This topic is divided in two sections.
The first one will focus on the appropriate positioning of the examinee,
ultrasound technique and normal ultrasound findings,
illustrated with images of the relevant anatomical structures of the forefoot.
The second section will cover ultrasound findings of various forefoot disorders,
showing examples of traumatic,
degenerative and inflammatory processes as well as several non-neoplastic soft tissue masses.
In some cases,
correlation with other imaging techniques will be displayed.
1.
Scanning technique and normal ultrasound examination
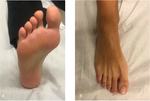
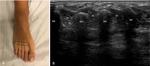
The examination should be performed with a high frequency probe.
The patient should be supine,
with the limb in extension or in slight flexion,
according to the approach being used,
plantar or dorsal,
respectively (Fig. 1).
As is true for the remaining musculoskeletal system,
the approach and technique in ultrasound of the forefoot varies according to the clinical scenario,
with specific positions or maneuvers for each structure and suspected pathology.
These will be detailed on the section on Forefoot Disorders.
In general,
ultrasound allows evaluation of:
.
metatarsophalangeal (MTP) joint spaces and recesses
.
intermetatarsal (web) spaces
.
subcutaneous tissues
.
cortical bone countours
.
capsuloligamentous complex of the MTP joints,
including the plantar plate
.
muscles
.
flexor and extensor tendons
.
nerves
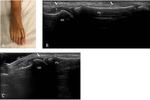
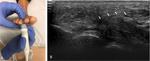
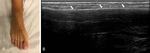
All of these anatomical structures are demonstrated on figures Fig. 2,
Fig. 3,
Fig. 4,
Fig. 5,
Fig. 6,
Fig. 7 and Fig. 8.
2.
Forefoot pathology
In this section the ultrasound features of forefoot disorders (traumatic,
inflammatory,
degenerative and soft tissue masses) will be reviewed,
with correlation with other imaging techniques in selected cases.
2.1.
Trauma
Plantar plate injury/tear
The function of the plantar plate is to limit the hyperextension of the MTP joint.
Injury of the plantar plate is associated with hypermobility,
acute hyperextension trauma,
or wearing high-heeled shoes,
as well as chronic overload.
Usually it affects the second ray,
but it can occur on the first – the so called turf toe.
The disruption of the plantar plate fibers occurs more often at the distal insertion (2).
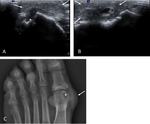
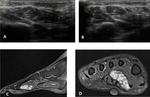
Ultrasound shows a discontinuity of this fibrocartilaginous structure (Fig. 9).
Dynamic examination with flexion and extension of the MTP joint makes diagnosis easier.
Fig. 10 (video file) demonstrates this technique in a normal and torn plantar plate.

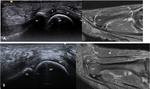
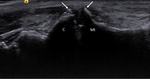
Fig. 10: Dynamic scanning technique of the normal and pathological plantar plate.
With the probe on the longitudinal plane over the plantar aspect of the MTP joint, the plantar plate (PP) should be seen between the metatarsal head (MT) and the flexor tendons (FT). With gentle flexion and extension of the joint, the plantar plate should follow the movement of the proximal phalanx (Ph).
In a patient with a large full thickness tear of the plantar plate (PP), the flexor tendons (FT) glide directly over the metatarsal head (MT). The torn retracted plantar plate (PT) is seen proximally, with a large gap (*) between it and the proximal phalanx (Ph). Dynamic scanning fails to demonstrate significant movement of the plantar plate when the MTP joint is flexed and extended.
Stress fracture
Stress fractures are overuse injuries,
caused either by an increase in physical activity in patients with normal bones (fatigue fractures) or normal physical activity in patients with decreased bone elastic resistency (insufficiency fractures) (1).
Radiographs may be normal until there is periosteal reaction,
which can take a few weeks to appear.
If a stress fracture is suspected,
radiographs should be repeated to confirm the diagnosis.
However,
MRI is considered the gold standard for stress lesions (2).
Ultrasound may also be used in the evaluation of stress fractures.
The patient can usually pinpoint the site of pain,
which helps the operator in precisely positioning the probe.
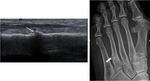
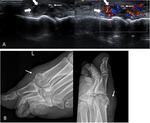
On ultrasound an acute stress fracture appears as a focal discontinuity of the bone contour associated with irregular periosteal elevation (Fig. 11).
An hypoechoic hematoma may also be seen and Doppler signal around the lesion is usually increased (2).
Foreign body
The presence of foreign bodies in the sole of the foot is not a rare finding.
On ultrasound foreign bodies are hyperechoic.
The hyperechoic foreign body may or may not cast an acoustic shadow,
depending on the material being metallic or organic,
respectively.
The formation of an abscess around the foreign body is a possibility,
characterized by low echogenicity,
heterogeneity,
and increased Doppler signal in the periphery.
It must be taken into account that the foreign body can reach a joint or tendon sheath and lead to synovitis or tenosynovitis (2).
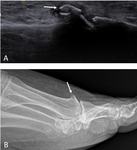
Some of these findings are shown in Fig. 12 and Fig. 13.
Freiberg disease
This condition affects the metatarsal heads,
more often of the second and third rays,
and seems to be related to repetitive or acute injury and vascular compromise,
although its cause is multifactorial.
It is more frequent in young women and wearing high-heeled shoes seems to be a predisposing factor (3).
Ultrasound shows irregularity of the metatarsal head contour and loss of its convexity.
Secondary degenerative changes may be present which can be well depicted on radiographs (4).
Doppler signal may be increased if there is concomitant synovitis (2).
Sesamoiditis
This is a painful inflammatory condition associated with repetitive trauma of the first MTP joint (3).
It is frequently associated with bi or multipartite sesamoids.
Ultrasound may show fragmentation of the sesamoid,
but it is difficult to differentiate this from sesamoid fractures (2).
Also,
ultrasound cannot evaluate bone marrow edema or avascular necrosis.
For these reasons,
ultrasound is not recommended to evaluate this disorder,
and radiographs or MRI should be preferred.
2.2 Inflammatory / degenerative processes
Synovitis
Synovitis refers to inflammation of a synovial membrane (1),
in joints,
tendon sheaths or bursas.
It may be associated with systemic inflammatory diseases,
including rheumatoid arthritis or lupus,
or occur as a secondary local inflammatory response,
as in trauma,
degenerative joint disease,
infection or gout (1,
4,
5).
In general,
the main ultrasound findings are:
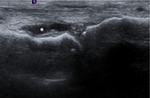
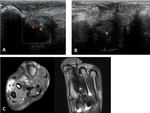
• Thickening of the synovial membrane – hypoechoic hypertrophy of the synovium with increased vascularity on Doppler (4) (Fig. 13).
• Presence of an effusion – anechoic and compressible areas with no Doppler signal.
When doubt arises whether the amount of effusion is physiological or not,
one should perform comparison with the contralateral asymptomatic side (1,
3,
4) (Fig. 14).
• Erosions (in joints) – they are the hallmark of inflammation.
On ultrasound we may find loss of continuity of the intraarticular or periarticular bone contour,
loss of conspicuity of the cartilaginous layer and cartilage thinning.
Erosions should be visible in two perpendicular planes (1,
3).
Tenosynovitis is a frequent finding on patients with inflammatory synovitis (4) (Fig. 15).
It is also important to evaluate the intermetatarsal spaces and the submetatarsal space because there can be associated bursitis (2).
Gout
Gout is a metabolic disease in which articular and periarticular deposition of urate crystal is the key point (2,
6).
Although radiographs are generally the first-line examination,
ultrasound has a high sensitivity in the diagnosis of gout (6).
The first MTP joint is affected in most cases and usually courses with severe pain (5).
Ultrasound nonspecific signs of synovitis can be observed (sinovial hypertrophy with increased vascularity,
effusion and erosions) (2,6).
However,
the most suggestive ultrasound findings are those that reflect the deposition of urate crystals:
• the deposition of urate crystal in articular cartilage forms a hyperechoic line that parallels the bone surface,
resulting in the “double-contour” sign (6).
• the deposition of urate crystal in the synovial membrane or joint effusion gives rise to floating hyperechoic punctiform foci,
the so called “snow storm appearance” (6).
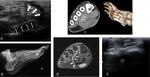
• gouty tophus results from urate deposition on articular or periarticular structures and appears as a heterogeneous irregular mass often with adjacent bone erosion (2) (Fig. 16).
Degenerative joint disease (osteoarthritis)
Osteoarthritis is a common finding on the foot and the first MTP joint is the most commonly affected.
It’s more frequent on the eldery,
the main cause being age-related wear and tear of the joints (3).
Radiographs are the first-line examination,
revealing joint space narrowing,
osteophyte formation and subchondral sclerosis and cysts.
Some of these features may be evident on ultrasound (4) (Fig. 17 and Fig. 18).
Osteomyelitis/Septic arthritis
Osteomyelitis is more common on diabetic patients.
It may result from infection of cutaneous ulcers that spread by contiguity to the underlying metatarsal heads and MTP joint.
This occurs mostly on the first and fifth metatarsal heads / MTP joints (4).
Ultrasound features are nonspecific.
Secondary signs of soft tissue infection should be investigated: cellulitis and soft tissues abcess,
skin ulcer or cortical interruption may suggest an infectious etiology (4).
Septic arthritis may exhibit findings similar to those described on the Synovitis section.
2.3 - Soft tissue masses
Morton’s neuroma
Morton’s neuroma is not a true neuroma,
but represents instead perineural fibrosis associated with interdigital nerve degeneration (5).
It is usually a painful condition,
affecting most commonly the second and third intermetatarsal spaces (7).
Ultrasound has been shown to have a very high sensitivity and specificity for the diagnosis of Morton’s neuroma (2).
Evaluation of the intermetatarsal spaces was described on the scanning technique and normal findings section (Fig. 5).
To complete this evaluation it’s important to perform dynamic scanning with compression of the intermetatarsal space.
Fig. 19 (video file) demonstrates this technique on a normal intermetatarsal space.

Fig. 19: Dynamic scanning technique of the normal intermetatarsal space.
With the probe on the longitudinal plane over the plantar aspect of the MTP joint, scan from side to side until you recognize the proximal phalanx (Ph) and metatarsal head (MT) of each of the adjacent rays. In between lies the intermetatarsal space (IT). Gentle compression applied by the probe on the plantar aspect of the forefoot and by the operator fingers on the dorsum of the forefoot spreads the intermetatarsal space and improves visualization of the structures within it.
Ultrasound usually depicts a well-defined hypoechoic nodule along the interdigital nerve (7) (Fig. 20),
which becomes more conspicuous and well defined during compression of the intermetatarsal space.
Fig. 21 (video file) shows the effect of compression when scanning for Morton's Neuroma.

Fig. 21: Dynamic scanning technique for Morton's Neuroma.
With the probe on the longitudinal plane over the plantar aspect of the intermetatarsal space, apply compression as illustrated in the previous video. A hypoechoic nodule (*) can be seen, corresponding to a Morton's neuroma. Notice how it becomes more conspicuous and well defined during compression.
During the scan,
we may search for Mulder’s signal. It consists of pain and a palpable click in response to lateral compression of the metatarsals,
as the neuroma pops out of the intermetatarsal space (8). Fig. 22 (video file) explains in detail how to perform the Mulder test and shows its ultrasound features.
Mulder’s signal,
however,
has been shown to have a low specificity for the diagnosis of Morton’s neuroma (2).
Fig. 22: Sonographic Mulder's sign
With the probe on the transversal plane over the metatarsal heads, lateral compression of the metatarsals is applied with the operator's nonimaging hand.
If a Morton's neuroma is present, ultrasound may show a soft tissue hypoechoic nodule (*) popping out of the intermetatarsal space, corresponding to the neuroma. The extrusion of this lesion can sometimes be accompanied by pain and a palpable click.
Cysts
Ganglion cysts are the most frequent benign masses found on the foot (5).
They are composed of mucous material,
involved by a fibrous capsule but not by a synovial membrane (2).
On ultrasound they appear as anechoic or hypoecoic masses with variable morphology,
sometimes with internal echoes or septations.
(5) Posterior acoustic enhancement is frequently present (2).
Fig. 23 shows an example of a ganglion cyst.
Plantar fibromatosis (Ledderhose disease)
Plantar fibromatosis is a benign condition which results from fibroblastic tissue proliferation on the plantar fascia.
Plantar fibromas are frequently distributed on the mid- and forefoot region and often are multiple and present on both feet (5,
9). They usually appear as a mass on the soil and most of them are painless (2).
Ultrasound shows a hypoecoic or isoechoic fusiform mass growing in the plantar fascia.
Doppler signal may be slightly increased (2,
5).
The characteristic ultrasound features of these lesions,
associated with their distribution and multiplicity,
suggest the diagnosis of plantar fibromatosis (5).
Ultrasound has advantages when compared to MRI: besides allowing easy evaluation and comparison of both feet,
the greater spacial resolution of ultrasound improves accuracy in detecting smaller lesions (2).
Fig. 24 shows examples of plantar fibromas.
Hemangiomas and Vascular malformations
A hemangioma is a usually self-limited vascular abnormality.
Vascular malformations are errors in vascular morphogenesis that grow chronically with time or acutely in response to trauma,
infection,
hemorrhage or hormonal changes.
On ultrasound these lesions have a variable appearance,
with different echogenicities (hypo-,
iso-,
or hyperechoic),
and can have solid or cystic components,
with or without detectable Doppler signal.
The presence of phleboliths is rather characteristic.
Fig. 25 shows an example of a vascular malformation on the forefoot.
When these lesions are suspected,
MRI is advised in most cases (2).
Others
A multitude of other soft tissue masses can occur on the forefoot,
such as bursitis,
lipomas,
pigmented villonodular synovitis,
giant cell tumours of the tendon sheath,
peripheral nerve sheath tumours,
aggressive fibromatosis (Fig. 26) or sarcomas.
In some cases,
ultrasound displays specific features and is the only examination needed,
particularly for superficial and smaller lesions.
In nonspecific lesions or complex,
large and deeply located masses,
ultrasound may be useful to evaluate the size,
echogenicity,
morphology and Doppler signal,
but in most instances MRI is advised for a more comprehensive characterization and differential diagnosis.