Type:
Educational Exhibit
Keywords:
Kidney, MR, MR-Diffusion/Perfusion, Diagnostic procedure, Surgery, Haemorrhage, Biological effects
Authors:
H. Sahin, A. I. Biranci, A. Cakir, Y. Pekcevik, E. Kısa, Z. Kozacioglu; Izmir/TR
DOI:
10.1594/ecr2018/C-2456
Background
Partial nephrectomy (PN) is currently the treatment of choice for small renal masses to avoid the possible renal function impairment that can result from radical nephrectomy [1].
Hemostasis is a key factor during PN.
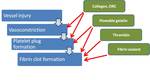
When the wall of a blood vessel is injured,
several sequential reactions occur to produce fibrin and form a stable hemostatic plug.
Those reactions involve;
(1) Vessel constriction to reduce blood flow
(2) Adherence of circulating platelets to the vessel wall at the injury site
(3) Platelet activation and aggregation under control of several enzymatic processes [2].
Hemostatic agents and tissue sealants are now being used more commonly during PN as an adjuvant to suturing.
They act by imitating,
promoting or by-passing specific steps of the coagulation cascade ( Fig. 1 ).
The most common hemostatic agents used in minimally invasive urologic surgeries are oxidized regenerated methylcellulose,
gelatin-based sealant,
glutaraldehyde-based adhesives,
human fibrinogen and thrombin fleece,
absorbable hemostatic gelatin sponge and hemostatic sealant powder [2].
In addition,
autologous perirenal fat and Hem-O-lok clips are also used to achieve hemostasis.
The different composition of those agents causes variable radiological appearances which may confound the interpretation of findings in the follow-up after PN.
We aim to review magnetic resonance (MR) imaging features associated with hemostatic agents and tissue sealants using our cohort.