Survey Results:
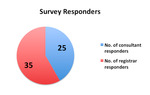
There were 60 respondents in total,
35 radiology registrars and 25 radiology consultants (Fig.5).
Overall,
consultant responders expressed a greater subjective preparedness for an MCI compared to radiology registrars.
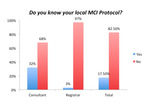
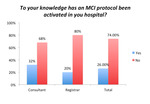
32% of consultants knew their local MCI protocol,
only 3% of registrars knew their respective protocol (Fig.6).
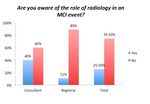
40% of consultants were aware of the role of radiology in an MCI,
compared to just 11% of registrars (Fig.7).
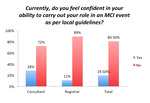
28% of consultants felt confident in their ability to carry out their role in the event of an MCI,
only 11% of registrars expressed such confidence (Fig.8).
74% of responders were unaware of a previous MCI protocol activation at their hospital (Fig.9).
Significantly,
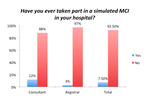
92.5% of responders have never taken part in an MCI simulation at their hospital (Fig.10).
Role of Radiology in MIP and During an MCI:
Well-designed radiology protocols will save lives in the MCI setting.
However,
imaging can be time-consuming and hamper forward flow6-9.
During an MCI,
resources are stretched and the capacity for individualized care is exceeded.
The amount or radiology required during MCIs will vary depending on the nature of the individual MCI and on the number of casualties.
The aim of MIP is to do the most good for the most people in the shortest time possible.
Unfortunately,
the role of radiology and the amount of imaging required is often underestimated in mass casualty planning and protocols7,10-13.
Diagnostic Radiology has two main goals during an MCI:
- To facilitate prompt identification of critically ill patients who require immediate intervention.
- To communicate critical imaging findings to caring physicians in a prompt and accurate fashion12,14,15.
On review of the literature,
the practical radiology approach to an MCI varies considerably6,8-11,14,15.
Some authors favour the use of a "trauma series",
of radiographs as part of the initial patient assessment6,7,11,14.
Other authors suggest initial imaging with CT only as part of triage8,9.
Whole Body Computed Tomography (WBCT) has a well-established role in imaging of the critically ill and injured patients.
The use of radiographs for initial assessment may help facilitate access to the CT scanner for critically ill patients and avoid CT "bottlenecks"7.
Many centres will employ a combination of radiographs,
ultrasound and CT in MCI response 6,7,10,11,14,15.
Issues of patient identification,
tracking and communication can also be more difficult than expected during the initial chaos of an MCI11,12,14.
Key Points to Address in Radiology MIP and MCI Protocols:1,11,14-18
Alerting Staff:
A reliable and tested communication system must be in place to alert appropriate radiology department staff of an MCI protocol activation.
Staff Roles:
Key staff roles must be adequately defined in the MCI Protocol i.e.
Clinical Director of Radiology,
Lead CT Radiologist,
Lead Porter,
Lead PACs Radiographer. Key staff role descriptions should address issues such as imaging request triaging and appropriate allocation of resources.
There should be a designated radiology department representative on the hospital disaster command committee.
Patient Identification,
Scan Ordering,
Patient Tracking:
During an MCI,
patient details may not be available e.g.
date of birth,
name etc.
Unique patient identifier systems should be in place in the Emergency Department and on PACS in order to process the rapid influx of patients accurately during an MCI.
A large influx of patients can lead to confusion and disorder in the emergency department.
Scan orders may be duplicated and scan ordering systems may not function adequately.
Most modern departments have electronic radiology ordering systems which can be time-consuming for ordering physicians.
Use of a less time intensive,
streamlined,
MCI electronic ordering system can lead to an improved patient throughput during an MCI.
Back up paper ordering systems should be in place in case of an IT failure.
MCI Scan Protocol:
A dedicated,
quick and robust WBCT protocol should be decided upon and included in the MCI protocol.
Additional sequences can be added at the CT radiologists request.
A departmental decision should be made about the radiological methodology for initial patient assessment and triage e.g.
should patients have an initial trauma series of radiographs or proceed directly to WBCT?
PACS:
MCIs can lead to a large number of scans in a short period of time.
This can lead to freezing and increased time for scan transfer to PACS.
Contingencies to address such issues should be included in the protocol e.g.
transfer 5mm slices only to PACS initially to avoid system overload.
Scan Results:
Issues regarding communication of scan results should be addressed,
i.e.
who is responsible for communicating urgent results,
how will results be communicated during a PACS failure?
A "Lead CT Radiologist",
should be in the CT control room at all times during an MCI in order to appropriately triage requests,
make necessary alterations to scan protocols,
communicate with referring physicians and provide initial "hot reports",
regarding important imaging findings.
A "Diagnostic CT Radiologist",
should dictate formal reports for PACS at a remote location and should be aware of the initial "hot report",
before finalizing dictated reports.
The use of a standardised,
checkbox,
dedicated MCI CT reporting template may help communicate results more efficiently and can act as a back up in the case of a PACS failure (Fig.11).
Department Logistics:
Instructions should be in place to cancel all non-urgent imaging once an MCI protocol is activated.
The MCI protocol should be scalable i.e.
more resources and staff should be activated for larger MCIs.
Details regarding patient tracking within the radiology department and room availability tracking should be included in the protocol.
Staffing requirements for each scanner should be specified in order to facilitate maximum throughput i.e. the number of radiographers and radiologists needed to efficiently man each CT scanner.
MCI Simulation:
MCI simulation involving all key staff as specified in the protocol is an indispensable educational tool.
Simulation allows for;
- Estimation of CT and Plain Radiography surge capacity.
Prior knowledge of rate at which scans can be completed can be used to help scale the MCI response in a more accurate fashion.
- Identification of gaps and weak points in the protocol.
- Improvement of staff knowledge regarding their role in an MCI.
- Improved familiarity with the MCI protocol and increased confidence on the part of the participating staff members to carry out their role.