INTRODUTION
Fibromatosis is a rare mesenchymal tumor characterized histologically by proliferation of fibroblasts and myofibroblasts with marked production of intercellular collagen.
It comprises a broad group of fibrous tissue proliferations of similar histologic appearance that has biologic behavior intermediate between that of benign fibrous lesions and fibrosarcoma.
Fibromatosis was first described more than 150 years ago by McFarlane.
Because of its rarity,
most published series describe only small numbers of patients.
The incidence is estimated to be between three or four cases per million per year,
and it tends to have a female predominance.
The peak age of onset has been reported to be between 25 and 35 years,
while the majority of cases occur between puberty and 40 years.
There is a strong tendency toward local recurrence; however,
these lesions never metastasize.
The lesions have a well-circumscribed or infiltrative margin and the degree of cellularity is widely variable.
Fibromatosis can be divided into two major groups (superficial and deep) with several subdivisions by clinical presentation,
patient age,
and natural history.
CLASSIFICATION
Superficial fibromatosis arise from fascia or aponeuroses,
rarely involve deep structures.
They are usually small (<5cm),
slow-growing lesions.
Deep fibromatosis (DP) principally involve the deep muscles of the trunk and extremities (including the abdomen and pelvis) and tend to be more aggressive with a high recurrence rate.
DP are also referred to as desmoid tumours.
They are characterized a abdominal,
intraabdominal,
and extra-abdominal.
SUPERFICIAL FIBROMATOSIS
Adults
- palmar fibromatosis- Dupuytren's disease
- plantar fibromatosis- Ledderhose's disease
- knuckle pads
Children / infants
- calcifying aponeurotic fibroma/ juvenile aponeurotic fibroma
- lipofibromatosis
- infantile digital fibroma
- inclusion body fibromatosis
DEEP FIBROMATOSIS (musculoaponeurotic)
Adults
- desmoid-type fibromatosis
intra-abdominal desmoid tumours
- mesenteric desmoid tumor
- pelvic fibromatosis
- abdominal wall fibromatosis
- extra-abdominal desmoid tumours
- extra-abdominal desmoid tumour of the breast
- well-differentiated nonmetastasising fibrosarcoma
- aggressive fibromatosis
Children
- fibromatosis colli
- myofibroma
- myofibromatosis/ infantile myofibromatosis/ aggressive infantile fibromatosis
HISTOPATHOLOGIC FEATURES
The fibromatosis are a heterogeneous group of tumors with varying histologic features,
and the character of the tissue within a lesion may vary (Fig.1).
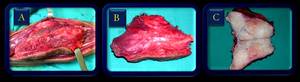
Fig. 1: (A) Macroscopic aspect of deep fibromatosis. (B) And (C) Photograph of the gross surgical specimen shows the well-defined mass.
Histologically,
the lesion consists of well differentiated collagen and fibrous tissue,
forming nonencapsulated,
poorly circumscribed masses.
The lesions have a well-circumscribed or infiltrative margin,
and the degree of cellularity is widely variable.
Because of differing clinical behavior,
DP should be differentiated from similar-appearing,
spindled tumors that have metastatic potential,
a task that can be difficult even in histologic sections.
DISCUSSION
SUPERFICIAL FIBROMATOSIS
Palmar fibromatosis
Palmar fibromatosis (Dupuytren's disease) (Fig.
2 and 3) is the most common type of fibromatosis,
with a prevalence of 1%–2% in the general population.
Older patients are most frequently affected,
with 24% of people over the age of 65 years demonstrating such lesions.

Fig. 2: Axial T1 (A) and PD fat sat (B) MRI of the wrist in a patient with Dupuytren's disease.
Palmar fibromatosis is bilateral in 42%–60% of cases.
These lesions are three to four times more common in men and are rarely seen in children.
The clinical presentation is subcutaneous nodules on the palmar surface at the level of the distal crease of the hand.
These nodules slowly progress to fibrous cords or bands that attach to and cause traction on the adjacent flexor tendons,
resulting in flexion contractures of the digits.
The fourth and fifth rays are most commonly affected,
followed by the second and third rays.

Fig. 3: MRI of the left hand. (A) Coronal T1 and (B) sagittal PD fat sat of the fi
fifth finger in a patint with Dupuytren's disease. Note the finger contracture.
Surgery is often purposely delayed owing to the high rate of recurrence (30%–40%) for lesions in the early proliferative phase.
This delay in definitive treatment may result in relatively severe flexion contractures.
Palmar fibromatosis in the proliferative phase demonstrates a high degree of cellularity.
These lesions typically mature over time with increased collagen content and reduced cellularity.
Highly collagenized lesions have a much lower prevalence of local recurrence following surgical resection.
Although these lesions have traditionally been diagnosed and treated clinically,
MR imaging has recently become valuable in planning surgical treatment.
Yacoe and co-workers correlated the cellularity of the lesions with their MR imaging appearance.
These authors reported that lesions that demonstrated intermediate signal intensity on T2- weighted spin-echo MR images were more cellular and thus more likely to locally recur.
This information may be useful in guiding the timing of surgical intervention.
If a lesion demonstrates intermediate or high signal intensity on T2- weighted spin-echo MR images,
surgery may be delayed until the lesion matures and becomes more hypocellular,
thus helping decrease the rate of postoperative recurrence.
Plantar Fibromatosis
Plantar fibromatosis (Ledderhose disease) (Fig.
4) occurs most frequently between the ages of 30 and 50 years,
with bilateral involvement seen in 20%– 50% of cases.
Concomitant palmar fibromatosis is seen in 10%–65% of patients.

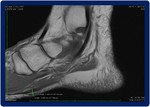
Fig. 4: MRI of the foot in a patient with plantar fibromatosis. Sagittal T1. Note the nodular area in the anterior aspect of the fascia.
These lesions develop most commonly in the medial aspect of the plantar aponeurosis.
They usually manifest as one or multiple firm,
fixed,
subcutaneous nodules,
which can extend to involve the skin or invade the deep structures of the foot.
Plantar fibromatosis is often asymptomatic until the lesion enlarges and causes mass effect or invades adjacent muscles or neurovascular structures.
Surgery with wide excision is reserved for larger,
painful lesions and those demonstrating neurovascular involvement.
Adjunctive radiation therapy may be used to decrease the rate of recurrence.
Lesions with minimal symptoms are usually treated conservatively by means of orthopedic footwear.
The typical MR imaging appearance of plantar fibromatosis is a poorly defined,
infiltrative mass occurring in the deep aponeurosis adjacent to the plantar muscles in the medial aspect of the foot.
These lesions typically have heterogeneous signal intensity equal to or less than that of skeletal muscle on both T1- and T2-weighted spin-echo MR images.
Lesions with high signal intensity on T2-weighted images reflect a more cellular lesion with relatively less collagen.
The enhancement with gadolinium contrast material is variable,
with marked enhancement seen in approximately 50% of lesions.
Juvenile Aponeurotic Fibroma
Juvenile aponeurotic fibroma is a rare,
locally aggressive fibroblastic lesion located in the palms of the hands and soles of the feet in young children.
Male patients are twice as commonly affected as female patients,
and most of the lesions manifest within the first 2 decades of life.
Juvenile aponeurotic fibroma is uncommon in older children and adults.
This type of fibromatosis is one of the few to frequently calcify and is also referred to as calcified aponeurotic fibroma.
The typical clinical presentation is a slow-growing,
asymptomatic soft-tissue mass.
Most of the lesions (67%) arise in the deep palmar fascia of the hand.
The lesions are locally aggressive and have a recurrence rate of greater than 50% following surgical resection.
Radiographs show a nonspecific soft-tissue mass,
which can demonstrate fine stippled calcifications and occasional scalloping of the adjacent bone.
Biopsy is important in evaluation of these lesions and differentiation from synovial sarcoma,
which can occur in young children,
commonly calcifies,
and may demonstrate extrinsic erosion of bone.
Infantile Digital Fibromatosis
Infantile digital fibromatosis occurs in the fingers and toes of infants.
This lesion is distinguished from other forms of infantile fibromatosis by the characteristic patient age and location and histologic identification of a specific intracytoplasmic perinuclear inclusion body.
This lesion has also been referred to as Reye tumor,
infantile digital fibroma,
and infantile digital myofibroblastoma.
Most cases (80%) are diagnosed within the 1st year of life,
and approximately 30% of cases are congenital.
The fingers are more frequently affected (60% of cases) than the toes (40% of cases).
These lesions usually manifest as single or multiple nodules involving the extensor surfaces,
most commonly the dorsal and lateral aspect of the distal or middle phalanx.
The most common treatment is surgical excision.
Spontaneous regression has been reported in approximately 8% of cases.
However,
as with other fibromatoses,
there is a high recurrence rate of approximately 60%.
Radiographs commonly show a nonspecific soft-tissue mass involving a digit with infrequent underlying bone involvement.
DEEP FIBROMATOSES
The deep group consists of rapidly growing lesions that often reach a large size and have a high tendency to recur after treatment,
hence the term "aggressive fibromatosis" (Fig 5 and 6).

Fig. 5: A young man with a palpable mass involving the left thigh. Desmoid tumor. (A) Coronal T1-WI shows that the mass has intermediate signal intensity (less than that of fat). (B) Coronal and (C) axial MR images after intravenous administration of gadolinium contrast material demontrate that the mass enhances (arrows). (D) Photograph of the gross surgical specimen shows the well-defined mass.
The course of the disease varies.
It may be fatal if the tumor infiltrates vital structures.
Local recurrences are frequent,
19 to 77%.

Fig. 6: Desmoid tumor. (A) Axial enhanced CT of the abdomen shows a large mass (arrows) anterior to the psoas muscles. (B) Photograph of the gross surgical specimen (Courtesy of Dr. Manoel Rocha, USP, SP, Brazil).
This group principally involves the musculature of the trunk and the extremities.
The term "desmoid tumor" (desmos in Greek means band),
first used by Mueller in 1838 to emphasize the bandlike or tendonlike consistency of these lesions,
is synonymous with this type of fibromatoses (Fig.
7).

Fig. 7: Male patient with deep fibromatosis of the knee. (A) axial T1WI MR image shows a heterogeneous soft-tissue mass in the popliteal fossa (arrow) with areas of low signal intensity. (B) Sagittal T1WI after intravenous administration of Gd demonstrates marked enhancement of the lesion. (C) Photograph of the surgical specimen reveals well-circunscribed mass.
Abdominal fibromatosis
Abdominal fibromatosis is a distinct entity that tends to occur in women during pregnancy or within the 1st year after delivery and in women who use oral contraceptives (Fig.
8).

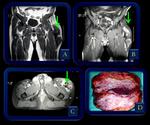
Fig. 8: (A) and (B) US images show hypoechoic lesion (arrows) with well-defined margins involving the abdominal wall in this 32-year-old woman presenting with an abdominal mass. (C) MR axial T1-weighted image of the abdomen after the administration of Gd demonstrates a well-defined mass with marked enhancement (arrow).
It involves the musculoaponeurotic structures of the abdominal wall.
The rectus abdominalis and internal oblique muscles of the anterior abdominal wall are most frequently affected.
It is similar to extraabdominal fibromatosis in gross appearance and histologic features,
but it is classified separately because of its unique patient population (young women during or following pregnancy).
Intraabdominal fibromatosis
Intraabdominal fibromatosis (IAF) (Fig.
9,
10 and 11) is histologically related to the other fibromatoses,
but it has different location and clinical manifestations.
Clinically,
macroscopically and at histology it may resemble a GIST.
Nevertheless while GISTs may often have a malignant potential,
IAF,
as for biological behaviour,
remains essentially a benign lesion.

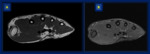
Fig. 9: Pelvic fibromatosis. (A) Axial CT of the pelvis shows homogeneous mass on the right, adjacent to the bladder. Axial MR images (B) T2-WI and (C) T1 WI demonstrate that the lesion has intermediate signal intensity (similat to muscle). (D) Axial MRI after intravenous administration of Gd demontrates marked enhancement of the mass (arrow).
IAF is divided into pelvic,
mesenteric,
retroperitoneal and intra-abdominal desmoid tumours associated with Gardner&rsquos Syndrome.
Gardner described the association of familial intestinal polyposis,
osteomas,
fibromas and epidermal or sebaceous cysts in 1951.
This is an autosomal dominant condition.

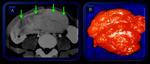
Fig. 10: Mesenteric fibromatosis. Axial enhanced CT of the abdomen shows fat-containing lesion involving the mesenteric vessels (arrows).
Although most cases of mesenteric fibromatoses are sporadic,
some are associated with familial adenomatous polyposis.
Approximately 10% of patients with this syndrome also have fibromatosis,
which typically is the intraabdominal type.

Fig. 11: Another patient with mesenteric fibromatosis. (A) Axial enhanced CT of the abdomen and (B) Axial MR T1WI demontrate a fat-containing mass surrounding the mesenteric vessels (arrows). (Courtesy of Dr.Manoel Rocha, USP, SP, Brazil).
These tumors are usually located in the small-bowel mesentery,
may cause bowel obstruction,
and frequently recur after attempted surgical resection.
Extraabdominal desmoid-type
Extraabdominal desmoid-type fibromatosis (extraabdominal desmoid,
well-differentiated nonmetastasizing fibrosarcoma,
or aggressive fibromatosis) arises from the connective tissue of muscle and its overlying aponeurosis or fascia (Fig.
12 to 21).

Fig. 12: (A) This man presented with a mass involving the medial portion of his left leg. (B) AP and (C) lateral radiographs of the left leg show a soft-tissue mass (arrow) without bone involvement.
Extraabdominal desmoid-type fibromatosis (EAF) often begins as a painless,
deep soft-tissue mass in the lower extremity,
upper extremity or the head and neck.
EAF are locally invasive and commonly recur locally but do not metastasize.

Fig. 13: – MRI (A) axial and (B) coronal post-contrast T1WI of the right shoulder reveals marked enhancement of the mass in this female patient with fibromatosis.

Fig. 14: Head and neck fibromatosis. MRI. (A) Axial T1WI shows a mass anterior to the mandible on the left side (arrows). (B) Axial T1WI after intravenous Gd administration demonstrates the strong enhancement of this lesion. (courtesy of Dr. Silvia Marçal Benício de Mello, MED IMAGEM, SP, Brazil).
Although the etiology of EAF is not known,
some associations include genetics,
hormonal status (related to pregnancy and often regressing after delivery),
and prior trauma.

Fig. 15: Extraabdominal fibromatosis in a young man. MR images of the left thigh. (A) Coronal T2WI and (B) fat-suppressed T1WI MR image obtained after intravenous administration of Gd shows that the lesion (arrows) enhances and has lobulated margins. (C) Sagittal MR image and (D) corresponding area of the lesion marked on the skin of the patient.
IMAGING FEATURES
ULTRASOUND
Sonographic findings of fibromatoses are typically described as uninodular or multinodular relatively well-defined nodules with an inhomogeneous internal structure.
The nodule(s) may be isoechoic or hypoechoic and relatively avascular,
with minimal or absent color flow within it.
The marked vascularity was associated with the more aggressive type of fibromatoses and documented by surgery.
This observation of color flow may aid in preoperative evaluation and may suggest complete resection rather than local or partial excision because the potential for recurrence may be high if incompletely removed.
COMPUTED TOMOGRAGHY
CT scans of the deep fibromatoses are also usually nonspecific.
Lesions may be hypoattenuating relative to skeletal muscle but are typically isoattenuating or even hyperattenuating.
They are generally well-defined and homogeneous.
Hyperdense areas on unenhanced scans are attributed to collagen and an abundant capillary network.
The tumors are usually better demonstrated after contrast infusion and no relationship can be established between the vascularity of the tumors and their histologic features.
The enhancement after intravenous administration of iodinated contrast material can sometimes be marked.
MAGNETIC RESONANCE IMAGING
The best imaging modality for evaluation and staging of the deep fibromatoses is MR imaging.

Fig. 16: Extraabdominal fibromatosis. Patient with a mass involving the left thigh (A). (B) Axial T1WI MRI demonstrattes an infiltrative lesion (arrows). (C) Fat-suppressed T1WI axial MRI obtained after intravenous administration of Gd shows that the mass (arrows) is intermuscular and invades
the subcutaneous fat. The mass demonstrates marked enhancement and irregular infiltrative
margins. (D) Photograph of the surgical specimen shows the infiltrative margins of the mass.
The fibromatoses display a variety of signal intensities.
In some cases with high signal intensity on T1WI.
This could be attributed to fat within the lesions.

Fig. 17: This adult male patient presented with a mass involving the left arm-pit (A). (B) Axial T1WI and (C) axial T1WI after Gd administration demonstrate a lobulated mass with strong enhancement in the axilar region. (D) Coronal MRI T1WI shows the homogeneus enhancement of the lesion (arrow). (E) Surgery and (F) Photograph of the gross surgical specimen.
On T2WI,
the majority of the fibromatosis has notably increased signal intensity,
as do the majority of other soft-tissue tumors.
Sundamam et al.
described areas of decreased signal intensity on T2WI and attributed this to acellularity and abundant collagen.

Fig. 18: Extraabdominal fibromatosis. (A) This young man presented with a mass in the anterior aspect of the right forearm. (B) Radiograph shows a soft-tissue mass. (C) MRI Sagittal T1 after the administration of Gd shows enhancement of the lesion (arrows).
The DF typically demonstrate moderate to marked enhancement after administration of gadolinium contrast material,
particularly in less collagenized and more cellular regions.
Only 10% of lesions lack significant enhancement at MRI.
Lesion margins at MRI may be well defined or infiltrative.

Fig. 19: Deep fibromatosis in a young woman who presented with a large mass on the right
thigh (A). MRI coronal images (B), (C) and (D) show the heterogeneous intermuscular lesion
(arrows).

Fig. 20: MR images (A) coronal T1WI and (B) axial post-contrast T1WI show a heterogeneous soft-tissue mass in the medial portion of the left leg (arrows) in another male patient with deep fibromatosis.
MRI can be useful for determining the response to radiation therapy or chemotherapy.
A positive response to treatment,
in which the tumor becomes less cellular and more collagenous,
is manifested by decreased lesion size and decreased signal intensity on T2WI obtained at follow-up MRI.

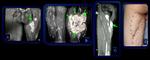
Fig. 21: (A) Photograph of the legs of a young man with a mass involving the right calf. (B) Lateral radiograph demonstrates the soft-tissue mass (arrows) without bone involvement. (C) MR Sagittal image shows a heterogeneous intermuscular mass with areas of low signal intensity involving the posterior region. (D) Photograph of the gross surgical specimen.
DIFFERENTIAL DIAGNOSIS
Benign fibrous (fibroblastic or myofibroblastic) soft-tissue tumors are a heterogeneous group of fibrous lesions with widely varied anatomic locations,
biologic behavior,
and pathologic features.
The four broad categories of fibrous proliferation are benign fibrous proliferations,
fibromatoses,
fibrosarcomas,
and fibrous proliferations of infancy and childhood.
When interpreting MR images of soft-tissue masses in adults,
radiologists should be aware of the clinical behavior,
common sites of manifestation,
and histopathologic and imaging features of the relatively common group of benign fibrous soft-tissue tumors.