The MRI protocol for testicular lesions usually includes T1-weighted sequences (with or without fat-sat),
T2-weighted sequences,
and gadolinium-enhanced T1 fat-sat sequences (all in different spatial planes).
Compared to striated muscle,
normal testes are isointense (homogeneous intermediate) at T1 and hyperintense at T2; normal testes show homogeneous uptake of contrast material.
Intratesticular lesions can be classified as benign,
malignant,
or pseudolesions.
Most solid intratesticular lesions are malignant (Table 1).
1. Benign lesions
Testicular cyst
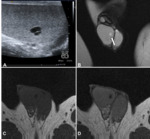
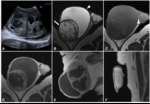
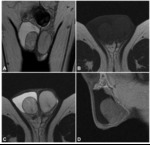
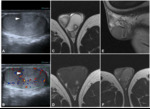
MRI findings: circumscribed lesions located within the testis itself or in the tunica albuginea that are hypointense at T1-weighted sequences and hyperintense at T2-weighted sequences. They sometimes contain proteinaceous fluid and spermatozoa (when they can be called spermatoceles) and have a fluid-fluid level (fig 1).
Epidermoid cyst
This solid benign lesion consists of a cavity filled with keratin and products of desquamation,
delimited by a single layer of squamous epithelium.
MRI findings: round,
well-delimited (with or without a capsule),
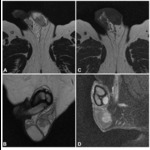
non-enhancing lesion that can be hyperintense at T1-weighted images(due to high protein contents).
At T2-weighted images,
it may have a low-intensity rim or may also show alternating rings of high and low signal (“onion ring” appearance).
Fig quiste epiderm
Imaging diagnosis of these lesions enables conservative management (enucleation),
thus avoiding unnecessary orchiectomy (fig 2)
2. Malignant testicular lesions
Testicular cancer is the most common tumor in young and middle-aged men (usually between 15-35 years).
Risk factors include cryptorchidism,
chromosomal abnormalities (e.g.,
Klinefelter),
previous or family history of testicular cancer,
and infertility.
Intratesticular cancer is divided into germ-cell tumors and non-germ-cell tumors; germ-cell tumors account for 90% to 95% of all malignant testicular tumors.
Germ-cell tumors are subdivided into seminomas and non-seminomas:
- Seminomas are more common and comprise various histologic subtypes; they are usually seen as well-defined,
homogeneous,
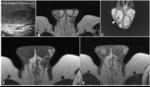
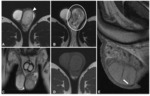
solid lesions. MRI findings: homogeneous lesions,
hypointense at T2-weighted sequences,
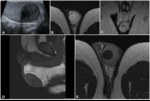
isointense at T1-weighted sequences; they may contain fibrovascular septa and may enhance after contrast administration (fig 3).
Some histological variants with aggressive component may have an heterogeneous enhancement and cystic/necrotic areas.
(fig 4)
- Non-seminomas comprise a broad group with diverse histologic types,
including embryonal carcinomas,
yolk-sac carcinomas,
choriocarcinomas,
teratomas,
etc.
At histology,
these tumors can present a single histologic type,
but more often they are a mix of different types,
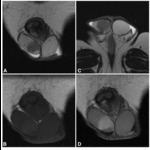
sometimes with a seminoma component as well.MRI findings: non-seminomas are usually larger than seminomas; they are heterogeneous,
with areas of necrosis/hemorrhage,
and show patchy uptake of contrast material.
(fig 5)
The imaging findings for seminomas and non-seminomas overlap,
making it impossible in some cases to differentiate between the two main types.
Non-germ-cell tumors are uncommon; this group comprises different types of lesions:
- Sex cord-stromal tumors (a group that includes Leydig cell tumor,
Sertoli cell tumor,
and granulosa cell tumor).
The most common type in this subgroup is Leydig cell tumors (1%-3% of all testicular tumors); these lesions may be classified as potentially malignant (Leydig cell hyperplasia) or as malignant (Leydig cell tumor).
It is practically impossible to differentiate between benign and malignant lesions on imaging studies
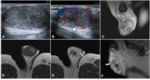
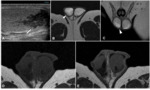
MRI findings: isointense at T1,
hypointense at T2,
with characteristic intense,
homogeneous enhancement.Because patients with these types of tumors are potential candidates for minimally invasive surgery (enucleation),
radiologic suspicion is important to avoid unnecessary orchiectomies (fig 6).
- Lymphomas account for 1% to 9% of testicular tumors; they are the most common testicular tumors in adults ≥60 years old.
They are typically non-Hodgkin lymphomas (most often diffuse large B-cell type).
MRI findings: infiltrative lesions with ill-defined margins; hypointense at T2-weighted sequences and isointense at T1-weighted sequences,
with variable enhancement (usually homogeneous or patchy in large lesions) (fig 7).
- Metastases: metastases to the testes are rare,
usually occurring in the context of disseminated disease from primary prostate,
lung,
or colorectal cancer; testicular involvement tends to be multifocal and bilateral.
- Leukemia,
sarcoma,
leiomyoma,
vascular tumors...
3. Pseudolesions
Some non-neoplastic conditions can simulate solid masses.
These are often abnormalities of vessels or of the perfusion of the testicular parenchyma: infarction,
hematoma,
orchitis,
fibrosis,
and tubular ectasia.
Tubular ectasia of the rete testis
Dilation of the seminiferous ducts located in the mediastinum testis due to partial or total obstruction of the efferent ducts.
It is seen as a multicystic elongated tubular lesion that is characteristically hypointense at T1 -weighted sequences and hyperintense at T2-weighted sequences and does not enhance after the administration of contrast material.
(fig 8).
Testicular atrophy
Unilateral or bilateral decrease in testicular size (both in diameters and volume),
testicular atrophy can be due to congenital causes (cryptorchidism is a common cause) or due to processes occurring in the past (e.g.,
ischemia,
infections,
trauma).
MRI findings: smaller than normal testis or testes; the parenchyma is hypointense on both T1- and T2-weighted sequences,
with overall hypoenhancement after the administration of contrast material.
(fig 9)
Orchitis
An infectious process involving the testes,
orchitis can be viral (in children) or bacterial (most cases of bacterial orchitis occur in sexually active men or in men older than 50 years of age with benign prostatic hypertrophy).
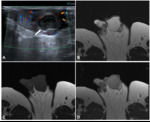
MRI findings: enlarged testis with a heterogeneous signal that is diffusely hypointense on T2-weighted sequences and slightly hyperintense on T1-weighted sequences; the involved testis has increased uptake of contrast material compared to the contralateral testis.
These findings can be associated with radiologic signs of epididymitis,
thickening of scrotal linings,
and hydrocele or pyocele,
especially in pyogenic infections,
and this is useful for the diagnosis.
This clinical syndrome can be complicated by the development of an intratesticular abscess,
which is seen as a collection within the parenchyma with moderate peripheral enhancement.
(fig 10 and 11)
Segmental infarction
Segmental infarction corresponds to an area of ischemic parenchyma in the testis; it can occur secondary to multiple causes that are not always recorded in the clinical history: infection,
trauma,
or hematologic abnormalities (e.g.,
sick-cell anemia or polycythemia).
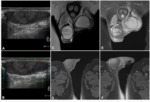
MRI findings: an isointense area in T1-weighted sequences that has a variable signal in T2-weighted sequences; characteristically,
the lesion itself does not enhance,
although a thin peripheral ring of enhancement is sometimes present.
(fig 12)
Testicular hematoma
A hematic intratesticular collection can be due to multiple causes (e.g.,
trauma or ischemic infarction) or can arise spontaneously.
MRI is very sensitive in differentiating among the different stages in the evolution of the hematoma itself.
MRI findings: a hyperintense area on T1-weighted sequences that has variable signal intensity on T2-weighted sequences.
In older hematomas,
a hypointense halo can be appreciated in the periphery.
Hematomas do not enhance after the administration of contrast material.
(fig 13)