1. Patient demographics (Table 1)
The three most common indications for lung transplantation in our cohort were chronic obstructive pulmonary disease (34.6%),
interstitial lung disease (31.6%) and alpha-1 antitrypsin deficiency (7.2%).
Although cystic fibrosis was also a common indication in the younger patients.
The most frequent entity of the interstitial lung disease group was the usual interstitial pneumonia.
2.
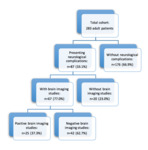
Total of neurological events and brain imaging studies (Figure 1)
In the 7-year study period,
87 patients had neurological manifestations (33.1 % of the 263 total lung transplants performed) and 67 patients (77.0 % of the 87 recipients with neurological manifestations) had brain imaging studies.
Sixty-three patients had one neurological complication,
20 had two neurological complications and 4 had three neurological complications (27.6% of the patients had two or more complications).
Twenty-five patients (37.3% of the imaged patients) had structural abnormalities on brain imaging.
The average time to a complication in our cohort was 5.8 months.
3. Spectrum of structural abnormalities on brain imaging
The clinical indications for brain imaging included focal neurologic signs (36.4 %),
encephalopathy (33.8 %),
headache (10.4 %),
seizures (10.4 %),
trauma or fall (3.9 %),
and other causes including fever and sepsis (5.2 %).
In our cohort,
the most frequent neurological final diagnosis in descending order were encephalopathy,
polyneuropathy,
strokes and seizures (Table 2).
ENCEPHALOPATHY
Alterations of consciousness and encephalopathy were common after transplantation ranging from confusion and delirium to stupor and coma.
Encephalopathy was the leading cause of neurological complication in our cohort.
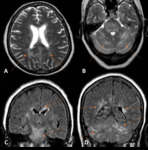
Thirty-nine patients suffered from this condition and 26 of them had brain imaging studies.
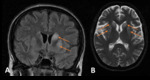
None of the CT studies revealed the underlying cause of encephalopathy,
nevertheless 2 MRI showed abnormalities.
(Fig.
2).
Drug toxicity due to tacrolimus was the main cause of encephalopathy in our cohort,
followed by cerebrovascular events.
Neurotoxicity of calcineurin inhibitors (manifested with altered consciousness,
seizures,
and cortical blindness) was more common with higher intravenous dosing in the early postoperative period.
In our cohort,
the average time after LT to encephalopathy was 1.4 months.
CEREBROVASCULAR COMPLICATIONS
Vascular complications occurred in 14 patients post-transplant and constitute the third most common neurological complication in our cohort.
Seven patients had strokes within the first week of lung transplantation.
There were two fatal cerebrovascular events (fatal ischemic strokes),
in which the duration from stroke to death was of 48 hours or less.
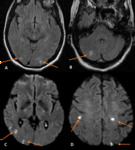
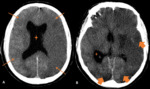
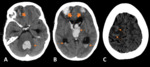
Vascular events included: five multiple cerebral emboli (Fig.
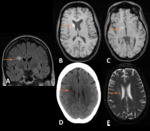
3); two watershed/hypotensive ischemic infarctions; two watershed/hypotensive ischemic infarctions with multiple cerebral emboli; two basilar artery ischemic strokes; one posterior cerebral artery ischemic stroke with intracerebral haemorrhage (Fig.
4); one middle cerebral artery ischemic stroke (Fig.
5); and finally,
one subarachnoid haemorrhage. Out of the 14 patients with cerebrovascular complications,
11 died. The average time after LT to encephalopathy was 3.5 months.
SEIZURES
Generalized seizures occurred in 8 patients.
Most commonly,
seizures presented as generalized tonic-clonic events with primary or secondary generalization.
Imaging was normal in 7 patients and revealed signs of diffuse hypoxic ischemic encephalopathy in one patient (Fig.
6).
The average time after LT to seizures was 1.9 months.
CNS MALIGNANCIES
Two patients had CNS malignancies.
A small meningioma was incidentally discovered in one male patient.
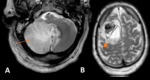
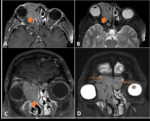
A twenty-one-year-old female patient was diagnosed with B-cell lymphoproliferative disorder affecting the orbit (Fig.
7).
The hematologic diagnosis was a Epstein-Barr virus–associated lymphoproliferative disorder,
in particular, post-transplant associated lymphoproliferative disorder.
The average time after LT to CNS malignancies was 3.1 months.
CNS INFECTIONS
It was recorded one case of CNS infection.
One female patient with disseminated cryptococcal disease had imaging evidence of CNS infection (Fig.
8).
The average time in this case was 2 months.
OTHER
Severe neuromuscular complications due to severe critical illness polyneuropathy occurred in 20 patients and constitute the second most common neurological complication in our cohort.
These patients were exposed to intravenous corticosteroids and some of them to multiple organ failure and sepsis. We observed 2 patients suffering from postoperative entrapment neuropathies related to traction and stretch injury (lower trunk brachial plexopathy).
Headache was present in 8 patients.
However,
neuroimaging studies did not reveal any abnormalities.
Two of those patients experimented severe headache as an early manifestation of neurotoxicity due to calcineurin inhibitor (tacrolimus).
Post-traumatic haemorrhage events related to accidents were found in 4 patients: 1 subdural hematoma,
1 epidural hematoma,
1 intracerebral haemorrhage with subarachnoid and intraventricular haemorrhage (Fig.
9) and 1 subarachnoid haemorrhage.