Thirty two boys and 21 girls,
aged between 3 days and 12 years with an average age of 6 ½ years.
The reasons for consultation were dominated by dyspnea and chest pain.
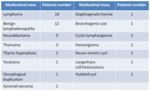
The results of our study are represented in Table 1.
The differential diagnosis of a mediastinal mass is based on identifying its location in anterior,
middle or posterior mediastinum and attenuation: soft tissue,
fat,
fluid,
enhancement and the presence or not of calcifications.
I. Anterior Mediastinal Masses
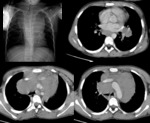
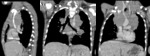
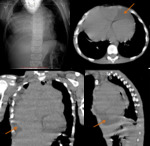
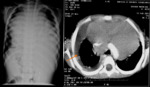
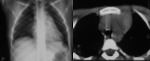
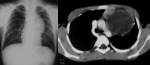
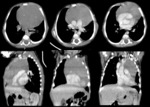
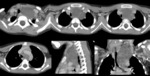
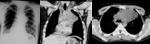
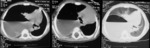
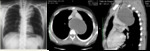
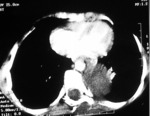
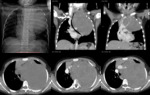
A. Lymphoma: Hodgkin and non-Hodgkin lymphoma (fig.
1-4)
Lymphoma is the most common anterior mediastinal mass in children,
with Hodgkin lymphoma occurring three to four times more frequently than non-Hodgkin lymphoma.
Calcifications or cystic areas,
due to ischemic necrosis consequent to rapid tumor growth,
can be seen.
Lymphadenopathy from lymphoma has varied appearances,
ranging from mildly enlarged nodes in a single area to large conglomerate soft tissue masses in multiple regions.
Thymic enlargement and lymphadenopathy show minimal if any enhancement after intravenous contrast.
Additional findings include airway narrowing and compression of vascular structures.
Hodgkin lymphoma in children is more common in the second decade of life.
The lymphomatous mass is most common located in the anterior mediastinum and reflects lymphadenopathy or infiltration and enlargement of the thymus.
The enlarged thymus has a quadrilateral shape with convex,
lobular lateral borders.
The CT-images of the same patient show a large soft tissue mass in the anterior mediastinum,
which arises in the thymus.
B. Thymic hyperplasia (fig.
5)
Thymic hyperplasia is another cause of thymic enlargement.
In childhood,
thymic hyperplasia is most often 'rebound' hyperplasia associated with chemotherapy,
particularly therapy with corticosteroids.
Rebound hyperplasia may be observed during the course of chemotherapy or after therapy completion and occurs 3 to 10 months after the start of chemotherapy.
The mechanism of hyperplasia is believed to be initial depletion of lymphocytes from the cortical portion of the gland due to high serum levels of glucocorticoids,
followed by repopulation of the cortical lymphocytes when the cortisone levels return to normal.
On CT,
hyperplasia appears as diffuse enlargement of the thymus,
with preservation of the normal triangular shape.
The definition of thymic hyperplasia is a > 50 % increase in volume of the thymus.
CT,
MRI of PET cannot differentiate rebound hyperplasia from infiltration of the thymus by tumor.
The absence of other active disease and a gradual decrease in thymus size on serial CT's supports the diagnosis of rebound hyperplasia.
The thymus usually returns to its normal size in 3 to 6 months.
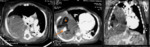
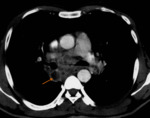
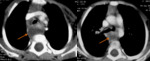
C. Thymoma (fig.
6)
Thymomas are common and account for 20% of mediastinal neoplasms.
Thymic carcinomas are extremely rare and acount for less than 1% of all thymic tumors.
The images show a thymoma on the left and a carcinoma on the right.
The thymic carcinoma has invaded the superior vena cava (arrow).
D. Langherans histiocytosis (fig.
7)
Thymic involvement in Langerhans cell histiocytosis has been reported infrequently.
However,
it probably has occurred more often than it has been recognized.
Histiocytic infiltration increases the size of the thymus,
and the thymic enlargement may be noticeable even on initial chest radiographs.
CT provides clearer depiction of the heterogeneously attenuating,
diffusely enlarged thymus.
Contrast-enhanced septa also may be seen within the thymus at CT.
The contours of the organ remain smooth and lobulated.
Punctate or serpentine calcifications are typical features but are not always present.
The calcifications may be of vascular or dystrophic origin; their exact pathogenesis is not known.
Cystic areas corresponding to focal lesions also may be observed within the enlarged thymus.
Areas of low attenuation at CT and signal hyperintensity at T1-weighted MR imaging without fat suppression correspond to areas of fatty replacement of the normal thymic tissue as a result of fibroxanthomatous reaction.
Amongst differential diagnosis of Langerhans cell histiocytosis,
we find teratomas.
The calcifications that occur in teratomas are coarse and easily detected on chest radiographs,
unlike the subtle punctuate and serpentine calcifications that occur in thymic Langerhans cell histiocytosis,
features that are visible only at CT.
E. Lymphangioma (fig.
8)
Lymphangiomas are developmental tumors of the lymphatic system.
In the mediastinum they are almost always an inferior extension of a cervical lymphangioma.
Isolated mediastinal involvement is rare.
Lymphangioma is a benign,
but aggressive tumor that shows mass effect and may encase vessels and other structures.
It typically affects infants younger than 6 months of age.
At CT it appears as nonenhancing,
thin-walled,
multiloculated mass with near water attenuation.
In children thymoma,
thymic carcinoma and goiter are so uncommon,
that you should put them very low in your differential diagnosis.
F. Synovial sarcoma (Fig.
9)
Synovial sarcomas commonly occur in the extremities of young adults.
A primary occurrence in the mediastinum is very rare with only a few reported cases in the world literature.
Mediastinal synovial sarcomas are highly aggressive tumors with a high recurrence rate and ability to progress to metastatic stage.
These neoplasms may invade adjacent organs or metastatize via the blood,
rarely via the lymphatic system.
G. Germ-cell tumors
Germ-cell tumors are the most common cause of a fat containing lesions in the anterior mediastinum and the second most common cause of an anterior mediastinal mass in children.
Approximately 90 % are benign germ-cell tumors.
Most arise in the thymus.
On CT,
a benign teratoma is a well-defined,
thick-wall cystic mass containing a variable mixture of water,
calcium,
fat and soft tissue.
The soft tissue component in benign teratoma is minimal.
Size is not an indicator of malignancy.
In our series,
the teratoma was located in the middle and posterior mediastinum (fig.
10).
Mature teratomas can be very large and still be benign.
Malignant teratomas make up 10 % of all teratomas.
They tend to have irregular or nodular walls and a predominance of soft tissue components.
They also may show pulmonary or liver metastases and chest wall invasion.
The most common non teratomatous germ-cell tumors in the pediatric population are choriocarcinoma,
embryonal cell cancer and yolk-sac cancer.
II. Middle Mediastinal masses
In the middle mediastinum we will find foregut duplication cysts or lymph nodes.
Foregut cysts in the middle mediastinum are classified as bronchogenic or enteric.
Bronchogenic cysts are lined by respiratory epithelium and most are located in the subcarinal or right paratracheal area in close proximity to the trachea or bronchus.
Enteric cysts are lined by gastrointestinal mucosa and are located in a paraspinal position in the middle to posterior mediastinum near the esophagus.
A. Mediastinal lymphadenopathy (fig.
11-12)
Mediastinal lymphadenopathy is usually caused by lymphoma or granulomatous disease.
Metastatic disease from rhabdomyosarcoma,
osteosarcoma or a Wilms tumor,
is also a possibility.
On CT,
adenopathy can appear as discrete,
round,
soft tissue masses or as a single soft tissue mass with poorly defined margins.
Calcification within lymph nodes suggests old healed granulomatous disease,
fungal infection or metastatic disease from osteosarcoma.
Areas of low attenuation suggest tuberculosis or fungal infection.
B. Bronchogenic Cysts (fig.
13)
Bronchogenic cysts are the most common intrathonacic foregut cysts.
They are most commonly located in the carnal area,
followed by paratracheal area,
then esophageal wall and retrocardiac area.
The images show a well defined lesion of water attenuation in close proximity to the trachea or bronchus,
which is typical for a bronchogenic foregut cyst.
C. Hydatid cyst (fig.
14)
Mediastinal cysts remain rare,
even in endemic countries,
which make initial diagnosis difficult.
Our case shows the importance of keeping this diagnosis in mind when a patient presents with signs of mediastinal compression.
D. Enteric foregut cyst
CT scan usually shows a well defined lesion of water attenuation in the lower mediastinum in close proximity to the esophagus,
which is typical for an enteric foregut cyst.
III. Posterior Mediastinal masses
Posterior mediastinal masses are of neural origin in approximately 95 % of cases and may arise from sympathetic ganglion cells (neuroblastoma,
ganglioneuroblastoma or ganglioneuroma) or from nerve sheaths (neurofibroma or schwannoma).
In the first decade of life they are usually malignant,
most commonly neuroblastoma.
In the second decade or life they are usually benign (ganglioneuroma,
neurofibroma,
rarely schwanoma).
A. Neuroblastoma (fig.
15-16)
Neuroblastoma typically is fusiform in shape,
of soft tissue density; 50% of thoracic tumors have calcifications.
Neuroblastoma grows over several interspaces and frequently invades the vertebral canal.
The CT-images show a calcified mass in the posterior mediastinum extending over several vertebrae,
which grows into the vertebral canal.
B. Other Neurogenic Tumors
In the 2nd decade other neurogenic tumors are seen like ganglioneuroma,
neurofibroma and rarely schwanoma.
They are round or oval in shape,
smaller in size than ganglion cell tumors and usually extend over only one or two vertebrae.
Both types of tumor may cause pressure erosion of a rib and invade the spinal canal.
C. Diaphragmatic hernia (Fig.
17)
1. Bochdalek Hernia
Hernias through the foramen of Bochdalek are developmental defects in the posterior part of the diaphragm.
These hernias are usually diagnosed in infants who present with clinical symptoms of pulmonary insufficiency.
The herniated contents contain fat and omental tissue in a majority of cases,
but other retroperitoneal and intraperitoneal structures can infrequently be involved.
CT usually demonstrates fat above the diaphragm and is extremely beneficial in revealing organ entrapment.
Coronal and sagittal reformatted images show the defect to best advantage.
2. Morgagni Hernia
Hernias through the foramen of Morgagni are not usually diagnosed until adulthood.
The underlying developmental defect allows herniation of abdominal contents between the fibrotendinous elements of the sternal and costal portions of the diaphragm.
The defect is anterior and retrosternal in location and is usually a right-sided process (90% of cases).
The contained abdominal contents may include,
in order of decreasing frequency,
the omentum,
colon,
stomach,
liver,
and small intestine.
Morgagni hernia can be associated with trauma,
severe effort,
and obesity.
Sagittal and coronal reformatted CT images are often helpful in demonstrating the diaphragmatic defect and identifying the contents of the hernia.
3. Hiatal Hernia
Hiatal hernias may be sliding or,
much less commonly,
paraesophageal.
Sliding hernias involve cephalic displacement of the esophageal junction through the esophageal hiatus into the posterior mediastinum.
Paraesophageal hernias involve protrusion of the stomach into the thorax through the esophageal hiatus.
The stomach is usually anterior to the body of the esophagus and posterior to the pericardium.
CT helps verify migration of the stomach cranially through the hiatus.
Sagittal and coronal reformatted images often help demonstrate the hernia and the hiatal defect.
D. Oesophageal duplication (fig.
18)
Esophageal duplication cysts are usually located along the esophagus in the lower posterior mediastinum.
Duplication of the oesophagus has a range of macroscopic appearances,
ranging from complete (which is very rare) to partial cystic duplication (oesophageal duplication cyst).
It is the second most common gastrointestinal tract duplication after that of the ileum.
On CT scan,
duplication cysts appear as is sharply marginated masses with homogeneous fluid density.
No enhanced after intravenous contrast administration is visible.
E. Neurenteric Cyst
Neurenteric cysts are the least common type of foregut cysts.
They communicate with meninges and are associated with spinal dysraphism,
butterfly vertebrae on hemivertebnae,
and scoliosis.
F. Extramedullary hematopoiesis
Extramedullary hematopoiesis accounts for less than 0.1 % of the lesions in the posterior mediastinum.
It is characterized by formation of blood elements outside of the bone marrow.
It occurs with severe anemia.
On CT it is seen as a paravertebral mass and occurs with coarse bone trabeculation in the adjacent vertebra.
IV. How helpful is CT scan?
Mediastinal masses in children may represent congenital anomalies,
infections,
and benign and malignant neoplasms.
Pseudomasses can pose diagnostic challenges to the unwary eye.
In both asymptomatic and symptomatic children with mediastinal masses,
CT scan plays a paramount role by providing precise information regarding location,
appearance,
size,
and relationship to the adjacent mediastinal structures as well as detecting metastases.
Knowledge of the practical diagnostic imaging approach based on the three mediastinal compartments and the characteristic imaging appearances can lead to a correct diagnosis and subsequent optimal management.
A. Location (fig.
19)
B. Density
Density on CT scan may be helpful in the anterior mediastinum masses:
- Soft tissue: lymphoma and thymic hyperplasia.
- Fat: germ cell tumor,
thymolipoma.
- Water density: lymphangioma.
and the middle mediastinum masses:
- Low attenuation: tuberculosis,
fungal.
- Calcified: tuberculosis,
fungal,
osteosarcoma.