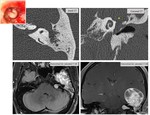
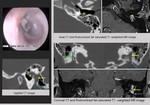
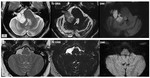
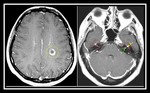
Findings and procedures
Facial Nerve Anatomy:
Supranuclear control of VII: Upper Motor Neuron (Motor Cortex).
The supranuclear contribution originates from pyramidal neurons located in the lower third of the precentral gyrus of the frontal motor cortex.
The cortical projection fibers for the upper face demonstrate an incomplete decussation and project to the ipsilateral and the contralateral facial nuclei.
However,
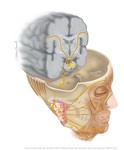
the supranuclear fibers for the lower facial muscles completely decussate to the contralateral facial nucleus (Fig.1).
The facial nerve,
from the departure point in the brainstem,
has a complex trajectory,
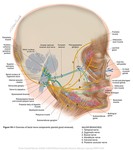
giving rise to some important nerves presented schematically in Fig 1.
All the way to the division into the terminal branches,
the facial nerve has 6 segments.
Intracranial segment:
The facial nerve starts from the pons,
from three separate nuclei attributed to each type of fibres.
a) Motor Nucleus: The motor nucleus of the facial nerve lies in the lower third of the pons,
behind the superior olivary nucleus,
and medial to the spinal tract of the trigeminal nerve.
From this origin,
the fibers first pass backward and reach the posterior end of the nucleus of the abducens nerve.
After looping around the abducens nucleus (internal genu),
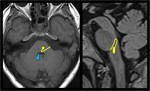
the fibers travel between the medial border of the trigeminal nucleus and the lateral edge of the facial motor nucleus (Fig.
2,
Fig.
3).
The motor fibers finally exit the caudolateral pons in the cerebellopontine angle (CPA) medial to cranial nerve VIII.
b) Nucleus Tractus Solitarius: This nucleus receives taste sensation from the anterior two thirds of the tongue,
and hard and soft palate,
travelling within the chorda tympani (Fig.
2).
c) Sensory Nucleus: The somatic sensations from the posterior aspect of the external auditory canal,
pinna,
and mastoid region travel through the nervus intermedius to the dorsal part of the primary sensory nucleus of trigeminal nerve within the pons (Fig.
2).
d) Parasympathetic Nucleus: The parasympathetic component of the facial nerve originates from the superior salivatory nucleus in the dorsal pons.
The facial nerve provides presynaptic parasympathetic fibers to the sphenopalatine and pterygopalatine ganglia for innervation of the lacrimal glands,
and to the submandibular ganglion for innervation of the sublingual and submandibular salivary glands (Fig.
2).
Cisternal segment.
After leaving the brainstem,
on the lateral side of the bulbopontine sulcus,
the facial nerve is situated in the postero-lateral area of the CPA.
At this point,
the facial nerve is on a superior position,
the intermediary is in the middle and the vestibulo-cochlear nerve is on a inferior position.
The last part of this segment can be considered a separate one: the cisternal segment.
Intracanalicular segment.
The facial nerve is in the antero-superior quadrant of the internal acoustic meatus (in the fovea facialis),
above the falciform crest.
The superior compartment is divided by a vertical crest (Bill’s bar) which sepparetes the facial nerve from the superior vestibular nerve.
At the end of this canal there is the geniculate ganglion (in the anterosuperior angle of the medial wall of the middle ear).
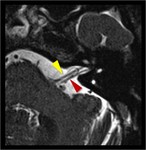
Here is the point where all the facial nerves fibers come together (Fig.
5 and 6).
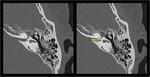
Labyrinthine segment.
This part of the nerve has an antero-posterior direction.
At the farthest point of this portion,
the segment changes direction to a 75o angle and forms the external genu of the facial nerve.
This is also where the geniculate ganglion is situated.
This is the shortest (3-5 mm) and narrowest (<0.7 mm) segment.
From the apex of the ganglion emerges the greater superficial petrosal nerve,
that contains preganglionic parasympathetic fibres that go to the lacrimal glands.
This nerve goes parallel to the anterior surface of the temporal bone.
It blens with the symphatethic fibers of the internal carotidian plexus (the deep petrosal nerve) and forms the Vidian nerve that goes through the Vidian canal (the pterygoid canal).
Inside this canal lies the pterygopalatine ganglion where the fibres synapse.
The postgaglionary fibers join the branches of the mandibular branche of the trigerminal nerve in order to innervate the lacrimal gland,
the small palatine salivary glands and the nasal cavity.
At this laberinthine segment,
the facial nerve goes between the cochlea (inferior) and the vestibule (posterior),
in the same horizontal plane with the superior wall of the vestibular cavity.
(Fig.
5,
Fig 6).
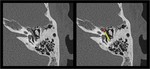
Tympanic segment.
This segment runs from the geniculate ganglion to the second facial genu,
medial to the incus.
It has a transverse direction,
running in an oblique manner from anterior to posterior and upside-down,
along the medial wall of the middle ear.
It has a superior lateral position in relation to the oval window,
and an anterior-inferior position to the lateral semicircular canal.
This segment ends in an inferior stand from the aditus ad antrum,
where it makes a second curve at a 95-125 o angle,
and becomes vertical.
(Fig.
7,
Fig.
8,
Fig.
9).
Mastoid segment.
From the second genu,
the facial nerve runs postero-medially,
along the external auditory canal,
towards the stylomastoid foramen,
where it exits the temporal bone (Fig.
9,
Fig.
10).
It contacts with the mastoid cells via the pre-mastoid slide.
At this level,
two branches emerge: the stapedial nerve that goes to the staepidian muscle in the middle ear,
and the chorda tympani nerve.
The chorda tympani nerve is actually formed by the preganglionary parasympathetic fibers that go to the salivary glands,
and the sensory fibers that go from the tongue to the solitary nucleus.
The parasympathic fibers synapse in the submandibular nucleus,
and the post gangionary fibers go to the submadibular and sublingual salivary glands.
Extracranial part.
The facial nerve leaves the cranium through the stylomastoid foramen (Fig.
10),
where it comes in contact with:
• Anterior: the base of the styloid process.
• Posterior: the occipito-temporal suture.
• Lateral: the tympanic part of the temporal bone and the mastoid process.
• Medial: the jugular fossa and the golf of the internal jugular.
It reaches the retro-mandibular fossa and has an oblique,
anterior trajectory.
Before entering the parotid gland,
the facial nerve crosses a triangular,
inter muscular space,
formed by the digastric and the styloid muscles.
Here is the place where branches for the digastrics muscle,
the stylohyoid muscle and posterior auricular emerge.
The posterior auricular fibers are responsible for the general sensitive innervations of the Ramsey-Hunt area (sensation,
temperature,
touch).
The facial nerve enters the parotid on its posterior surface.
It has a curved trajectory,
with the anterior-oriented concavity.
It runs inferior,
anterior and lateral to the inferior border of the gland,
where it becomes superficial.
The facial nerve has five terminal branches: temporal branch,
zygomatic branch,
mandibular branch,
buccal branch and cervical branch (Fig.
2).
Pathology
In this section,
we demonstrate pathologies of the facial nerve beginning medially at the facial nerve nuclei and laterally to the peripheral divisions,
in a segmental anatomical approach.
Clinically, It is possible to localise,
in some instances,
the precise level of lower motor neuron facial palsy based on the affliction of the greater superficial petrosal nerve (lacrimation),
stapedius nerve (hyperacusis),
and the chorda tympani nerve (impaired taste and salivation).
Lesions may,
therefore,
be classified as suprageniculate,
suprastapedial,
and suprachordal,
respectively.
In many instances,
however,
such localisation is not possible.
Central facial palsy is initially investigated using MRI.
Peripheral facial nerve disorders may be evaluated using high resolution CT,
MRI,
or both,
as discussed above.
Congenital Disorders.
Congenital causes are usually asymptomatic or manifest with a slight facial weakness.
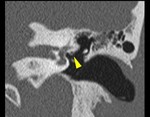
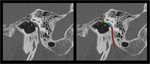
Congenital facial nerve dehiscence is a sporadic anomaly,
in which there is a bone deficiency overlying the facial nerve.
The most affected segment is the tympanic one,
superior to the oval window.
Because of the lack of bony protection,
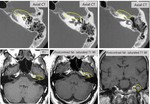
the nerve is predisposed to inflammatory pathologies (cholesteatoma otitis media) (Fig.
11).
The imaging method of choice for the diagnosis of this pathology is CT.
External auditory canal atresia (EAC) (Fig.
12) or stenosis is associated with anomalies of all elements derived from the first pharyngeal pouch: hypoplasic pavilion,
ear hypoplasy with fused or malrotated ossicles,
anterior displacement of the external genu,
of the tympanic and mastoid segments.
The stylomastoid foramen can be displaced anteriorly,
which predisposes the facial nerve to traumatic injuries.
Congenital facial paralysis is caused by certain anomalies of brainstem nuclei and appears as part of certain syndromes,
such as: Moebius,
DiGeorge,
Goldenhar,
CHARGE (colobomas,
heart defects,
choanal atresia,
mental retardation,
genitourinary anomalies,
ear anomalies),
trisomy 13,
and trisomy 18.
Congenital hypoplasia or facial nerve or aplasia can appear as isolated phenomenons or as part of a syndrome.
The diagnosis of this lesion can be performed based on 3D constructive interference in steady state (CISS) MRI sequences
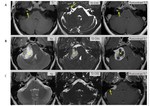
Infectious disorders.
Due to the existence of some vascular plexus surrounding the facial nerve,
there is a normal enhancement of the geniculate ganglion,
and the tympanic and the mastoid segments.
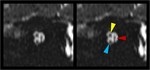
Enhancement of the cysternal,
canalicular or labyrinthic segments though,
suggests an inflammatory or infectious disease.
Infectious pathology can be of viral nature,
including the Ramsey-Hunt syndrome (varicella zoster virus),
HIV,
polio or Herpes Simplex virus.
Bacterial causes of infectious pathology include Borrelia burgdorferi, Staphylococcus,
Streptococcus,
and Mycobacterium. Possible fungal infections can be caused by Aspergillus.
Lyme disease is the most common cause of facial bilateral paralysis.
The most common inflammatory causes that may affect the facial nerve are sarcoidosis and Guillan-Barre syndrome.
The vast majority of acquired cholesteatomas (Fig.
11) develop as a result of chronic middle ear infection,
and are usually associated with perforation of the tympanic membrane.
Clinical presentation usually consists of conductive hearing loss,
often with purulent discharge from the ear.
Facial Nerve Trauma.
Fractures of the temporal bone may be associated with facial paralysis in up to 50% of cases.
Facial paralysis is usually delayed,
incomplete,
and transient.
Although any fracture of the temporal bone can result in facial nerve injury,
it is more likely to occur with transverse (38%-50% of cases) rather than with longitudinal (20%) fractures.
Immediate facial paralysis usually indicates severe nerve injury (transection),
whereas paralysis of delayed onset is usually due to an intramural hematoma.
Fractures are best demonstrated on high resolution CT.
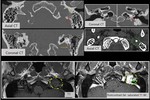
Vascular disorders.
Geniculate fossa vascular malformations affect the surrounding bone tissue,
but can also affect the canalicular segment of the facial nerve.
Lesions appear hypervascularized,
with irregular margins and avid contrast enhancement.
CT shows a bone reaction with a honeycomb appearance.
(Fig.
13).
The neurovascular compression syndrome refers to symptoms produced by the compression of the facial nerve by different vascular structures.
The antero-inferior cerebellar artery (AICA) arises from the middle segment of the basilary artery and goes towards the auditory canal,
giving birth to the labyrinthine artery.
AICA`s tortuosities and aneurysms can compress the cisternal and canalicular segments.
The persistence of the stapedial artery is a rare anatomic variant and it is caused by the lack of regression of this artery.
Usually it is associated with an aberrant trajectory of the internal carotid artery.
Rarely,
venous anomalies can affect the facial nerve canal.
The most frequent causes are: aberrant venous sinuses,
venous lakes,
and jugular bulb anomalies (Fig.
14).
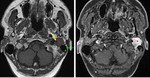
Neoplastic processes.
The facial nerve may be affected directly by primary tumors,
or secondarily by tumours arising from the temporal bone or by perineural spread of an extratemporal malignancy.
Metastasis commonly affects the petrous apex and the internal auditory meatus.
CT typically shows erosion and destruction of cortical bone,
with MRI demonstrating enhancement on contrast-enhanced T1-weighted images.
Lipomas can occur in the CPA or IAC,
entrapping unmyelinated facial nerve fibers (Fig.15).
Haemangiomas arise from the vascular plexus surrounding the facial nerve,
most commonly in the perigeniculate region.
Haemangiomas cause facial nerve dysfunction by direct neural compression or neural ischaemia due to vascular steal.
Temporal bone high resolution CT can visualize mineralisation of ossifying haemangiomas,
distinguishing these tumours from facial nerve schwannomas (Fig.13).
MRI is useful for accurate identification of schwannomas,
lipomas and haemangiomas (Fig.
13,
Fig.
15,
Fig.
17,
Fig.
18).
Malignant tumors of the parotid can affect the extratemporal facial nerve.
Primary malignant neoplasms include mucoepidermoid carcinoma,
adenoid cystic carcinoma,
adenocarcinoma,
malignant mixed tumors,
acinic cell carcinoma,
lymphoma,
and squamous cell carcinoma.
In particular,
adenoid cystic carcinoma frequently exhibits perineural spread (70-75%).
MRI with gadolinium is useful for detecting perineural spread from parotid and minor salivary gland malignancies along the facial nerve (Fig.16).
Facial schwannomas may occur along any segment of the facial nerve.
CT and MRI play an important role in evaluation of these tumors.
On MRI,
they may present as lobulated masses (when in the CPA cistern,
IAC,
tympanic segment,
and parotid space) or segments of fusiform expansion (particularly labyrinthine and mastoid segments).
Tumours in the IAC are usually indistinguishable from vestibular schwannomas.
CT best depicts the expansion,
of the bony facial canal produced by VII schwannomas.
(Fig.17,
Fig.
18,
Fig.
19)
Demyelinating disorders.
Demyelinating disorders that involve the white matter of the brain and spinal cord can also affect the facial nerve.
The active forms produce edema,
abnormal enhancement,
or reduced diffusivity.
Facial nerve involvement has been described in cases of multiple sclerosis (Fig.
20),
Guillan-Barre Syndrome and chronic inflammatory demyelinating polyneuropathy.