CT IMAGING TECHNIQUE
CT examinations from the domes of the diaphragm to the symphysis pubis with 2.5 mm collimation,
2.5 mm intervals,
at 120kV were obtained on multidedector CT scanner (GE,
Medical Systems,
Milwaukee,
Wis,
USA).
All patients received 1250ml of diluted (3%) water with soluble contrast material orally,
periodically over 1.5hr before the scan and in addition to that,
250ml just before the study,
to opasify the stomach,
small bowel and colon.
Non-opasificed bowel loops may be a source of diagnostic error that can simulate soft tissue masses.
After an unenhanced scan of the upper abdomen,
a contrast- enhanced scan of the upper abdomen covering the entire liver in the early arterial and the portal venous phase was performed,
followed by a The arterial phase scan was initiated 4 seconds after the contrast bolus [100 ml Iopromide (Ultravist,
Berlin,
Germany) followed by 40 ml saline; flow,
4 ml/s] arrived at the aorta (bolus tracking; resulting total delay approximately 20 seconds).
Portal venous phase scanning was initiated with a 40 seconds delay,
the delay for the venous phase was 80 seconds.
MR images were obtained with a 1.5 -T system (Signa Horizon Echo Speed; GE Medical Systems,
Milwaukee,
WI,
US) in 3 cases,
and with a 3T MRI scanner (Verio,
Siemens Healthcare,
Erlangen,
Germany) using a standard liver MRI protocol in two patients.
Axial-coronal-sagittal routine T1-weighted,
T2-weighted images,
and fat-suppressed T1-weighted,
opposed-phase T1-weighted images,
and diffusion weighted imaging (DWI) were acquired before contrast administration.
Dynamic contrast enhanced hepatobiliary phase imaging is performed after gadoxetic acid infusion with body coil.
PATIENTS
We retrospectively reviewed CT and MR images of 5 surgically and histologically proved intraabdominal liposarcomas between January 2012 and August 2017.
Two patients were male,
and three was females,
with age ranged from 44 to 53 years,
mean 47±1.6-year-old.
CT and MR imaging findings of all of the patients were correlated with histopathologic subtypes.
Histopathological findings of all tumors were reviewed for diagnosis and classification of histologic subtypes.
An intra-abdominal primary site was present in 4 of 5 patients with liposarcomas.
two patients were male,
and three was females.
The histologic subtypes of the liposarcomas were as follows: one well differentiated,
three myxoid liposarcoma,
and one was dedifferentiated liposarcoma (Table 1).
45-years old male case had one solid lesions with the diameter’s of 1x1.5cm,
on dynamic series heterogeneous contrast enhanced liver metastases and histopathologic diagnoses of this case was well-differentiated liposarcoma.
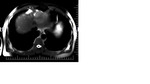
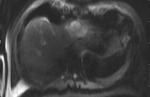
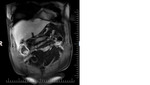
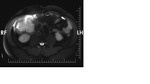
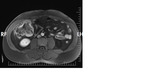
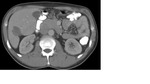
47-years old female case,
had three hepatic solid lesions (the biggest one’ diameter is 5x4cm),
on dynamic series diffuse contrast enhanced liver metastases and histopathologic diagnoses of this case was myxoid liposarcoma (Figure 1-3).
63-years-old female case had one semisolid lesion with the diameter’s of 5x4cm,
on dynamic series peripheral heterogenous type contrast enhancement is detected.
Histopathologic diagnoses of this case was myxoid liposarcoma (Figure 4-5).
53-years-old male case had multiple semisolid lesions (the biggest one’ diameter is 3x4cm),
on dynamic series peripheral ring type contrast enhancement is detected.
Histopathologic diagnoses of this case was myxoid liposarcoma.
48-years-old male case had multiple cystic lesions the biggest one’ diameter is 2.5x4cm),
on dynamic series minimal peripheral contrast enhancement is detected.
Histopathologic diagnoses of this case was dedifferentiated liposarcoma (Figure 6).