1 Parasitic etiology
1.1 Hydatid splenic cyst
Hydatid disease is a worldwide zoonosis caused by the larval stage of the Echinococcus tapeworm.
The outter layer of the hydatid cyst,
the pericyst,
is composed of the host cells presenting a dense,
fibrous protective layer.
It is followed by the middle laminated membrane,
the ectocyst,
and the inner germinal layer,
the endocyst,
where the parasite is produced [3].
The most common location of hydatid lesions is the liver,
followed by the lungs and the spleen,
where they most commonly migrate to by hematogenous spread.
In the spleen it is found in aproximately 2% of patients [3].
Usually,
they are asymptomatic but most frequent clinical signs and symptoms include abdominal pain,
splenomegaly and fever [4].
Ultrasound (US) and computed tomography (CT) are the most commonly used tools in clinical practice for diagnosing hydatid cysts.
Hydatid cysts in the spleen are usually solitary.
Their appearance on US examination may vary.
The wall of the cyst is usually demonstrated as a double echoic line separated by a hypoechoic layer. The cysts may be simple with no internal structures,
or with multiple echoic foci floating within.
The endocyst may be detached from the pericyst for various reasons.
It may also manifest as a multivesicular cyst with well-defined fluid collections in a honeycomb pattern with multiple septa giving the appearance of cysts within a cyst.
The lumen of the cyst may be filled with echoic material giving a mixed echoic pattern mimicing a solid mass.
A distinctive feature of hydatid cysts is calcification of the wall,
which may be partial or complete,
the latter being associated with the death of the parasite.
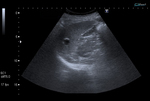
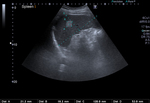
When the wall is completely calcified,
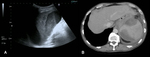
only the hyperechoic contour with posterior acoustic shadow is demonstrated by US (Figure 1).
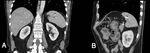
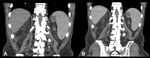
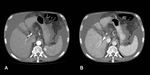
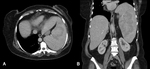
CT is indicated when US is not diagnostic or when complications are suspected.
The fluid of the cyst has water attenuation and the calcifications in the wall of the cyst are easily recognizable (Figure 2).
Even in non-calcified cysts,
the cyst wall is hyperdense on a native scan.
CT can also depict a daughter cyst [3].
Because of the risk of rupture,
splenic hydatic cysts are usually treated with partial or total splenectomy followed by albendazole therapy [5].
2 Non-parasitic etiology
2.1 Congenital splenic cyst
Congenital cysts present 10% of all non-parasitic splenic cysts.
Their histological hallmark is the presence of an epithelial lining.
They are classified into epidermoid,
dermoid and mesothelial cysts by the type of epithelium covering the surface [6].
Not only one type of epithelium can be present in a congenital cyst.
Furthermore,
the whole spectrum of cytodifferentiation from mesothelial to squamous cells has been found [7].
Therefore,
their etiopathogenesis is not yet completely understood.
One of the most supported hypotheses,
the mesothelial invagination theory,
postulates that during development there is invasion of mesothelium within the capsule and due to its pluripotent nature metaplasia and formation of a cyst is possible [6].
Usually,
they are asymptomatic but in cases of bigger cysts they can present with mass symptoms.
Most commonly,
a left upper abdominal mass and pain or epigastric pain and fullness is reported [8].
Helpful clinical findings in diagnosing an epithelial cyst are highly elevated tumor markers carbonhydrate antigen 19-9 (CA19-9) and / or carcinoembryonic antigen (CEA),
which are secreted by the epithelial lining [9].
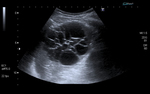
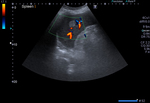
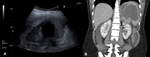
On US imaging,
they are usually found as solitary,
unilocular,
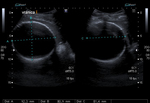
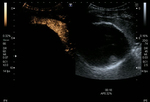
anechoic cysts with a well defined border.
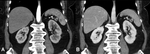
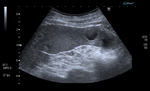
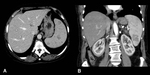
Sometimes internal echoes may be seen in the lumen (Figures 3 and 4). CT shows a hypoattenuating,
well defined lesion (Figure 5).
Calcifications of the wall may be present.
Because of their undistinctive features,
the diagnosis relies on histology.
It was shown that there is no increase in the risk for complications in larger aysmptomatic cysts,
therefore all asymptomatic congenital cysts are left untreated.
Furthermore,
it was shown that with time congenital cysts can decrease in size (Figure 6).
If they become sympomatic or the patient presents with a complication,
a partial or total splenectomy is performed [10].
2.2 Neoplastic splenic cyst
- Splenic lymphangioma
Splenic lymphangioma is a rare benign neoplasm of the lymphatic vessels that can be part of a systemic lymphangiomatous syndrome or confined to the spleen [9].
It consists of a single layer of flattened endothelium lined spaces filled with eosinophilic proteinaceous material.
Similar to haemangiomas,
depending on the size of the vascular channels lymphangiomas can be divided into capillary,
cavernous or cystic.
In the spleen,
lymphangiomas are usually microcystic and subcapsular in location.
The cysts have a fibrous wall,
sometimes with calcification within [11].
They are usually found in children and can be asymptomatic or present with abdominal pain,
mass or splenomegaly when larger in size [9].
On US they demonstrate as anechoic or hypoechoic,
multiple,
thin-walled cysts of various sizes with possible internal septations,
debris and peripheral calcifications (Figure 7). On CT they appear as well defined areas of low attenuation that do not enhance after contrast application (Figure 8) [9].
When they are larger and multifocal,
they are separated by distinct splenic tissue.
Because of presence of proteins,
fluid blood or fat,
they may also appear inhomogeneous.
Presence of curvilinear calcifications suggest the diagnosis [11].
Conservative treatment is possible in small incidentally found lymphangiomas,
although surgical resection is the preffered method of therapy [12].
- Splenic haemangioma
Splenic haemangiomas,
or slow flow venous malformations,
are the most common primary benign lesion of the spleen.
They are proliferations of the vascular channels lined with a single layer of endothelium and filled with red blood cells.
These spaces are separated by thin septa or splenic tissue and can range in size from capillary to cavernous [11].
Splenic haemangiomas are usually smaller than 2 cm and tend to be solid.
Larger cavernous haemangiomas can undergo thrombosis,
infarction and necrosis giving a pseudocystic appearance [11].
When multiple,
they can be associated with systemic syndromes,
such as Von Hippel-Lindau disease,
Klippel-Trénaunay syndrome,
Kasabach-Merritt syndrome,
or the Proteus syndrome [9,
13].
Because of their slow growth,
they are usually asymptomatic.
When symptomatic,
the signs and symptoms are non-specific,
such as pain,
splenomegaly,
a palpable mass [9].
Their appearance can vary depending on the size and the portion of solid and cystic components.
On US imaging,
the typical appearance of a well-defined hyperechoic mass is present in less than two thirds.
Other possible appearances are very variable,
including large complex masses with solid and cystic areas.
In such lesions,
absence of flow on Doppler evaluation is a helpful feature (Figures 9 and 10).
The most typical pattern of enhancement on contrast enhanced US is isoechogenicity with the spleen parenchyma in all phases,
while the peripheral globular enhancement with centripetal fill-in typical for liver haemangiomas is more rarely seen in splenic haemangiomas [14].
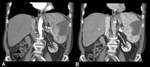
CT shows a small low-attenuation mass that fills in a centripetal pattern after contrast application and is isoenhanced to the liver parenchyma in the portal phase (Figure 11 and 12).
If they are larger and show central degenerative changes,
such as fibrosis,
infarction or thrombosis,
they may not enhance in whole and give discrete mottled areas of heterogeneous attenuation [11].
If the haemangiomas are very large,
there is a risk of spontaneous rupture and intervention is indicated.
The treatment options most commonly endorsed are arterial embolisation and partial or total splenectomy [9].
2.3 Traumatic splenic cyst
After traumatic events,
subcapsular or intrasplenic hematomas occur.
Usually,
they gradually organize and resorb or are replaced by fibrous tissue.
If they fail to organize,
they liquefy and transform into a cystic appearance.
Traumatic cysts,
or pseudocysts,
do not have an inner lining and are different from other types of cyst by having a hemorrhagic interior found at patohistology [2].
It is hard to differentiate traumatic cysts from other types of non-parasitic cysts on US imaging.
It may include some echoic foci from the debris and calcifications may be present.
On CT they appear as unilocular,
well defined,
low attenuation lesions with no contrast uptake (Figure 13) [9].
2.4 Degenerative splenic cyst
Splenic infarcts can occur from various etiologies that lead to occlusion of arterial supply or venous drainage resulting in tissue ischaemia and necrosis.
In acute infarcts,
oedema,
haemorrhage and cystic changes can be present.
As the infarct matures,
it can go to resolution,
fibrosis or liquefication,
the latter forming degenerative cysts.
Patients with acute splenic infarcts can be asymptomatic or present with left upper quadrant abdominal pain,
fever and referred pain in the left shoulder due to diaphragm irritation [9,15].
Infarcts are usually wedge,
but can also be round or irregular,
in shape.
Its appearance on US imaging is determined by the stage the infarct is in.
It can appear iso- or hypoechoic in more acute stages and hyperechoic in the chronic fibrotic stage.
If it liquefies and a degenerative cyst is formed,
it appears anechoic and well defined.
On CT,
which is the investigation of choice in the acute phase,
splenic infarcts appear as areas of heterogenous patchy enhancement in the portal phase.
Treatment with anticoagulants is aimed at preventing further infarcts and is additional to treating the underlying cause [15].
To prevent infection,
antibacterial treatment can be added in acute phases.
2.5 Malignant splenic cyst
Primary splenic mucinous cystadenocarcinoma is a very rare entity.
What is more often but still uncommonly seen are cystic metastases in widespread malignant disease or in case of splenic lymphoma.
Many cancers can metastasize to the spleen,
most frequent being melanoma.
Others include ovaries,
endometrium,
breast,
prostate,
colon,
stomach and lung.
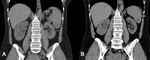
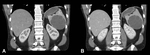
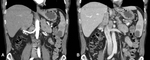
The cystic component is usually seen in a fast growing large metastasis as a result of infarction or necrosis (Figures 14 and 15).
There can also be direct progression of the tumor into the spleen (Figure 16).
Primary splenic lymphoma is rare (Figures 17 and 18).
The spleen is more commonly secondarily involved in systemic lymphoma [9].
Primary mucinous cystadenocarcinoma appears as multicystic,
multiloculated septated mass filled with gelatinous mucin,
which may give low-level internal echoes on US and higher attenuation on CT imaging.
With metastases,
the diagnosis is usually readily available.
On the other hand,
lymphoma can mimic a benign cyst with its uniform structure and therefore very hypoechoic appearance on US imaging.
Contrast enhanced US and CT imaging confirm the solidity of the lesion by showing intralesional vascularity and contrast uptake [16].
3 Complications of splenic cysts
A splenic cyst of any type can become haemorrhagic,
infected,
or can rupture due to trauma or increased intraluminal pressure.
Risk factors include a very large size of the cyst,
a focus of infection elsewhere in the body,
trauma,
recent surgery,
immunodeficiency,
intravenous drug abuse and certain haematological disorders.
It can present with left upper quadrant abdominal pain,
referred pain to the left shoulder,
fever,
nausea and vomiting.
In case of rupture and haemorrhage,
signs of peritonitis can evolve and it can lead to a hypotensive shock.
If a hydatid cyst ruptures,
an anaphylactic shock can develop.
Patients with complications of splenic cysts can therefore present with a very acute clinical picture and prompt diagnosis is essential for good patient outcome [9,
17].
Ultrasound is usually the first in line of imaging in an acutely ill patient.
On US imaging,
a splenic abscess is demonstrated as an anechoic,
hypoechoic or even hyperechoic poorly defined lesion.
If gas is formed inside the abscess,
hyperechoic areas with artefacts are present.
Doppler examination may show peripheral hyperaemia.
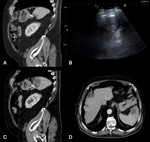
A centrally low-attenuated lesion (20 – 40 HU) is shown on CT (Figure 19).
Once a capsule develops,
minimal peripheral contrast enhancement can be seen [9].
Haemorrhagic cysts have various appearances depending on the stage of evolution of the blood products.
Therefore,
they can appear as very heteroechoic or even anechoic on an US examination [2].
Ruptured cysts with fluctuating fluid and free fluid in the abdomen can usually be well demonstrated on the US examination (Figure 20).
CT can give information on additional findings in the abdomen associated with the cause of the rupture [17].
Though percutaneous drainage of splenic abscesses has a high success rate,
definite surgical treatment is sometimes needed.
Percutaneous drainage is also very valuable as a bridge to elective surgery in unstable patients [18].
If haemorrhagic cysts get infected or are in danger of a rupture,
they can be aspirated or removed surgically.
In cases of rupture,
splenectomy is the only choice of treatment.
Whenever possible,
a partial splenectomy is preffered to preserve splenic tissue [10].