached to the optic disc or ora serrata,
in a chronic state with high echogenicity,
or in those with multiple detachments.
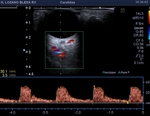
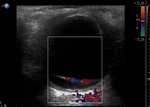
In cases with such atypical morphology in B-mode US,
colour Doppler US adds additional and more reliable information,
by enabling detection of blood flow in the detached retina. Fig 11
Resistance index in the ophthalmic artery is measurable and can be decreased.
Choroid
Choroidal detachment: Fig 12 to 14
It is a detachment of the choroid from the underlying sclera due to fluid accumulation in the potential suprachoroidal space.
Causes include inflammatory pathology (uveitis),
blood (trauma,
surgery),
or choroidal tumors.
Typically appears on ultrasound as a two thick convex and barely mobile lines extending from the ciliary bodies to a point on both sides of the papilla,
creating an obtuse angle and sparing the optic disk.
Choroidal tumors: Uveal Melanoma: Fig 15 to 17
Malignant melanoma is the most common primary intraocular tumor and occurs more often in the choroid,
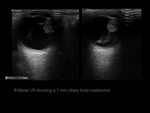
the iris or the ciliary body.
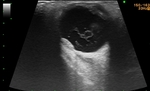
Melanomas of the eye are usually round lobed hypoechoic lesions,
with marginal retinal elevation and no calcifications.
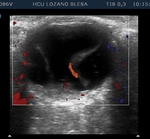
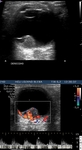
Color Doppler US usually shows vascular flow with low resistance.
They can be associated with several complications like vitreous hemorrhage,
retinal and choroidal detachments.
Fig 16
Choroidal metastases: Fig 18 to 19
Metastases to the eye are most common from the breast,
lung,
and unknown primary. Metastatic tumors appear as posterior wall irregular masses,
hyperechoic compared with melanoma and with a more discoid shape.
In Color Doppler US mode metastases demonstrate higher flow than melanoma. Fig 19