CT FINDINGS:
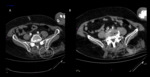
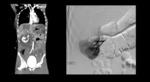
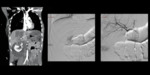
Active Contrast Extravasation
Better identified on dual-phase CT,
refers to a focal area or jet of increased attenuation within a hematoma.
The hyperattenuating area must change/enlarge on delayed images Fig. 1,
in keeping with an active bleeding[9].
Bone fragments or foreign bodies also appear as areas of high attenuation,
but don't change configuration on delayed imaging[9].
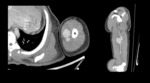
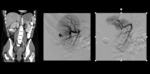
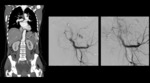
Pseudoaneurysm Formation
Refer to injury involving the media and intima vessel wall layers,
resulting in the tunica adventitia retaining blood and forming a vessel outpouching.
They have high rupture risk and result from blunt or penetrating trauma.
Pseudoaneurysms appear as rounded structures adjacent to blood vessels on non-contrast CT,
and as a focal outpouching with the same density as the blood vessel on contrast-enhanced CT Fig. 2.
Areas of mixed attenuation within the pseudoaneurysm may represent thrombus formation[15].
Aortic pseudoaneurysms are most common at the diaphragmatic hiatus and aortic isthmus and peripheral pseudoaneurysms in the femoral artery.
A ductal diverticulum/bump (remnant of the ductus arteriosus) may be confused with an aortic pseudoaneurysm as it appears as an aortic arch anterior surface outpouching[15].
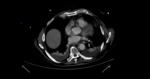
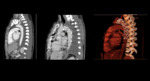
Vessel Dissection
In vascular dissection,
a tear or disruption occurs in the intima layer allowing blood flow into the media of the vessel wall.
Pathognomonic imaging finding on CT/MRI is an intimal flap,
seen as a linear defect within the contrast column crossing the blood vessel lumen.
The false lumen is usually the largest, with lower density[15]. It may become partially or completely thrombosed Fig. 3.
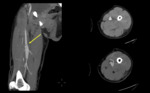
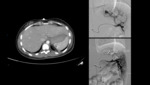
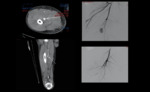
Traumatic AV Fistulas
Occurs with injury to an adjacent artery and vein pair, appearing as well-circumscribed areas of increased attenuation that persist on delayed imaging.
On CT Fig. 4 and MRI they can be identified by the early opacification of the draining/affected vein during the arterial phase[15].
INTERVENTIONS
Angiography
Angiography is indicated for hemodynamically stable patients with active bleeding on contrast enhanced CT [11,27]. Arterial access site is selected based on distance to anatomic region of interest,
vessel lumen diameter,
proximity to bone for adequate compression,
and integrity of overlying skin.
Most common access site is the common femoral artery. Seldinger technique is used for vascular access by puncturing the vessel with a hollow needle through which a guidewire is inserted into the vessel lumen.
The needle is removed over the guidewire and replaced with a catheter or sheath.
Sheaths allow catheter exchanges during a procedure.
The intravessel end is open while the outside end is capped with a hemostatic valve and a side tube for flushing.
They vary in internal lumen size (ie.
6 Fr sheath fits a 6 Fr catheter).
Guidewires vary in tip configurations and materials,
which impart different degrees of flexibility,
torque and gliding capabilities.
Sizes range from 0.010-0.038 inches in diameter and 40-300 cm in length.
Catheters also vary in inner and outer diameters,
tip configurations,
and sidehole pattern.
Outer diameter is specified in French gauge (1 Fr = 0.33mm) and end hole diameter in hundredths of an inch (ie.
0.035in).
Tip configurations are usually named by their shape (ie.
straight,
pigtail,
cobra),
intended vessel (ie.
celiac),
or designer (ie.
Simmons).
Catheter size is selected based on patient anatomy,
vessel size and possibility of stent placement or embolization during procedure.
For example,
catheterization of peripheral arteries or the celiac trunk is commonly done with a 5 Fr catheter.
Pelvic procedures might require a smaller 4 Fr catheter.
Catheters with multiple side-holes, like pigtail catheters Fig. 5,
are employed for nonselective large vessel high flow injections.
For selective injections,
smaller single-end hole catheters are used with tip configuration tailored to the target artery angle.
For example,
in Fig. 6,
a Cobra 4fr catheter was needed for selective angiography of the right kidney.
Embolization
With evolution of medical therapy and minimally invasive procedures, TAE has earned a role in non-operative management (NOM)[8]. TAE avoids the need for open surgical vessel ligation by achieving arterial occlusion and stopping active bleeding.
Organs with dual vascular supply (liver) tolerate extensive embolization,
as well as organs with multiple collateral vessels (pelvis,
gastrointestinal tract)[3].
Multiple embolic agents are available,
including Gelfoam,
coils,
particles,
sclerosing agents.
Embolic agent selection is based on vessel size,
desired permanence of occlusion,
degree of collateral flow and operator preference.
Gelfoam is an inexpensive,
temporary embolization agent which provides mechanical obstruction allowing vessel recanalization 2-3 weeks after application.
Gelfoam sponges are cut into small 1-2mm strips and loaded into a syringe.
An additional syringe is filled with sterile saline and connected via a three-way stopcock with to-and-fro motion,
allowing both to mix.
The embolic suspension is then injected through the catheter under fluoroscopic guidance until forward flow is reduced[2].
Coils are commonly used for trauma,
achieving permanent vessel occlusion by inducing thrombosis via thrombogenic fibers.
Selection of coil size according to vessel caliber is important,
to avoid forward migration,
resulting in more distal embolization.
Coils are mainly used for traumatic AV fistulas and pseudoaneurysms due to deployment precision,
thus avoiding antegrade or retrograde flow.
For pseudoaneurysms,
the sandwich technique is used,
which consists of coil embolization followed by Gelfoam slurry administration attaining both thrombosis and mechanical occlusion[8,
3,
24].
Once proximal embolization is achieved,
distal access to the vessel is no longer attainable,
therefore follow-up endovascular repair is not possible.
Particle embolization is less common in trauma, reserved for vessels smaller than the particle size (ranging from 500 to 900 um)[24] and if distal embolization is unsuccessful after coil or Gelfoam.
Particles may be released proximal to a pseudoaneurysm allowing antegrade flow to carry them past the pseudoaneurysm,
thereby reducing flow of the retrograde feeding vessels and then antegrade flow may be controlled with coils.
Sclerosing agents (absolute alcohol) are used for rapid hemostasis from multiple bleeding sites in organs that can be sacrificed (shattered kidney).
Once the sclerosing agent is injected under fluoroscopic guidance,
it is important to use additional techniques,
such as balloon occlusion,
to prevent agent reflux to non-targeted vasculature.
Stent
Management of large vessel injuries has moved to stent graft placement[8] reducing open vascular surgeries. Studies have confirmed success rate of percutaneous stent-grafting making it a practical alternative to open surgeries[18].
Benefits include: immediate patient extubation after procedure[18],
less blood loss,
decrease rate of post-procedural infections,
shorter hospital stay and lower morbidity and mortality[24,
4,6 ].
Complications include: endoleaks,
arteriotomy site hematomas,
aortic wall injury,
aneurysm formation[5],
and post-procedure infection/ inflammation.
Follow-up studies should be performed to evaluate stent graft position and rule out occlusion,
stenosis or malfunction.
Advances in stent-graft equipment and procedural techniques have considerably expanded the indications for endovascular approach in vascular trauma[16,
6] and procedural sites,
which include carotid,
femoral,
axillary/subclavian,
iliac arteries,
abdominal and thoracic aorta injuries.
Endovascular stent grafting procedure is used for large vessel vascular injuries.
Surgical planning with CT angiography (CTA) is required for anatomy evaluation,
stent measurements,
“landing zone” dimensions and access site assessment.
Endovascular stent grafting is performed at a hybrid OR/angiography suite under sedation or general anesthesia,
with a standby cardiovascular surgery team available.
Femoral surgical cut-down is required to expose the femoral artery for stent insertion.
After “landing zone” evaluation and measuring the injury site with an initial DSA run,
the stent graft is inserted and directed with the guidewire to the affected area for deployment Fig. 7.
Contrast is administered to confirm device final position.
SOLID ORGAN INJURY
Kidney
Renal injury is present 2% of trauma patients[26].
Angiography is indicated in renal trauma patients that fail non-operative management due to continued bleeding (decreasing hematocrit or persistent gross hematuria).
Complications such as pseudoaneurysms and arteriovenous fistulas are also treated endovascularly.
Embolization is indicated for segmental renal artery bleeding,
while a bleeding main renal artery should be managed surgically.
Subsegmental embolization is desired to preserve as much renal function as possible Fig. 8,
usually done by coils or sclerosing agents.
Spleen
The spleen accounts for approximately 49% of visceral injuries[10].
Angiography is performed if contrast enhanced CT demonstrates active contrast extravasation or pseudoaneurysm,
which are managed with proximal or distal embolization.
Proximal embolization preserves collateral flow thus increasing the possibility of organ preservation,
while distal embolization is mainly used in hemodynamically unstable patients in order to control extraparenchymal contrast extravasation.
Proximal embolization is achieved with coils at 2 cm after the takeoff of the first pancreatica magna artery[3,
24].
Coils should be larger than the vessel to avoid migration and distal embolization.
Coils may also be used for superselective distal embolization of a single vessel via a microcatheter,
nonetheless distal TAE is usually performed using Gelfoam Fig. 9.
Liver
The liver is in the top 3 most commonly injured solid abdominal organs in blunt/penetrating trauma. Since the liver has a dual blood supply,
early identification of active bleeding is vital.
Abdominopelvic CT with intravenous contrast has a 95% sensitivity and 99% specificity[1].
CT scan findings that are associated with hepatic vascular injury are: hemo/pneumothorax,
intra abdominal free fluid or hemoperitoneum,
right sided rib fractures,
right lung lower lobe contusions,
right kidney injury,
retroperitoneal hematoma,
adrenal hemorrhage,
among others.
Studies have validated the use of NOM as treatment of choice in all stable patients and selected unstable patients with hepatic vessel injury[8,
25,
28].
Currently most liver injuries can be treated with NOM[10,
1],
because dual blood supply makes infarction from embolization unlikely when portal vein is patent[8] Fig. 10 .
VASCULAR INJURY
Aorta
Traumatic aortic injuries are most commonly due to deceleration injuries,
occuring at the aortic isthmus,
due to shearing forces. Penetrating aortic injuries usually result in massive hemorrhage and death,
therefore are less commonly seen at the emergency room.
Acute aortic injuries include tears (type I),
intramural hematoma (type II),
pseudoaneurysm (type III) and rupture (type IV).
Management with thoracic stent-graft is preferred over open surgery for type II- IV aortic injuries Fig. 11.
There must be a suitable landing zone for the stent graft,
which means adequate distance between the lesion and a major aortic branch.
Partial or complete covering of the left subclavian artery is sometimes accepted in an emergent basis if a right vertebral artery angiography demonstrates adequate posterior cerebral circulation[13].
Pelvis
Pelvic hemorrhage is usually associated to pelvic fractures or venous disruption. Only 10-20% of cases are secondary to arterial injury[8],
most form internal iliac artery branches,
with the internal pudendal and superior gluteal arteries being the most commonly injured[8].
Contrast CT or non-selective arteriography is initially used to identify the bleeder,
followed by selective arteriography of the internal iliac arteries.
CT cystogram should be avoided prior to contrast enhanced CT/angiography to avoid confusing intraluminal bladder contrast extravasation from arterial bleeding.
TAE is accepted for pelvic active contrast extravasation,
arterial irregularity/truncation,
AV fistula or pseudoaneurysm Fig. 12.
If there is a large pelvic hematoma without active contrast extravasation,
but the patient is hemodynamically unstable,
TAE may also be performed[8].
Embolic agent selection should aim to preserve normal vessels and collateral flow,
for which Gelfoam is commonly used.
Coils are another option,
mainly for large pseudoaneurysms.
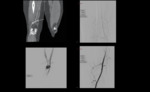
Extremity
Extremity trauma can be secondary to crush injuries,
osseous fractures,
blunt trauma,
and penetrating injuries.
Early recognition of vascular injury is of profound importance for limb salvaging,
with physical exam being sensitive and effective in predicting which patients will have negative angiographic studies [8,
7,
17].
In the past,
patients with suspected vascular injury underwent operative exploration[8],
but this has decreased with advances in minimally invasive procedures.
CTA has a sensitivity of 90% to 95.1% and a specificity of 98.7% to 100% for detection of extremity arterial injury[19].
However,
CTA also has its drawbacks in the setting of poor arterial opacification,
motion artifact,
streak artifact from adjacent metallic fragments,
or slowing of flow beyond injured sites[19].
Whenever CTA is non-diagnostic or additional evaluation is warranted, DSA should be performed[8].
Peripheral vascular injuries can be managed with stent-grafts,
balloon occlusion or embolization.
Stent-grafts are better suited for the treatment of injuries involving large vessels with a low mobility given the stent-graft susceptibility to fracture or thrombose in areas of high mobility or compression Fig. 13.